Jürgen Linder, MD, PhD1, Gunilla Brodda Jansen, MD, PhD2, Kristina Schüldt Ekholm, MD, PhD3 and Jan Ekholm, MD, PhD2
From the 1Division of Insurance Medicine, Department of Clinical Neuroscience, Stockholm, 2Department of Clinical Sciences, Division of Rehabilitation Medicine, Karolinska Institutet, Danderyd University Hospital, Stockholm and 3Mid Sweden University, Östersund, Sweden
OBJECTIVE: To describe the frequency of reported sleeping, depression and pain problems, the severity of these problems and the degree of self-estimated difficulties in mental functions and activities in relation to the sleep disturbance and pain category group in patients on long-term sick-leave.
DESIGN: Cross-sectional study.
Patients: A total of 1206 patients experiencing difficulty in resuming work.
METHODS: Patient examinations by specialists in psychiatry, orthopaedic surgery and rehabilitation medicine. Validated questionnaires, including status regarding depression, sleep, pain and functioning were used.
RESULTS: The prevalence of sleep disturbance was 83%; 74% of the patients with moderate/severe sleep disturbance also had moderate/severe pain problems and 26% had no/mild pain problems. Fifty-seven percent of the patients with no/mild sleep disturbance and 83% of the patients with moderate/ severe sleep disturbance also had depression. The degree of difficulty in performing the 6 selected International Classification of Functioning, Disability and Health activities and mental functions was higher for the category with moderate/severe sleep problems, compared with those with no/mild sleep problems.
CONCLUSION: To optimize rehabilitation for patients on long-term sick-leave experiencing difficulties in returning to work, the results indicate a need also to focus attention on sleep problems and not only on pain and depression. This may entail the planning of measures to improve decision-making and concentration and alleviate lassitude, fatigability, sadness and pessimistic thoughts.
Key words: sleep disorders; pain; depression; functioning; sick leave; rehabilitation; mental functions; activity limitations; disability; work resumption.
Correspondence address: Jürgen Linder, Department of Clinical Neuroscience, Karolinska Institutet, Filmgatan 22, SE-169 33 Solna, Sweden. E-mail: jurgen.linder@ki.se
J Rehabil Med 2014; 46: 00–00
Accepted March 4, 2014; Epub ahead of print May 21, 2014
Introduction
Many authors have studied sleep disturbances; both regarding quality and quantity, and have found that these are common problems for patients with longstanding pain, and that there is a relationship between sleep and pain (1–3). There is increasing interest in the relationship between sleep disturbance and work disability (4) and rehabilitation measures (5). A recent study has indicated that insomnia plays a major role in sickness absence (6).
The cause of sleep disturbances is a topic of debate, regarding what comes first, the pain or the sleep problems, as is the origin of the disturbed sleep. Depression alone can cause poor sleep, or it can be a symptom in depression and pain conditions (7, 8). Sleep disturbances can also be present without concomitant depression in patients who have pain. For instance, patients with rheumatoid arthritis or fibromyalgia often report poor sleep, both regarding number of hours and quality (3). Sleep deprivation affects pain thresholds not only for patients with ongoing pain, but also in healthy subjects in whom disrupted sleep can lead to spontaneous pain or increased sensitivity to evoked pain in experimental settings (9, 10).
Several research groups have studied the relationship between sleep disorders and problems in functional status (11–13). Åkerstedt et al. (14) have shown that disturbed sleep and fatigue in a national sample are predictors of lack of return from long-term (> 90 days) and intermediate-term sickness absence. It was shown that frequent sleep problems were associated with subsequent sickness absence spells in middle-aged public sector employees in Finland (15). In a recently published prospective study it was noted that the presence of sleep disturbances, together with a number of health complaints, predicted onset, persistence and worsening of pain. It was also suggested that the elimination of sleep problems in an early phase was an interesting approach towards treating chronic pain (16).
The present study focuses on sleep disturbances within a group of patients on long-term sick-leave, the rationale being that sleep disturbances may be a common denominator in these patients, who generally are diagnosed with depression, chronic pain or both. In the present study, all patients were on long-term sick-leave and had not been able to resume work and they had, in that sense, become long-term “problem cases” for the social insurance officers. To be able to optimize rehabilitation efforts and give patients an individually tailored rehabilitation period there is a need to assess difficulties other than pain and depression and to focus on and understand sleep disturbances, which are frequently reported by the patients.
The actual research aims are therefore directed towards the frequency of reported sleeping, depression and pain problems, the severity of these problems and the degree of self-estimated difficulties in selected International Classification of Functioning, Disability and Health (ICF) mental functions and activities in relation to the sleep disturbance and pain category group (ICF) (17).
The following questions were addressed regarding the present patients: (i) What is the distribution of the different degrees (mild or no, moderate or severe) of sleep disturbance in the patients? (ii) What is the relationship between the degree of sleep disturbance and degree of pain? (iii) What is the relationship between the degree of sleep disturbance and occurrence of major depression? (iv) What is the relationship between the degree of sleep disturbance and occurrence of depression in patients with or without long-standing pain? (v) What is the degree of self-estimated difficulties in selected ICF activities and mental functions in relation to the patients’ sleep disturbance and pain categories?
Material and methods
Participants
In a cross-sectional study, individuals on long-term sick-leave experiencing difficulties in returning to work were identified by local social insurance officers, and referred to a special unit designed for psychiatric and somatic diagnosis and assessment of the current disability status. In total, 1,335 individuals were consecutively referred for a medical assessment during a 10-year period between 1998 and 2007; see earlier studies (4, 5, 18–21). During this 9-year time-span no major changes had yet been made in the Swedish Social Insurance system, i.e. there was, for instance, no time limit in Sweden for individuals’ sickness benefits (22). The participants lived in Stockholm County, which has a population of approximately 2 million.
From the referred patients, 31 individuals did not participate. The remaining 1,304 patients were clinically examined; 1,005 by 3 board-certified specialists in psychiatry, orthopaedic surgery and rehabilitation medicine, and 299 patients exclusively by a board-certified psychiatrist due to obvious dominating psychiatric problems. A further 98 individuals were excluded due to incomplete questionnaires, and the final study group thus comprised 1,206 patients.
After completing several questionnaires the patients were examined by the 3 specialists who later met and jointly agreed on making 1 or more International Classification of Diseases, tenth edition (ICD-10) diagnoses (23) for each individual.
Questionnaires
Several questionnaires were used. For symptoms and diagnostic criteria, the following scientifically validated self-report scales were used: the Comprehensive Psychopathological Rating Scale for Self Administration (CPRS-SA) (24), measuring 23 symptoms and including the Montgomery-Åsberg Depression Rating Scale (MADRS) (25). In addition, the Depression Rating Self Report Questionnaire (DSRS) was used as a tool to identify possible depression (26). Complete details of this procedure have been published previously (7, 8, 18–21). For self-assessment of difficulties with activities and mental functions, questions from the CPRS-SA (24) were used; these questions allow scoring on a 0–3 scale (similarly to the description of the item “aches and pain” below).
When linking the items of the health-status measures used, to the World Health Organization (WHO) ICF categories, the published linking rules were applied (17, 27–29). There were no problems linking 5 of the selected items. The concept “lassitude” may be seen as a mental function, but we have intentionally chosen to emphasize its activity aspect and therefore made the link to d220 “Undertaking multiple tasks” (instead of b1301 “Motivation” that had been the choice as a mental function, and in our opinion had not completely covered the concept behind the question).
Definition of sleep disturbances
Sleep disturbances were categorized by means of the item “Reduced Sleep” in the MADRS (25). The item text in the MADRS is as follows:
“Reduced Sleep
Representing the experience of reduced duration or depth of sleep compared to the subject’s own normal pattern when well.
0 Sleeps as usual
1
2 Slight difficulty dropping off to sleep or slightly reduced light or fitful sleep
3
4 Sleep reduced or broken by at least two hours
5
6 Less than two or three hours sleep
Note: Patients could mark their score anywhere and continuously on a vertical line to the left of the digits and item text.”
Definition of pain scores
The item text for “Pain” in the CPRS (24) is as follows:
“Aches and pains
Representing reports of bodily discomfort, aches, and pains.
0 Absent or transient aches
1 Occasional definite aches and pains
2 Prolonged and inconvenient aches and pains. Request for effective analgesics
3 Severely interfering or crippling pains
Note: Patients could mark their score anywhere and continuously on a vertical line to the left of the digits and item text.”
All item scores were measured with a ruler and immediately transferred to a special database. After validation the data were stored in a SPSS database (IBM SPSS 22.0 for windows (SPSS Inc., Armonk NY, USA)).
The scores from the sleep and pain items were dichotomized based on the median scores and categorized into 2 levels: 1 = no or mild symptoms; 2 = moderate to severe symptoms. The 0–6 scale used by the patients for the sleep item was transformed back to the original 0–3 scale (24, 25).
Definitions of sleep categories
S1 Sleep category 1 (no or mild sleep disturbance): below median score
S2 Sleep category 2 (moderate to severe sleep disturbance): above median score
Definitions of pain categories
P1 Pain category 1 (no or mild aches and pains): below median score
P2 Pain category 2 (moderate to severe aches and pains): above median score
Statistical methods
All calculations were performed using non-parametric statistics (the χ2 test, Fisher’s exact test, the Kruskal Wallis test and Wilcoxon’s rank-sum test). Data were analysed using SPSS/PASW statistical program package. p < 0.01 was chosen as the level for statistical difference.
Ethical approval
The study was approved by the Regional Ethical Review Board in Stockholm, Sweden (1995-149; 2006/1281-31; 2008/71-31/5; 2008/1051-31/12, and 2010/448-32).
Results
Patients
The median [quartiles] age of the 1,206 patients was 45.9 [39.4–52.5] years, 62.8% were women, 41% were born outside Sweden, 62% had secondary school or higher education, and 53% were unemployed. All had been on long-term sick-leave for more than 1 year. The majority, 984 individuals, were on full-time and 178 were on part-time sick-leave. Their predominant medical problems were psychiatric, mainly depressive disorders, longstanding regional or general pain or combinations of psychiatric disorders and pain.
Diagnoses
The most common psychiatric diagnoses were mood disorders (ICD chapter F3), the most common somatic diagnoses were soft tissue disorders ICD-chapter M7), and the most common combination of psychiatric and somatic diagnoses was mood disorders and soft tissue disorders (F3 and M7).
In summary, 481 individuals had exclusively one or more psychiatric diagnoses, most commonly depression, anxiety and personality disorders (ICD-chapters F3, F4, F6). Exclusively somatic diagnoses were made in 268 patients, mainly soft tissues disorders or dorsopathia (M7, M5), and 449 individuals had combined psychiatric and somatic diagnoses. Eight individuals had symptoms but no ICD diagnoses were made.
Sleep and pain categories
The majority of the patients, 83% (1,002/1,206), reported sleep problems with a severity of > 0.5 on the 0–3 scale. Based on the median score (= 2.0) of the item “Reduced sleep”, 585 patients were grouped into sleep category 1 (S1). The remaining 621 patients were grouped into sleep category 2 (S2).
In category S1 (Table I, upper row), 57% (n = 334/585) of the patients were diagnosed with depression. In category S2, 83% (n = 515/621) were diagnosed with depression. As for sleep disturbances, the majority, 92% (1,104/1,206), reported pain with an intensity of more than 0.5 on the 0–3 scale. Based on the median score (2.0) of the item “Aches and pains”, 462 patients were grouped into pain category 1 (P1), and the remaining patients, n = 744 into pain category 2 (P2). In category P1, 64% (n = 295/462) (Table I, lower row) of the patients were diagnosed with depression. In category P2, 74% (n = 554/744) of the patients were diagnosed with depression.
Table I shows the distribution of sleep and pain categories with regard to presence or absence of depression for all 1,206 patients. Moderate to severe sleep disturbances (row S2) were more common in patients with concomitant depression, in 61% (515/849, column “Sum D1”, Table I). In comparison, only approximately 30% (106/357, column “Sum D0”, Table I) of the patients without concomitant depression experienced moderate to severe sleep disturbances (p < 0.001). In the group of moderate to severe sleep disturbance with concomitant depression, approximately 75% reported moderate to severe pain (387/515 column “P2D1”/”Sum D1”, Table I). Also, patients with moderate to severe sleep disturbance, but without concomitant depression, reported a similar frequency of moderate to severe pain, 71% (75/106, column “P2D0”/”Sum D0”, Table I)
|
Table I. Overview of the distribution of sleep and pain categories and relationship to presence or absence of depression |
|||||||||
|
Category |
P1D0 n |
P1D1 n |
Sum P1 n |
P2D0 n |
P2D1 n |
Sum P2 n |
Sum D0 n |
Sum D1 n |
Sum n |
|
S1 |
136 |
167 |
303 |
115 |
167 |
282 |
251 |
334 |
585 (S1) |
|
S2 |
31 |
128 |
159 |
75 |
387 |
462 |
106 |
515 |
621 (S2) |
|
Sum S1–S2 |
167 |
295 |
462 |
190 |
554 |
744 |
357 |
849 |
1,206 |
|
P1: Pain category 1; P2: Pain category 2; S1: Sleep category 1; S2: Sleep category 2; D0: without depression; D1: with depression. |
|||||||||
Sleep and depression
Fig. 1a (upper part), illustrates the percentage distribution of sleep problems (S1 and S2) in 4 groups in relation to the severity of pain (P1, P2) and in the absence or presence of concomitant depression (D0, D1). These 4 groups are shown in Fig. 1 as P1D0, P1D1, P2D0, and P2D1. In group P1D0 (patients in pain category 1 and with no depression), 18.6% had moderate to severe sleep problems. In group P1D1 (patients in pain category 1 with concomitant depression), 43.4% had to severe sleep disturbances (p < 0.0001, Fisher’s exact test, 2-tailed).
In group P2D0, (pain category 2 and no depression), 39.5% hade moderate to severe sleep problems, in contrast to group P2D1 (pain category 2 and depression), where 69.9% had moderate to severe sleep problems (p < 0.0001, Fisher’s exact test, 2-tailed).
Pain and depression
The lower part of Fig. 1b illustrates the percentage distribution of pain problems (P1 and P2) in relation to the severity of sleep disturbances (S1, S2) and to the absence/presence of concomitant depression (D0, D1), resulting in groups: S1D0, S1D1, S2D0, and S2D1. In group S1D0 (patients in sleep category 1 and no depression) the proportion of moderate to severe pain problems (P2) was 45.9%. In group S1D1 the proportion of P2 was 50%, i.e. no significant difference was noted. In group S2D0, (sleep category 2 and no depression, Fig. 1b, third column), the proportion of patients with moderate to severe pain problems (P2) was 70.8%, and in group S2D1, the corresponding percentage was 75.2%, and this difference was also not statistically significant.
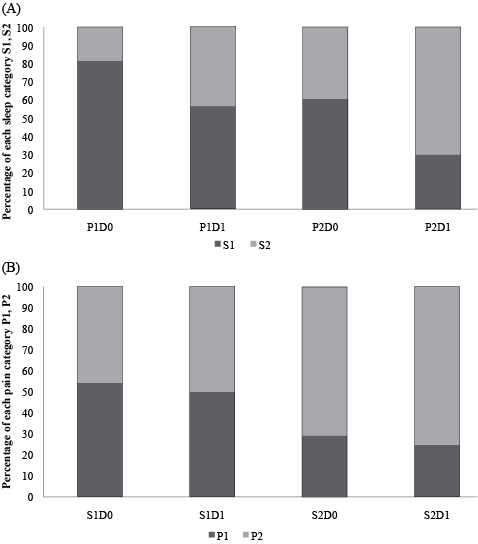
Fig. 1. (A) The percentual distribution of sleep disturbances, vertical axis (categories S1, S2) in 4 patient groups P1D0, P1D1, P2D0, and P2D1 grouped according to 4 possible combinations of pain (P1, P2 and depression (D0, D1) categories. The proportions in sleep categories S1 and S2 are significantly different when comparing patients with depression (D1) and patients without depression (D0) within each pain category, P1, P2 (p < 0.0001). (B) The percentual distribution of pain intensity, vertical axis (categories P1, P2) in 4 patient groups S1D0, S1D1, S2D0, and S2D1 grouped according to 4 possible combinations of sleep disturbance (S1, S2 and depression (D0, D1) categories. The proportions in pain categories P1 and P2 are not significantly different when comparing patients with depression (D1) and patients without depression (D0) within each sleep category, S1, S2.
Pain, sleep and depression
Fig. 2 shows another aspect of the relationship between the intensity of pain and of sleep disturbances in relation to depression. Within the light sleep disturbances category (category S1), more than half (55.1%) of the patients with no or mild pain, (group S1P1) also had depression. For patients with light sleep disturbances and moderate to severe pain (group S1P2), the frequency of depression was slightly greater (59.2%). There was no statistically significant difference between the proportions of depression with respect to pain intensity in the 2 groups with light sleep problems (S1P1 vs S1P2).
For the patients with moderate to severe sleep disturbances, (category S2), 80.5% of the patients with no or mild pain (group S2P1) and 83.8% of those with moderate to severe pain (group S2P2) were diagnosed with depression (Fig. 2). There was no statistically significant difference between the groups with severe sleep problems with regard to pain intensity. The overall differences between the 4 categories were highly significant (p < 0.0001, χ2 test). However, the minor differences in percentage of patients with depression within each sleep category were not significantly different. There was no statistically significant difference between the frequencies of pain within either group S1 or S2. In contrast, the differences between categories S1 and S2 were highly significant (p < 0.001, Fisher’s exact test), indicating that the severity of sleep disturbances, but not the severity of pain, influences the proportion of patients with co-morbid depression.
This can be seen as an increasing “degree of influence” of the combined sleep and pain problems, ranging from “mild or no” (S1P1) to “moderate to severe” (S2P2). Fig. 2 indicates that increasing sleep disturbances, together with increased pain intensity, seem to influence towards a higher prevalence of depression, from 55.1% of those with S1P1 to 59.2% of those with S1P2, to 80.5% of those with S2P1 and, finally, 83.8% of those in category S2P2.
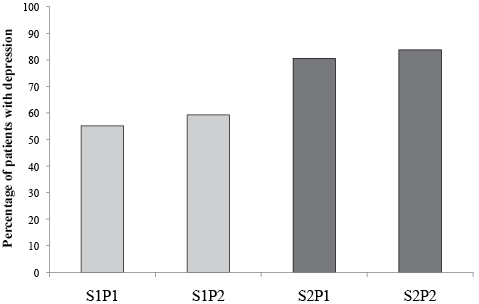
Fig. 2. Percentage of patients with presence of depression in relation to 4 combinations of sleep disturbance and pain intensity categories. Horizontal axis shows combined categories in increasing order from S1P1 to S2P2. Vertical axis shows percentage of patients with depression.
For the 849 patients with depression (group D1) (Table II, lower half second-last column), 334 had mild or no sleep disturbances (group S1D1) (Table II). Of these patients, 50% (n = 167) had no or mild pain (P1) and the remaining 167 individuals had moderate to severe pain (P2). The 515 patients with moderate to severe sleep disturbances and depression (S2D1), 25% (n = 128) had no or mild pain (P1D1) and 75% (n = 387) had moderate to severe pain (P2D1).
In the patient group without depression, n = 357 (Table II, upper half, second-last column), most patients, 70% (251/357), had no or light sleep disturbances. Within this group (S1D0), 54%, (n = 136) had no or mild pain (P1D0) and 46% (n = 115) had moderate to severe pain (P2D0). Of the patients without depression (Table II, upper half, second-last column), 106/357 had moderate to severe sleep disturbances. In this subgroup, 29% (n = 31), had no or mild pain and 71% (n = 75) experienced moderate to severe pain.
|
Table II. Proportion of pain problems, pain categories P1, and P2 in the sleep categories with no or mild (S1) and with moderate to severe sleep problems (S2) in patients without depression, D0, and with depression, D1 |
||||
|
Category |
P1D0 % (n) |
P2D0 % (n) |
Sum % (n) |
Group |
|
Without depression |
||||
|
S1 |
54 (136) |
46 (115) |
100 (251) |
S1D0 |
|
S2 |
29 (31) |
71 (75) |
100 (106) |
S1D0 |
|
Sum |
47 (167) |
53 (190) |
100 (357) |
D0 |
|
P1D1 |
P2D1 |
|||
|
With depression |
||||
|
S1 |
50 (167) |
50 (167) |
100 (334) |
S1D1 |
|
S2 |
25 (128) |
75 (387) |
100 (515) |
S2D1 |
|
Sum |
35 (295) |
65 (554) |
100 (849) |
D1 |
|
p < 0.001 Fisher’s exact test, right tailed (probability of belonging in category S2 is greater for P2 than P1 within each category of depression (D0: no depression; D1: depression). |
||||
The relationship between sleep categories and depression is shown in Table III (upper part). Of the 849 patients with depression (D1), the majority, 61% (n = 515) had moderate to severe sleep disturbances. Among the 357 patients without depression (D0), only 30% (n = 106) had moderate to severe sleep disturbances (S2). In comparison, the relationship between pain categories (Table III, lower part) was that in which the 849 patients with depression, 65% (n = 554) belonged to pain category P2 and had moderate to severe pain. For the patients with no depression (n = 357), 53% (n = 190) had moderate to severe pain and belonged to pain category P2.
|
Table III. Relationship between depression (D1, D0) and sleep disturbances (S1, S2), regardless of the presence of pain (upper section). Relations between depression (D1, D0) and pain intensity (P1, P2), regardless of the presence of sleep disturbances (lower section) |
|||
|
Sleep category |
S1 % (n) |
S2 % (n) |
Significance pa |
|
Depression (D1) |
39 (334) |
61 (515) |
|
|
No depression (D0) |
70 (251) |
30 (106) |
< 0.001 |
|
Pain category |
P1 |
P2 |
|
|
Depression (D1) |
35 (295) |
65 (554) |
|
|
No depression (D0) |
47 (167) |
53 (190) |
< 0.001 |
|
aFisher’s exact test, 2-tailed. |
|||
In summary, we conclude that sleep disturbances, and particularly sleep disturbances in combination with pain, are related to the prevalence of depression in the present patient material. For pain alone, controlling for sleep disturbances, no significant relationship between pain intensity and the prevalence of depression was noted.
Activities and mental functions
Activity limitations among the patients with sleep disturbance and difficulties in resuming work are shown in Table IV; the median scores for ability to make decisions in pain category 2 (P2) increased from 0.05 to 1.1 (on a scale from 0 to 3) with increasing degree of sleep disturbance (S1–S2). Likewise, the median score for P2, of degree of difficulty in ability to concentrate increased from 1.0 to 2.0 (S1–S2). Degree of difficulty in lassitude and related difficulty in undertaking tasks for category P2 increased from 1.3 for S1 to 2.0 for S2.
Impaired mental functions are also described in Table IV, lower part. The median scores for “Difficulty in terms of fatigability” increased from 1.5 in group S1P1 to 2.0 in group S2P2 on the 0–3 scale. In comparison, the scores for “Degree of sadness” and “Pessimistic thoughts” increased from 0.8 to 1.0 in group S1P1 to 2.0 in group S2P2.
|
Table IV. Disability, pain categories and degree of sleep disturbance (International Classification of Functioning, Disability and Health (ICF) b134). Medians and quartiles for: Pain categories: P1: no/mild pain; P2: moderate/severe pain. Sleep categories: S1: no/mild sleep disturbances; S2: moderate/severe sleep disturbances: Kruskal-Wallis test |
||||
|
Pain category |
S1 no/mild sleep disturbance Median (quartiles) |
S2 moderate/severe sleep disturbance Median (quartiles) |
Significance p (row) |
|
|
Activity/ICF category/question |
||||
|
Making decisions/ICF-d177/Ability to make decisions |
P1 |
0.5 (0–1) |
1.0 (0–2) |
0.005 |
|
P2 |
0.05 (0–1) |
1.1 (0–2) |
< 0.0001 |
|
|
Significance p (column) |
0.031 |
0.105 |
||
|
Focusing attention/ICF-d160/Ability to concentrate |
P1 |
1.0 (0.5–2) |
2.0 (1.0– 2.1) |
0.001 |
|
P2 |
1.0 (0.5–2.0) |
2.0 (1–2.5) |
< 0.0001 |
|
|
Significance p (column) |
0.038 |
0.272 |
||
|
Undertaking multiple tasks/ICF-d220/Lassitude |
P1 |
1.0 (0.5–2.0) |
2 (1.0–2.4) |
< 0.0001 |
|
P2 |
1.3 (0.5–2.0) |
2.0 (1.5– 2.5) |
< 0.0001 |
|
|
Significance p (column) |
0.007 |
0.30 |
||
|
Functions/ICF category/question |
|
|
|
|
|
Energy level/ICF-b1300/Fatigability |
P1 |
1.5 (1.0–2.0) |
2.0 (1.5–2.4) |
0.038 |
|
P2 |
2 (1.01–2.1) |
2 (2.0–2.5) |
< 0.0001 |
|
|
Significance p (column) |
< 0.0001 |
< 0.0001 |
||
|
Emotional functions/ICF-b152/Sadness |
P1 |
0.8 (0.0–1.5) |
1.0 (0.0–1.5) |
< 0.0001 |
|
P2 |
1.0 (0.0–1.5) |
2.0 (1.0–2.5) |
< 0.0001 |
|
|
Significance p (column) |
0.44 |
0.027 |
||
|
Optimism/pessimism/ICF-b1265/Pessimistic thoughts |
P1 |
1.0 (0.5–1.5) |
2.0 (1.0–2.1) |
< 0.0001 |
|
P2 |
1.0 (0.1–1.5) |
2.0 (0.95–2.13) |
< 0.0001 |
|
|
Significance p (column) |
0.664 |
0.317 |
||
Discussion
The present study addresses individuals on long-term sick-leave experiencing difficulties in returning to work, and one of the key questions is what factors contribute to their working incapacity. The inter-relationship between some of these factors has previously been studied, e.g. the intensity, duration and spreading of pain (7), as have somatic pain conditions and comorbid psychiatric disorders (8).
A number of studies have addressed the issue of sleep problems in relation to pain, depression and sickness absence (30–32). In a study from Hong Kong, it was reported that co-occurrence of chronic pain and sleep disturbances was common in the general adult population (33). In patients with fibromyalgia syndrome, it is suggested that sleep problems play a role in the relationship between pain, anxiety and depression (3, 30). Sleep problems have been reported to treble the risk for the development of depression in patients with persistent pain, and for those patients considerations concerning the prevention or treatment of sleep problems in addition to focusing on pain management have been suggested (32). Furthermore, recent studies from Finland have pointed out that sleep problems should be addressed to prevent ill health and sickness absence (31, 34).
The present study focused on sleep, pain, depression, and selected functioning issues in individuals on long-term sick-leave experiencing difficulties in returning to work. One of the main questions addressed in the present study is how frequent mild or severe sleep disturbances are in these patients.
Half of the patients were categorized as having moderate to severe sleep disturbance. The definition used for moderate to severe sleep disturbance implies that the patients had only a couple of hours of unbroken sleep, or worse still, less than a couple of hours of unbroken sleep in total (25). It can be concluded that many of these individuals on long-term sick-leave experiencing difficulties in resuming work had a more severe form of sleep problem. These findings are in line with those of others (15, 35). A recent study from Norway (36) pointed out that factors other than physical functioning could influence return to work among employees with chronic musculoskeletal pain and comorbid depressive symptoms. This is also in line with the findings of Theorell’s group, that employees without a history of sickness, in comparison with employees with a history of sickness, experienced less sleep disturbances and less neck, shoulder and back pain (37).
In the present study more than 80% of the patients reported sleep disturbances scoring higher than 0.5 on a scale from 0–3 and more than 90% reported pain scoring higher than 0.5 on a scale from 0–3. This is in line with a review of recent longitudinal and experimental data on the association of sleep and pain. It states that a key trend emerging from population-based longitudinal studies is that sleep impairments reliably predict new incidents and exacerbations of chronic pain (38). Longitudinal studies employing subjective and objective assessments of pain and sleep support the notion that sleep impairments are a stronger, more reliable predictor of pain than pain is of sleep. The review also reports that recent experimental studies suggest that sleep disturbance may exacerbate key processes that contribute to the development and maintenance of chronic pain.
Approximately 70% of the patients were also diagnosed with comorbid depression. In these 849 depressed patients, twice as many (60.7%) reported moderate to severe sleep problems as in the 357 patients without comorbid depression (29.7%). The proportions of moderate to severe pain problems were 65.3% in the depressed patients and 53.2% in the patients without concomitant depression. Since both differences were statistically significant (p < 0.0001, Fisher’s exact test), we conclude that sleep disturbances as well as pain contribute to the prevalence of comorbid depressions in this particular group of patients.
With our background of interest in working capacity and vocational rehabilitation perspectives, another basic question is to what extent sleep disturbance impacts on activities and functions. Ability to perform activities can be influenced by sleep disturbance and by depression or pain (14). The results of the present study concern patients with or without depression and, in addition, the extent of degree of pain reported. Our results show that patients of category (S2) with moderate to severe sleep problems had more difficulty in performing the 3 activities assessed than patients with no or mild sleep disturbance; the S2 patients had more difficulty in their ability to make decisions, to concentrate and they had problems with lassitude and related ability to undertake tasks. The median for ability to concentrate was 2, on a scale where 3 means that the activity cannot be performed at all. It is concluded that individuals on long-term sick-leave experiencing difficulties in returning to work and with sleep problems have difficulties in performing common important daily activities: ability to make decisions, ability to concentrate, and ability to undertake tasks due to lassitude.
The results show that the degree of fatigability, sadness and pessimistic thoughts increased with the degree of severity of sleep problems. In addition, fatigability also increased with severity of pain problems. The findings on mental functions and activities are in agreement with the ICF core sets on sleep disturbance (11–13), since these items are present in the comprehensive ICF core set for sleep disturbance. It has also been shown that even a single night of sleep deprivation can have a strong effect on decision-making (39). Compared with controls, patients with idiopathic rapid eye movement sleep behaviour disorder showed disadvantageous decision-making under ambiguity (40). Since decision-making, ability to concentrate, lassitude, fatigability, sadness, and pessimistic thoughts are considered to be important factors for working capacity, it is proposed that difficulties with these functioning issues may be part of the reason why these patients have problems resuming work.
Limitations of the study
The present data on pain, sleep, and depressive symptoms were based on the patients’ self-reports, which could bias the results. However, all questionnaires were completed in the setting of the hospital department, with personnel present who could answer questions from the patients about the forms. No forms were sent to the patients’ homes, in order to minimize the risk of relatives or other external factors influencing the patients’ answers.
Furthermore, on the one hand, it must be clear that these results cannot be generalized since they are derived from a patient group consisting of long-term sick-listed patients experiencing difficulties in resuming work. However, on the other hand, such patients are commonly found in rehabilitation settings and are often identified as problematic.
Conclusions and major results of this study
1. The prevalence of sleep disturbance in this particular population of patients with extremely long-term sickness absence experiencing difficulties in resuming work is very high (83%).
2. The distribution of sleep and pain disturbances was that 74% of the patients with moderate/severe sleep disturbance also had moderate/severe pain problems, and 26% had no/mild pain problems. Of the patients with no/mild sleep disturbance, 48% had moderate/severe pain problems, and 52% no/mild pain problems.
3. Concerning the relationship between sleep disturbance and occurrence of major depression it was noted that 57% of the patients with no/mild sleep disturbance and 83% of the patients with moderate/severe sleep disturbance also had depression. A further implication was that 43% of the patients with no/mild sleep disturbance and a minority, 17% of the patients with moderate/severe sleep disturbance did not have concomitant depression.
4. The relationship between occurrence of pain and major depression was that 64% of the patients with no/mild pain and 75% of the patients with moderate/severe pain had depression. This implies that 36% of the patients with no/mild pain and 25% of the patients with moderate/severe pain were not diagnosed with depression. Comparing the possible influence of sleep disturbance vs pain, it seems that sleep disturbance has a higher correlation with depression than that of pain intensity and depression.
5. The degree of difficulty in performing the 6 selected ICF activities and mental functions was higher for the category with moderate/severe sleep problems, compared with the patient category with mild/no sleep problems.
Concluding comment
To optimize rehabilitation programmes for patients on long-term sick-leave experiencing difficulties in returning to work, the results indicate a need to focus attention on sleep problems and not only on pain and depression. This may entail the planning of measures to improve decision-making and concentration and alleviate lassitude, fatigability, sadness and pessimistic thoughts.
References
