Lisa A. Simpson, MSc, OT1,2, Janice J. Eng, PhD, PT1,3, Tara D. Klassen, MSc, PT1,2,3, Shannon B. Lim, MSc1,2, Dennis R. Louie, BSc, PT1, Beena Parappilly, MSc, RN1,2, Brodie M. Sakakibara, PhD1,3 and Dominik Zbogar, MSc1,2
From the 1Rehabilitation Research Program, GF Strong Rehabilitation Centre, 2Graduate Program in Rehabilitation Sciences and 3Department of Physical Therapy, University of British Columbia, Vancouver, Canada
OBJECTIVE: It is important for older adults to be physically active, but many older adults walk slowly. This study examined the accuracy of a commercially available step-count device (Fitbit One) at slow speeds and compared the accuracy of the device when worn at the ankle and waist in older adults.
METHODS: The Fitbit One was placed at the ankle and waist of participants (n=42; mean age 73 years) while they performed walking trials at 7 different speeds (0.3–0.9 m/s). Step counts obtained from video recordings were used as the gold standard comparison to determine the accuracy of the device.
RESULTS: The ankle-worn device had significantly less error than the waist-worn device at all speeds. The percentage error of the ankle-worn device was less than 10% at speeds of 0.4–0.9 m/s and did not record zero steps at any speed. The percentage error of the waist-worn device was below 10% at only the 2 fastest speeds (0.8 and 0.9 m/s) and recorded zero steps for numerous participants at speeds of 0.3–0.5 m/s.
CONCLUSION: The Fitbit One can accurately capture steps at slow speeds when placed at the ankle and thus may be appropriate for capturing physical activity in slow-walking older adults.
Key words: physical activity; measurement; pedometer; older adults.
J Rehabil Med 2015; 00: 00–00
Correspondence address: Janice Eng, Department of Physical Therapy, University of British Columbia, Vancouver, V6T 1Z3, Canada. E-mail: janice.eng@ubc.ca
Accepted May 12, 2015; Epub ahead of print Jul 15, 2015
INTRODUCTION
The benefits of regular physical activity for older adults and those with chronic disease and/or mobility limitations are indisputable. Regular physical activity attenuates many of the health risks associated with obesity (1), cardiovascular disease (2), diabetes (3), depression and anxiety (4), and cognitive decline (5). As physical activity levels among older adults (both with and without chronic disease) are low (6), facilitating an increase in activity levels is an important public health issue. Many governments have produced physical activity guidelines for older adults that emphasize walking activities as an ideal means of low-impact, low-risk physical activity that most people find pleasurable (4, 7).
Step-count devices (i.e. pedometers and accelerometers), which provide instantaneous feedback, are increasingly being used to monitor physical activity and motivate older adults to increase their level of walking activity (8, 9). Strong relationships have been observed between step counts and accelerometer-determined activity, moderate to vigorous physical activity and sedentary activity (10). Moreover, the simplicity of step counts makes it an ideal measure for interpreting, comparing and setting physical activity targets. Numerous studies have examined the accuracy of various step-count devices. The accuracy of a number of pedometers and accelerometers has been established at speeds greater than 0.9 m/s (11). In contrast, studies have consistently shown poor accuracy (or even recordings of zero) of these devices at speeds less than 0.9 m/s (12–14). Accurately capturing steps at slower walking speeds may enable many more people to utilize step-count devices, especially those who walk slowly. Slow walking is associated with individuals who have frailty, chronic disease, and/or mobility limitations (15); these are ideal groups who would most benefit from encouragement to increase their activity levels. Walking is also a major goal for older adults undergoing rehabilitation (16). A device that can accurately capture steps at slower walking speeds may assist health professionals to create and monitor walking activity goals. Furthermore, individuals vary their speed throughout the day, depending on the task and environment (e.g. walking slower inside the house vs faster outside on a sidewalk; faster at beginning of walk vs slower at end of walk if fatigued). Therefore identifying a device that accurately captures steps at a variety of slower walking speeds is important.
An increasing number of accelerometers that provide instantaneous feedback are now commercially available. The recommended attachment location for these step-count devices is the waist or wrist. One study found that the number of steps captured by a wrist-worn accelerometer consistently captured fewer steps than a waist-worn accelerometer during treadmill walking at speeds ranging from 0.2 to 3.1 m/s (17). Another study in older surgical patients suggested that sensitivity could be improved for slower walking speeds when the step-count device was positioned at the ankle, but the accuracy was not evaluated (18). High accelerations at the ankle may make an ankle-positioned device an appropriate solution for increasing the accuracy of a commercially available step-count device at slow walking speeds. Thus the objectives of this study are: (i) to systematically examine the effect of walking speed on the accuracy of a commercially available device (Fitbit One) at slower walking speeds (≤ 0.9 m/s) in older adults; and (ii) to examine the effect of position (waist vs ankle) on the accuracy of this device. This study is the first step in assessing the accuracy of the Fitbit One device during slow continuous walking.
METHODS
Participants
Volunteers were recruited through flyers posted at multiple community locations (i.e. community centres, grocery stores, coffee shops) and through word of mouth. Volunteers were eligible for inclusion if they were over the age of 65 years and able to walk independently for at least 30 m with or without an assistive device. They were excluded if they had a major medical condition that affected their ability to walk (e.g. multiple sclerosis, stroke, Parkinson’s disease) or had had major surgery in the past 12 months (e.g. hip replacement, heart surgery). The University of British Columbia’s clinical research ethics board provided approval for this study and all participants provided informed written consent.
Device
The Fitbit One (Fitbit) (Fitbit Inc., San Francisco, CA, USA) was used for the study. The Fitbit contains a triaxial microelectromechanical accelerometer and uses proprietary algorithms to convert acceleration into step counts. The algorithm was designed to detect motion patterns most indicative of walking. The proprietary algorithm also includes a threshold that must be surpassed for a motion and its associated acceleration to be counted as a step. The manufacturer recommends wearing the Fitbit at the waist, pocket, wrist or attached to a bra. The number of steps taken is provided instantaneously by pressing a small button on the device. The Fitbit is lightweight (8 g) and small (4.8 × 1.9 × 1.0 cm). The Fitbit also captures distance travelled, stair counts and calories burned. Fitbit output can be wirelessly synced to a compatible smartphone or tablet.
Procedure
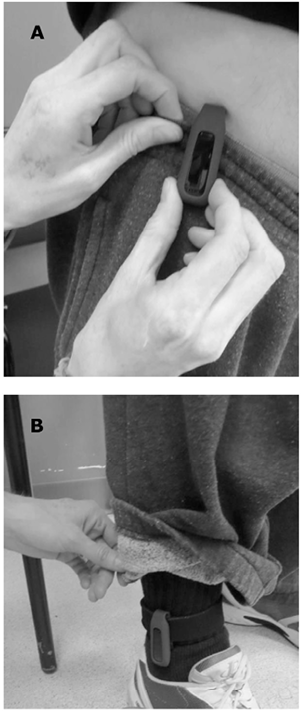
Participants attended a single testing session. Demographic information was obtained and then 2 Fitbits were attached to the participants’ right side at the following locations: (i) on the waistband, just above their greater trochanter (Fitbit – Waist), and (ii) on the ankle, just above the lateral malleolus (Fitbit – Ankle). Fig. 1 shows photographs of the Fitbit at the waist and ankle attachment locations. Participants walked a distance of 15 m for 8 different walking trials: 1 at their self-selected speed and 7 trials at speeds of 0.3–0.9 m/s in increments of 0.1 m/s. For the 7 speed trials, participants were instructed to walk directly beside a pace-setter (trained research assistant). Walking trials were repeated if the participant was not able to walk directly beside the pace-setter. The pace-setter used visual (markings on the floor) and auditory (metronome beats via earbuds) cues to maintain the intended speed. The step count on each device, which was obtained by pressing a button on the display, was recorded at the beginning and end of each walking trial. The order of the 7 walking trials was randomized for each participant, and each trial was video-recorded. Two independent viewers counted the actual number of steps from the video-recordings of each trial (considered gold standard). If there was greater than 1 step difference between the 2 viewers, a third viewer watched the video pertaining to the walking trial in question and consensus was reached on the step count. Video step counts from 1 viewer were randomly selected and used in the analysis when step counts were 1 step apart.
Data analysis
The accuracy of the Fitbit at each speed was assessed in 2 ways: (i) percentage error, which compared the actual steps recorded on the video (Actual) with steps recorded on the Fitbit (Fitbit). The percentage error for each individual was calculated using the following equation: ((Actual steps – Fitbit steps)/Actual steps) × 100); (ii) Visual analysis using Bland–Altman plots to examine the mean differences between the Actual steps and the Fitbit steps and the 95% limits of agreement (i.e. the interval within which 95% of the differences between Actual and Fitbit steps are expected to lie) (19). Separate plots were created for each speed and attachment location. Small mean differences and narrow limits of agreement indicate greater accuracy. The calculated percentage error values and Bland Altman plots for the ankle were compared with those of the waist to examine the effect of location on the accuracy of the Fitbit. In addition, paired t-tests comparing the percentage errors of the 2 Fitbit placements (Ankle, Waist) were used to further compare the accuracy at the different placements. Bonferroni-adjusted p-values for multiple comparisons are reported.
RESULTS
A total of 42 volunteers participated in this study. Participant characteristics are outlined in Table I. In summary, the mean age of the participants was 73 (± 6.9) years and the mean self-selected walking speed was 1.07 (range 0.54–1.69) m/s. Two-thirds of the sample had known medical conditions. High blood pressure, diabetes, and thyroid disorders were the most prevalent conditions. Percentage agreement between the independent video viewers ranged from 88% to 100% (Table II). In addition, participants were able to walk directly beside the pace-setters for all walking trials. The pace-setter protocol resulted in the participants being within 99% of the assigned speeds (Table II).
|
Table I. Participant characteristics (n=42) |
|
|
Variables |
|
|
Age, years, mean (SD) |
73 (6.9) |
|
BMI, mean (SD) |
26.1 (4.6) |
|
Males, n (%) |
11 (26) |
|
Known medical conditionsa, n (%) |
28 (67) |
|
Self-selected gait speedb, mean (SD) [range] |
1.07 (0.24) [0.54–1.65] |
|
Walk with assistive devicec, n (%) |
1 (2) |
|
aThree most prevalent conditions: high blood pressure, diabetes, and thyroid disorders. bGait speed in m/s. cCane. |
|
|
Table II. Accuracy of the Fitbit device at varying walking speeds |
|||||||||
|
Assigned speed (m/s) |
Actual speed Mean (SD) |
100% agreement between video raters (n) |
1 step difference between video raters (n) |
Fitbits recording zero counts – Ankle (n) |
Fitbits recording zero counts – Waist (n) |
Actual steps Mean (SD) |
Fitbit – ankle Mean (SD)/ % error (SD) |
Fitbit – waist Mean (SD)/ % error (SD) |
p-valuea |
|
0.3 |
0.30 (0.01) |
37 |
5 |
0 |
40 |
49 (5) |
43 (12)/ 14.5 (19.8) |
1 (4)/ 98.4 (11.1) |
<0.001 |
|
0.4 |
0.40 (0.01) |
40 |
2 |
0 |
30 |
41 (3) |
41 (4)/ 5.9 (5.9) |
7 (13)/ 82.0 (31.7) |
<0.001 |
|
0.5 |
0.50 (0.01) |
40 |
2 |
0 |
10 |
35 (3) |
36 (3)/ 4.1 (4.5) |
21 (13)/ 40.4 (36.9) |
<0.001 |
|
0.6 |
0.60 (0.02) |
42 |
0 |
0 |
2 |
33 (3) |
34 (4)/ 3.2 (3.9) |
26 (8)/ 21.6 (23.7) |
<0.001 |
|
0.7 |
0.70 (0.02) |
41 |
1 |
0 |
1 |
32 (2) |
32 (3)/ 2.5 (2.3) |
28 (5)/ 10.5 (16.0) |
0.003 |
|
0.8 |
0.80 (0.03) |
41 |
1 |
0 |
0 |
30 (2) |
30 (3)/ 2.8 (2.9) |
28 (2)/ 7.0 (5.3) |
<0.001 |
|
0.9 |
0.89 (0.03) |
38 |
4 |
0 |
0 |
28 (2) |
29 (3)/ 2.8 (3.3) |
27 (3)/ 5.6 (4.6) |
0.004 |
|
aComparison between Fitbit – Ankle and Fitbit – Waist % error. Bonferroni adjusted p-values reported. |
|||||||||
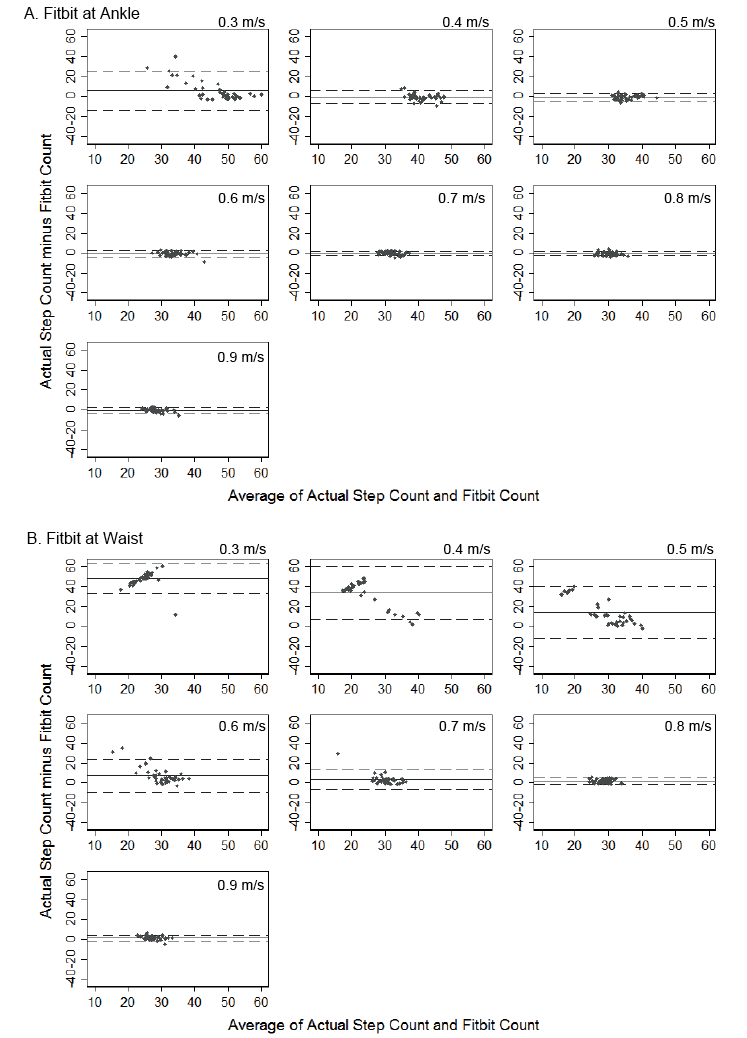
The Fitbit – Waist recorded zero step counts for some participants at all but the 2 fastest speeds (0.8, 0.9 m/s) (Table II). This means that after walking 15 m at all but 0.8 m/s and 0.9 m/s, the Fitbit – Waist monitor did not record any steps for some participants. At speeds of 0.3, 0.4, 0.5, 0.6 and 0.7, the number of participants recording zero steps was 40, 30, 10, 2 and 1, respectively. This is in contrast to the Fitbit – Ankle, for which no participants recorded zero step counts at any speed. The percentage error for both the Fitbit – Ankle and Fitbit – Waist decreased from their highest at the slowest speed (0.3 m/s) to their lowest at the fastest speed (0.9 m/s). The percentage error for the Fitbit – Ankle was below 5% for all but the 2 slowest walking speeds (0.3, 0.4 m/s), whereas the percentage error for the Fitbit – Waist never fell below 5% (Table II). The error of the Fitbit – Ankle was found to be significantly lower than the error of the Fitbit – Waist at all speeds (Table II). Finally, the mean differences (i.e. absolute error) between the Actual steps and Fitbit steps in the Bland–Altman plots for the ankle placement approached zero at all speeds except 0.3 m/s (Fig. 2A). This is in contrast to the Fitbit – Waist plots, which show the mean difference close to zero only at faster speeds (0.8, 0.9 m/s) (Fig. 2B). The limits of agreement for the Fitbit – Ankle were also narrower than the limits of agreement for the Fitbit –Waist at all speeds (Fig. 2A, B; Table III).
|
Table III. Bland–Altman mean differences and limits of agreement for each speed and location |
|||||
|
Speed (m/s) |
Fitbit – Ankle |
Fitbit – Waist |
|||
|
Mean difference |
Limits of agreement |
Mean difference |
Limits of agreement |
||
|
0.3 |
5.7 |
–13.5 to 25.0 |
48.0 |
33.4 to 62.7 |
|
|
0.4 |
–0.7 |
–5.6 to –7.0 |
33.4 |
7.2 to 59.6 |
|
|
0.5 |
–0.7 |
–4.3 to 2.3 |
14.2 |
–11.5 to 39.3 |
|
|
0.6 |
–0.6 |
–3.8 to 2.5 |
7.1 |
–9.2 to 23.4 |
|
|
0.7 |
–0.3 |
–2.3 to 1.7 |
3.3 |
–6.3 to 12.9 |
|
|
0.8 |
–0.3 |
–2.6 to 1.4 |
2.0 |
–1.6 to 5.5 |
|
|
0.9 |
–0.4 |
–2.9 to 2.1 |
1.4 |
–1.6 to 4.3 |
|
Fig. 2. Bland–Altman plots at the assigned walking speeds when positioned at: (A) waist and (B) ankle. Solid lines: mean differences between Actual and Fitbit step counts. Dashed lines: limits of agreement.
DISCUSSION
This study examined the accuracy of a commercially available step-count device at slow walking speeds (0.3–0.9 m/s) and compared the accuracy of this device at 2 different attachment locations (Ankle and Waist). Our findings suggest that the Fitbit One is more accurate at speeds below 0.9 m/s when placed at the ankle than when placed at the waist. The ankle-worn Fitbit can capture steps with 5% or less error at speeds as slow as 0.5 m/s. The walking speeds used in our study are typical gait speeds for frail older adults and those with chronic disease and/or disability. For instance, a systematic review by Peel et al. (20) reported gait speeds of 0.11–0.86 m/s from 7,000 older adults in hospital settings (i.e. acute or rehabilitation care); Giuliani et al. (21) reported a mean gait speed of 0.41 m/s among 1,791 individuals in residential care and Tavassoli et al. (22) reported a mean gait speed of 0.78 m/s among 1108 older adults referred to a Geriatric Frailty clinic.
The accuracy of the Fitbit – Ankle was superior to that of the Fitbit – Waist at all speeds. The ankle-worn Fitbit was able to pick up the majority of steps at the slowest speeds (0.3 and 0.4 m/s) compared with the waist-worn Fitbit. In addition, at 0.3 m/s and 0.4 m/s, the waist-worn Fitbit only counted steps for 2 and 12 participants, respectively. The accelerations at the hip at these speeds were probably not large enough to surpass the Fitbit’s required acceleration threshold. At 0.9 m/s, however, the difference between the device placements was minimal (< 3.0%) and thus either location is acceptable at this speed. The greater accuracy of the ankle-worn Fitbit at all speeds is probably due to the higher accelerations at the ankle during the swing phase of the foot. Indeed, one study examined power generated at different joints at a range of gait speeds that included 0.3–0.8 m/s, and found the power generated at the ankle was larger than the power generated at the hip at all speeds within this range. The relative difference, however, (i.e. ankle power/hip power) fell from 4 times at 0.3 m/s to 2.8 times at 0.8 m/s (23). The waist-worn Fitbit has been tested at higher speeds in young adults and shown to be accurate from 0.9 to 1.8 m/s (24). Interestingly, 10 participants walking at 0.5 m/s did not record any steps with the waist-worn Fitbit, while the other 32 individuals did record steps at the waist. Thus, a participant’s specific gait pattern (e.g. step length, cadence, swing pattern) may influence whether the device will record.
The manufacturer recommends wearing the Fitbit at the waist. We found, however, that the accuracy of the ankle-worn Fitbit is superior to other waist-worn step-count devices at slow speeds. Percentage error for other devices at slow speeds are: 75% error for the Yamax at 0.4 m/s (12); 48–59% error for the Omron at 0.46 and 0.58 m/s, respectively (25, 26)and 72% error for the New Lifestyle at 0.46 m/s (26). These values contrast to the 5.9% error for the Fitbit at the ankle at 0.4 m/s. The accuracy of the ankle-worn Fitbit at higher walking speeds, as well as while running still needs to be established, but is less relevant for the older adult population. The ankle-worn Fitbit device may overestimate steps at higher speeds and this may be the reason why the ankle is not a recommended attachment location.
The novel pace-setter paradigm allowed us to assess the accuracy of the Fitbit at a variety of speeds without constraining participants’ cadence or step length. Previous methods have used treadmills or metronomes to pace the participants, which alter a person’s natural gait pattern (27). Our pacing approach is simple, replicable and resulted in an almost perfect match between the participant’s speed and the assigned speed. In addition, the task of walking beside a pace-setter is similar to a typical activity (i.e. walking with a companion) that older adults may perform on a daily basis.
The Fitbit device is readily available to consumers. While the output is difficult to read at the ankle, the device has an interface that permits the data to be read on a mobile device. Step-count devices that provide instantaneous feedback are a promising method for increasing physical activity among sedentary older adults with or without mobility limitations who walk slowly. Indeed, systematic reviews of intervention studies have concluded that the use of pedometers and specific step targets results in increased physical activity levels and health improvements for sedentary individuals with or without chronic illness and/or mobility limitations (8, 9, 28). The step-count function of the Fitbit is designed to measure walking activity. Other physical activities that older adults may find meaningful, such as cycling, may not be accurately captured with this device. While newer activity monitors can now provide a number of metrics (e.g. energy expenditure, activity counts, distance), step counts are easy to understand, easy to set targets and easy to compare.
Study limitations
This study assessed a specific step-count device at specific walking speeds, but did not measure walking steps over the course of an entire day or during daily activities in a laboratory setting. The benefit of our protocol was that we could compare the number of steps recorded on the step-count device with a true gold standard (i.e. observed steps). The accuracy of the Fitbit at each speed (i.e. 0.3–0.9 m/s) was not assessed by individuals walking at their self-selected speed. However, we assessed the accuracy of the device across a range of speeds within each person, reflecting typical walking activity in which people vary their speeds throughout the day and across different activities. Our participants had a wide range of self-selected speeds, ranging from 0.5 to 1.7 m/s. Therefore, our protocol not only assessed participants who walked slowly at their self-selected pace, but also required participants to walk at a range of different speeds that they might experience in the community over the course of a day. Future studies should compare the accuracy of this device at the waist and ankle during the performance of daily tasks in older adults to further examine device utility in this population. A shorter testing distance was selected to ensure that participants could complete all 8 walking trials without fatigue, but still enabled a substantial number of steps per trial (~40 steps). It is possible that we may have overestimated the error due to miscounting when the total number of steps was small, and during the acceleration and deceleration phases of walking (29). It is unlikely that miscounting due to the acceleration and deceleration phases contributed to the percentage error recorded on the Fitbit – Waist at the slowest speeds, due to the large number of individuals not recording any steps at these speeds. Also, our results are not applicable to individuals with abnormal walking patterns, such as a shuffling gait. Our participants were healthy older adults who did not yet have any walking impairments, but had known medical conditions, with hypertension and diabetes being the most common. Our results may therefore generalize to individuals with chronic conditions with limited gait speed. Finally, our findings are limited to the specific device studied.
Conclusion
This study represents the first step in assessing the accuracy of the Fitbit One step-count device during slow continuous walking. The Fitbit One is accurate at speeds of 0.4–0.9 m/s when placed at the ankle (≥ 94% accuracy). The accuracy of the waist-worn Fitbit did not surpass 90% accuracy until faster speeds (0.8 m/s) were assessed. Sedentary individuals who have limited mobility and/or endurance may become frustrated and less motivated to continue with a lifestyle change intervention if the step-count device output does not represent their true level of activity. The Fitbit One, modified by wearing it at the ankle, is accurate for monitoring physical activity in older adults who walk slowly.
ACKNOWLEDGEMENTS
This work was supported by the Canadian Institutes of Health Research and Heart and Stroke Foundation of BC and Yukon. The authors would like to thank Jaymi Booth, Christie Chan, Zoe Hassall, Chihya Hung, Amanda Mow, and Caryne Torkia for providing assistance. The authors have no conflicts of interest to declare.
REFERENCES
