OBJECTIVE: The aim of this study was to explore and analyse the experience of living with long-term neck/shoulder pain and its effect on daily life.
DESIGN: A thematic interview study with emergent design.
SUBJECTS: Twelve patients in primary care (6 women and 6 men) with long-term neck/shoulder pain.
METHODS: Thematic interviews analysed using grounded theory.
RESULTS: A conceptual model emerged. The core category “striving to master variable pain” comprises how the informants are constantly aiming at not letting it become too much of a hindrance. The 3 sub-categories “space for health”, “strategies for pain control” and “disruptions in daily life” interact with each other. Giving oneself adequate time and prioritizing one’s health-promoting behaviour in relation to pain were important when adopting strategies for pain control. Men and women differed when describing consequences for domestic life and prioritizing their own health in relation to pain.
CONCLUSION: Living with long-term variable neck/shoulder pain involves a struggle not to let the pain become too much of a physical obstacle to daily life. Individuals learn to respond to the pain in different ways. Allowing oneself adequate time and prioritizing health in relation to pain appear to be important for controlling pain.
Key words: coping skills, daily life, neck/shoulder pain, primary health care, qualitative research.
J Rehabil Med 2009; 41: 768–774
Correspondence address: Cia Hunhammar, KvartersAkuten Matteus, Surbrunnsgatan 66, SE-113 27 Stockholm, Sweden. E-mail: ciahunhammar@hotmail.com
Submitted June 29, 2008; accepted May 27, 2009
INTRODUCTION
Neck pain is a common health problem worldwide, with lifetime prevalence between 14% and 71% and point prevalence between 6% and 22% (1). Neck pain often occurs together with pain from the upper extremities (2). Neck/shoulder pain (NSP) may arise from various structures in the neck or shoulder, and is, in many cases, labelled non-specific since no specific cause can be identified (3). A Dutch study presenting the self-reported prevalence of musculoskeletal pain in the general population showed that NSP occurs in all adult age groups, is most common between 45 and 64 years of age, and that females have a higher prevalence than men in all age groups (4).
Knowledge of the natural history of NSP is limited. The majority of patients recover within approximately one month and, for the others, the bulk of reduction is completed after 3 months (5). However, neck pain seems to recur and there is a risk of long-standing problems. A study conducted in Sweden showed that approximately 50% of people presenting to a general practitioner for neck pain reported pain and pain-related disability at a 5-year follow-up (6).
Many factors are assumed to contribute to the onset of NSP. Work-related physical factors, such as high physical load and repetitive work, are suggested to contribute (7). Bongers et al. (8) have reported that work-related psychological factors, i.e. high quantitative job demands, perceived job stress and general distress and co-morbidity, were of importance. Critical life changes influence the onset (9). Evidence about predictive factors for developing long-term NSP is limited. A history of previous attacks, long duration of pain, concomitant low-back pain, and age over 40 years seem to be associated with persistent NSP (10).
NSP is often described as recurrent, mild-to-moderate and, for most individuals, a low-intensity non-disabling condition (4). However, approximately 10–30% of those who reported NSP the preceding year experienced consequences for daily life (4). A Canadian survey on the prevalence of neck pain and neck-pain-related disability showed that 5% experienced disabling neck pain (11). In Sweden, approximately one-third of those who reported NSP the preceding year also reported healthcare consumption (6). NSP reportedly leads to socioeconomic costs for the individual and the community, and people on sick-leave account for the majority of these costs (12).
Living with long-term musculoskeletal pain and its consequences for daily life has been studied extensively among persons with fibromyalgia and generalized pain syndromes. Living with fibromyalgia is described as being greatly influenced by the pain, attempting to achieve pain relief and struggling for a tolerable existence (13, 14). Living with long-term neck-and lumbar pain has considerable consequences for daily life and is often a long process of accepting and adjusting to the pain (15, 16). However, research on experience of living with long-term regional pain is more limited, apart from studies focusing on migraine, long-term daily headache and long-term knee pain. Living with migraine and long-term headache affect all aspects of everyday life (17) and long-term knee pain is described as an impairment of quality of life (18). Clinical experience has shown that persons with long-term NSP experience consequences for daily life and many seek primary care. Better understanding of the experience of living with long-term NSP and its influence on daily life might reveal new insights that could affect the content of primary-care rehabilitation.
Aim
The aim of this study was to explore and analyse the experience of living with long-term non-specific NSP and how it influences daily life.
METHODS
Theoretical perspective
To be able to explore and analyse living with long-term NSP, a qualitative approach was chosen. Qualitative research methods are used for exploring the meanings of social phenomena as experienced by individuals themselves in their natural context (19). Grounded theory was chosen since it seeks to describe the field studied and is regarded as suitable for discovering new knowledge and generating new models/theories. The design was emergent and the sampling technique purposive, giving a more focused design over time as a result of the increased understanding a researcher achieves throughout the research cycle (20). Constant comparison was chosen as the data analysis method (21).
Study sample
In the present study NSP was defined as a person’s experience of pain located in the neck/shoulder region, and pain-related disability. Long-term pain was defined as pain lasting more than 6 months. Pain-related disability was defined as a condition of disability induced by long-term pain, as discussed by von Korff et al. (22). Neither the pain intensity nor the severity of the pain-related disability was taken into account for the present inclusion criteria. Inclusion criteria were: seeking primary care for long-term NSP; understanding and speaking Swedish; and age between 18 and 65 years. Exclusion criteria were: whiplash injury; neuropathic pain; cervical tumour or fracture; and rheumatoid arthritis or other disease, e.g. diabetes or neurological diseases, which might lead to disability. Information about the study and the participation criteria was given to physiotherapists working at 5 different clinics in urban primary care. Doctors at one primary care clinic were also informed. Thirteen patients were nominated and asked by their physiotherapist or doctor to participate. Twelve (6 women and 6 men) gave their informed consent. Initially the aim was to capture a broad diversity of perspectives from the informants. Sampling was conducted in relation to age, occupation and civil status. After the analysis of the first 4 interviews, it was found that some experiences were described differently by men and women. The subsequent purposive sampling then became more focused on finding as many women as men, as well as finding both men and women with no children living at home/having children living at home and with children of different ages. After 9 interviews a core category and 2 sub-categories had reached saturation, i.e. an additional interview would not add any substantial new information central to those categories (20). In order to reach saturation in all categories, the subsequent purposive sampling focused on finding informants with small children. Finally, the categories were considered saturated after 12 interviews. The informants were both blue-collar and white-collar workers; all were urban dwellers. At the time of the study informants were enrolled at the physiotherapy departments, but there was no relationship of dependence between informants and interviewer. After the interview the informants completed a form for background data and a self-rating scale with 3 questions about pain severity and 3 about pain-related disability, as described by von Korff et al. (22). The informants rated their present pain, the worst pain the preceding 6 months and the average pain over the preceding 6 months. The 3 disability questions dealt with the ability to continue with their usual activities of daily life, social life and working life during the preceding 6 months. Table I shows background data on the informants and data from the self-rating scales (22). The study was carried out in accordance with the Helsinki Declaration Criteria. Informed consent, confidentiality and the possibility to withdraw from the study at any time were stressed.
|
Table I. Background data of the informants and the self-ratings of pain intensity and pain-related disability described by von Korff et al. (22) (n = 12)
|
|
Sex, women/men, n
|
6/6
|
|
Age, years, median (range)
|
36.5 (19–58)
|
|
Durations of symptoms, years, median (range)
|
2.5 (0.5–30)
|
|
Marital status, married/partner, n
|
9
|
|
Education level, n
|
|
Upper secondary school
|
6
|
|
University
|
6
|
|
Occupational status, n
|
|
Full-time work 100%
|
6
|
|
Part-time 75%*
|
1
|
|
Part-time sick leave/pension 50%
|
3
|
|
Parental leave
|
1
|
|
Student
|
1
|
|
Informants with children at home, n
|
7
|
|
Age of children at home, years, median (range)
|
13 (1.3–19)
|
|
Self-rated pain intensity scale† median (range)
|
57 (33–83)
|
|
Self-rated pain-related disability scale‡ median (range)
|
33 (13–76)
|
|
*Self-chosen; †scale 0–10 (0 = “no pain” and 10 = “pain as bad as it could be”); ‡scale 0–10 (0 = “not affected at all” and 10 = “impossible to continue these activities”). For each informant a separate score for pain intensity and pain-related disability was created by calculating the mean of the 3 questions times 10. The median was then calculated for the whole group.
|
Data collection
The informants were interviewed by the first author (CH). Eleven interviews were held at the physiotherapy department and one in the informant’s home. Thematic interviews were used; that is, open-ended questions with themes decided beforehand (23), covering the private, occupational, domestic and social areas of daily life. The themes were chosen with the hypothesis that the pain might affect these areas. The open-ended questions were formulated to encourage the informants to speak freely and in their own words about their experience. During the analysis the authors discussed the mode of interviewing in order to ascertain open-ended questions. The interview started with the question “Could you describe a situation in daily life in which the pain has had an effect?” In accordance with emergent design, the interviews eventually broadened to deal with strategies used to control pain and circumstances perceived as important for controlling the pain. The interviews lasted between 40 and 55 min, except for one that lasted 15 min. They were tape-recorded and transcribed verbatim by the first author.
Data analysis
The interviews were analysed according to the grounded theory of constant comparison (21). The data was analysed concurrently with data collection in order to develop a more focused research design. In the first stage the data was analysed with open coding, i.e. word-by-word. The method is descriptive, aiming to capture the content of the data. For this, the Open code software program (24) was used. Two of the authors (CH, ML) analysed the interviews independently, and compared and discussed the codes until consensus was reached.
The next step was selective coding, deciding which open codes were important for the research topic. The selective codes were clustered and transformed into abstract categories with their properties and dimensions. The selective coding included choosing a core category and examining the data again with improved knowledge of what to look for. During the analysis a model emerged, and this was revised step by step. Triangulation by several researchers was used to ensure trustworthiness (19, 20). Two of the authors coded the interviews independently (CH, ML) and all 3 (CH, ML, LNW) questioned and discussed the emerging categories and the final model before it was accepted. The authors’ differing perspectives proved fruitful in the analyses. One author is a physiotherapist in primary care with preference for pain treatment, one has experience in multi-professional pain rehabilitation, and one has a teaching background. Other perspectives were obtained through discussions with consulting colleagues.
RESULTS
During the analyses a conceptual model emerged. The model explicates the informants’ experience of living with long-term variable NSP and consists of one core category “striving to master variable pain” and 3 sub-categories; “space for health”, “strategies for pain control” and “disruptions in daily life”. The model comprises how the informants were constantly “striving to master variable pain” aiming at not letting it become too much of a hindrance to daily life. The 3 sub-categories interact with each other, without causal relationship (Fig. 1). The categories’ properties are situated somewhere on a continuum, i.e. they had dimensions. A dominant feature was great variation in pain intensity during different periods. Furthermore, the informants described different attitudes to the fact that the pain existed, might persist and to the recurrent nature of the pain. Sub-category 1: “space for health” was described as important for controlling the variable pain and its consequences for daily life. “Space for health” comprises working and living conditions, giving priority to health-promoting behaviour in relation to the pain and the perceived cause of the pain. Sub-category 2 comprises the adoption of different “strategies for pain control” and sub-category 3 comprises physical, psychological and social consequences of pain, “disruptions in daily life”. Table II gives detailed descriptions of the categories, properties and dimensions. Some categories were described differently by women and men. In accordance with emergent design, the material was therefore also analysed separately by gender. Quotes from the interviews are used to describe some of the properties. Numbers in square brackets after the quotes identify the number of the interview. The quotations are marked by gender (f = female m = male).
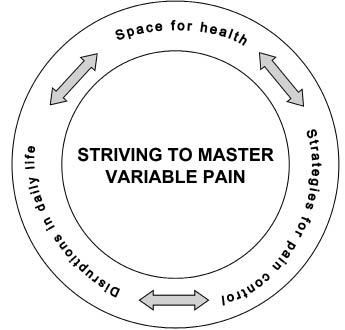
Fig. 1. The model illustrates the core category “striving to master variable pain” and the 3 sub-categories “space for health”, “strategies for pain control”, and “disruptions in daily life”.
|
Table II. The core-category and the 3 subcategories with properties and dimensions
|
|
|
Property
|
Dimension
|
|
Core category
|
|
|
|
Striving to master variable pain
|
Variable pain
|
mild ↔ intense
|
|
Thoughts about the future
|
hope for improvement ↔ worry for deterioration
|
|
Attitudes to pain
|
adjust ↔ ignore
|
|
Sub-category
|
|
|
|
Space for health
|
Working and living conditions
Priority for health
|
facilitate ↔ hinder
give priority ↔ give no priority
|
|
Explanation of pain
|
internal ↔ external
|
|
Strategies for pain control
|
Balancing pain
|
adjusting ↔ ignoring
|
|
Concealing pain
|
telling no one ↔ telling significant others
|
|
Disruptions in daily life
|
Mental strain
|
reminder ↔ hindrance
|
|
Body as obstruction
|
reminder ↔ hindrance
|
Striving to master variable pain
The informants described how they were constantly “striving to master variable pain”. The core category contains the properties: “variable pain”, “thoughts about the future” and “attitudes to pain”. “Variable pain” was described as a constantly present low- to-moderate dull pain located in the neck-and-shoulder region. A prominent feature was the existence of periods of deterioration and the pain was often unpredictable. The descriptions included other bodily sensations, such as stiffness, headache, numbness in the arms, and vertigo.
“Someone [the pain] is constantly arguing with you, never leaves you. And you try to say “Stop! Leave it! I can’t bear this! “and you try to get away, but you can’t. This someone is following you, keeps on bothering, bothering you – that’s how it is.” [9, m]
In “thoughts about the future”, the informants expressed hope for improvement or to keep the pain in check, but they did not believe in full recovery. Worries about future deterioration and being unable to continue with their work were described, as were concerns about the eventual negative effect of working despite pain and not going on sick leave. The informants also described different “attitudes to pain”: to the fact that the pain existed, might persist and to the recurrent nature of the pain. The “attitude to pain” was spread along a continuum; 3 examples of variation are given below. Incorporation into their lives of the consequences of pain and the periods of deterioration were described.
“Having some pain has become a part of everyday life. I live with pain without letting it hinder me except when it’s getting worse…then the pain mainly affects my mood and it sometimes restricts me from doing things.” [6, f]
Living life as before despite acknowledging the pain, e.g. ignoring one’s limitations, was also described.
“I’m not directly affected – I haven’t made any changes just because I’m in pain – I live with it. So I can manage to go to work, I enjoy my job, and that’s why I don’t want to report sick. “ [2, m]
Not having adjusted to the pain and its recurring nature led to a variety of behaviour, e.g. ignoring one’s physical limitations.
“Above all, I don’t want my body to stop me from doing things. It feels terribly annoying; I don’t want it to become a hinderance.” [11, f]
Space for health
When trying to control their pain, the informants described the importance of having “space for health”. This sub-category comprises 3 properties: “working and living conditions”, “priority for health”, and “explanation of pain”. “Working and living conditions” comprises the working environment and family situation that influenced, e.g. the amount of time available to spend on health-promoting behaviour in relation to the pain. The informants highlighted the need for adequate time to recover from work, taking breaks at work, seeing healthcare professionals, doing home exercises and being physically active. An obstacle to adequate time for taking care of one’s own health was a stressful lifestyle.
“When you have a very stressful lifestyle, like I had, all of life becomes very difficult. You don’t have enough time to recover from day to day, you sleep less because you have so much to do…” [7, m]
Having small children meant that there was limited time for taking care of one’s own health. Physical training or seeing the physiotherapist left little time in the daily schedule.
“Since I’m on parental leave, I’m expected to see the physiotherapist in the middle of the day. That stresses me, because then I have to arrange for someone to look after my boy and I have a bad conscience just being away for an hour…” [10, f]
The issue of allowing oneself to prioritize one’s own health in relation to pain was highlighted by the informants. Regardless of their situations in life, women and men described the issue somewhat differently. The women stressed how they had difficulties in prioritizing their own health in relation to the pain.
“In my situation I prioritize my children…my job is important and.. my wonderful husband…and then I have to handle all this in some way…so you just have to cope, your body should not be an issue.” [11, f]
“You have to try to get time for physical training, either in the evening or if you take an hour off work…or just try to be physically active somehow during the day…” [12, m]
The property “explanation of pain” included the informants’ beliefs regarding what caused the pain. They ascribed external causes of the pain to their occupation, to a specific instance of heavy lifting or to monotonous movement.
“My job is pretty strenuous…there’s a lot of carrying, I’m bending over, serving coffee with my right arm …of course you get problems. I’m not surprised that I’ve got these problems.” [3, f]
In addition, the women stressed internal causes of the pain. Factors related to their own bodies were expressed such as being small, weak and undergoing hormonal variations.
“I think it’s a combination…I’m told my back is hyper-mobile and in combination with incorrect sitting …” [6, f]
“Everything is made for men over 1.80 [metres] …if you are 1.56 [metres], the working environment can never be optimal…and then it turns out like this…” [11, f]
Strategies for pain control
Strategies used to control the variable pain were described in the sub-category “strategies for pain control”. This contains 2 properties: “balancing the pain” and “concealing the pain”. “Balancing the pain” comprises variations of physical behaviour and how the informants sought primary care in times of deterioration. Adjustments in physical behaviour at work and at home could include work tasks, doing a little at a time and accepting help with pain-provoking chores from others. Part-time sick leave or disability pension were options. Ignoring pain, working and being physically active despite pain, were also described.
“I try to be mindful in everything I do at work and observe what is going on in my body. If possible I try to stretch the muscles in my head and do some movements.” [4, m]
“I haven’t changed my behaviour at work, no…when the pain gets too heavy I call the physiotherapist…I don’t want to go on sick-leave, I’d rather work with the pain instead.” [2, m]
For those who practised physical training before the onset of pain, adjusting the training was one strategy to balance the pain. These informants managed their physical training on their own. Body awareness therapy was mentioned. Awareness of the possibly positive effects of relaxation training during the day was mentioned, but this training was seldom practised. The informants described mostly considerable confidence in their ability to control pain, except when it was experienced as too much of an obstacle to daily life.
“’Can you please help me because I can’t handle this any longer…’ I guess you wait a bit too long before you call for help. You should really go earlier, but you always think that you’ll manage it on your own.” [4, f]
The property “concealing the pain” included avoidance of complaints to others, i.e. only closest family, friends and colleagues knew about the pain. The informants found it difficult for others to understand. Talking about it drained them of energy and sometimes reinforced the pain.
“Sometimes you don’t want to talk about it, because you feel whiny and troublesome…and at the same time it’s hard for someone else to understand how it feels.” [6, f]
Disruptions in daily life
The sub-category “disruptions in daily life” contains 2 properties: “mental strain” and “the body as an obstruction”. It encompassed how the pain had physical, psychological and social effects, thus leading to disruptions in areas of daily life. The disruptions varied from a reminder to a hindrance.
“You don’t join in in the same way …often it (the pain) hasn’t held me up entirely: I do join in, but I don’t get as much benefit from it.” [6, f]
“My pain and my problems go in waves a great deal, and when they’re worst it can be difficult to push my children on the swings in the park, it’s hard to carry things and above all when it’s really irritated I have problems working at work. Because I sit in front of a computer and it’s that type of work, so it gets incredibly, terrifically painful.” [11, f]
“Mental strain” was described as tiredness and decreased memory function. Decreased concentration was common and the informants were reportedly less tolerant of stress both at work and at home. The pain often led to an irritable mood: they had to struggle to prevent their irritation from affecting interaction with others.
The “body as obstruction” included how the pain had consequences for the informants’ everyday physical capacities, occupational and private. In periods of intense pain they experienced difficulties with fairly heavy manual handling or monotonous keyboard work. Furthermore, they reported being unable to continue with their regular physical training. They did not experience any major consequences socially. The pain had little effect on night sleep except when it was intense. At the domestic level, men and women described the consequences somewhat differently. The women experienced difficulties with physically demanding housework chores, e.g. cleaning, cooking and carrying small children. The men’s descriptions were related mainly to heavy carrying and maintenance, e.g. gardening.
“It [the pain] affects chores at home…you can’t iron for example, because then you are bending your neck. To make a cake or to vacuum clean can be difficult…you have to avoid bending your neck and looking down…” [1, f]
“We have a house in the country and when working in the garden, for example raking or chopping down trees, of course it’s painful…” [7, m]
DISCUSSION
The main findings of this study concern how the informants were constantly trying to master the variable pain, in order to not let it become too much of a hindrance in daily life. They also showed different attitudes towards the pain. The nature of recurrence was experienced as a challenge to be mastered, especially as periods of deterioration could lead to consequences and to disruptions in daily life. The search for control of pain seemed to require adequate time and prioritizing one’s own health in relation to the pain. Perceived causes of the pain seemed to be of importance. Different pain-control strategies were described. Women and men described the consequences of pain and difficulties in adopting strategies somewhat differently.
Findings
The informants described different attitudes towards the pain and therefore showed different ways of adjusting to its intrusion into their lives. This is in accordance with the concept of normalizing, which deals with adjustment to a present situation (25) and, in this context, living with long-term pain with periods of deterioration. Symptom control and behavioural change, i.e. monitoring physical boundaries and pacing, become the norm. For some people normalization means letting plans go and scaling down life; for others it means struggling with illness to achieve future goals. The present informants can be seen as having “normalized” to the pain and the related disability in various ways. Gullacksen & Lidbeck (26) describe the process of adjustment to long-term musculoskeletal pain. During the first phase the pain becomes an intruder in the individual’s life. There is still hope for improvement, but also worries for the future. In the second phase the pain is recognized as not being temporary; and in the third phase there is consideration of the future, which includes adjustment to pain. The present informants were placed along the continuum of adjustment. One end-point was not having adjusted to the pain and its recurrent nature, often described as exceeding their physical limitations and resulting in deterioration and frequent recourse to healthcare. The opposite end-point was the informants’ adjustment to the consequences of their pain, e.g. pacing and adjusting their physical behaviour. However, these informants sometimes also needed support from health professionals in their endeavour to master the pain. The present informants were to be found in all the phases described by Gullacksen & Lidbeck (26), but mainly the first. One reason for not adjusting to long-term NSP might be the dominant feature of variation in pain intensity and pain-related disability.
Self-efficacy refers to a person’s confidence to engage in a course of action sufficient to accomplish a desired outcome, such as control of pain. This varies considerably among persons with pain (27). The present informants tried to control the pain themselves, seeking care in periods of deterioration. They expressed hope for improvement or confidence to keep the pain in check, but they did not believe in full recovery. Great worry for the future and low confidence in controlling the pain were, however, also described. Since self-efficacy is an important determinant of disability for people with musculoskeletal pain in primary care (28), deeper understanding of self-efficacy and its effect on controlling regional variable pain should be sought in further research.
The informants described how they tried to master long-term variable pain using different strategies. The term “self-management” deals with the activities people perform to create order, discipline and control in their lives (29). The literature on self-management has focused mainly on arthritis, but is assumed to be relevant for other long-term conditions. An interview study by Kralik et al. (29) shows that important aspects of self-management were contextual and involve finding ways to live life optimally. Self-management included planning, prioritizing and pacing activities so as not to aggravate the pain. The present informants perceived lack of time due to high demands at work, a stressful lifestyle and having small children as obstacles to self-management and their own health in relation to pain. The issue of allowing oneself to prioritize healthcare in relation to pain was also highlighted. These obstacles can be seen as important contextual factors affecting the self-management of long-term variable pain.
The women, more than the men, stressed difficulties in prioritizing their own health in relation to pain. This has been highlighted in other studies, which show that women with musculoskeletal disorders describe how difficult it is to put themselves first in taking care of their health, being obliged to limit their participation in rehabilitation because of their domestic responsibilities (30, 31). Domestic factors, it has been suggested, affect men’s and women’s rehabilitation processes differently (30) and influence the outcome of rehabilitation in favour of men (32).
Malterud et al. (33) introduced the concept of “self-assessed personal health resources”. This is defined as the individual’s subjective experience and perception of qualities or strategies thought to maintain health. In a clinical setting, self-assessed personal health resources may be identified and contribute to managing health. In a study comparing self-assessed health resources between men and women, the results indicate that there are gender dissimilarities in self-assessed health resources (33). One example is that, for men, personal strength was part of a proud identity, while women were able to manage simply because they had to. All our informants ascribed the cause of their pain to physical factors and, in addition, women adduced their own bodies. This ascription might influence one’s self-assessed health resources, whereas pain control might be easier with a behavioural change if one perceives an evident external cause of the pain, rather than an internal one. Ahlgren & Hammarström (32) suggest that the attribution of the cause could be regarded as a factor directing the rehabilitation process. However, the effect of attribution of cause on self-assessed personal health resources needs further exploration.
During periods of deterioration, the present informants described pain-related difficulties in performing physically demanding tasks at work, privately and in the home. The property “body as obstruction” has formerly been shown in phenomenological-hermeneutic research when investigating experience of living with fibromyalgia (13), but seemed appropriate for the present study. Individuals with fibromyalgia and other widespread pain conditions emphasize how pain influences their whole lives, and how the accompanying fatigue affects their social life and disturbs their sleep (13–15, 31). In contrast to life with widespread pain, remissions associated with variable pain seemed to allow for some pain relief and recovery, as also shown in earlier studies (15, 16).
Men and women described domestic consequences somewhat differently. Women with persistent widespread pain conditions or fibromyalgia report difficulties with housework and dependence on family members for help with these tasks (13, 33). Interviews with men with any pain condition are rare, but in one study (14) men with fibromyalgia describe no consequences for housework. Women often describe themselves as having and taking the main responsibility for household duties (30, 34), which may be a reason why consequences of pain for household work become more apparent for women than for men.
Methods
To ensure transferability, purposeful sampling was carried out (19–20). The informants were both white-collar workers and blue-collar workers, city dwellers, and only one had a foreign background. The results might therefore not be considered transferable to people with foreign background or to people living in suburbs or rural areas.
Clinical implications
In order to support people with long-term pain to control pain and reduce the consequences in daily life, both biological and psychosocial aspects need to be addressed. The present findings highlight some aspects of living with regional, long-term and variable pain, which could have clinical implications for professionals working in primary care.
• Individuals seeking primary care for regional, long-term and variable pain have learned to live with this in different ways: and this should be taken into account in the rehabilitation process. One way to prevent the development of a more persistent and widespread pain condition could involve awareness of the effect of self-efficacy on disability.
• Giving oneself enough time and prioritizing one’s own health in relation to pain, and the perceived cause of the pain may be important aspects affecting self-management. These aspects may, when needed, be discussed with patients.
• Using a gender-sensitive approach in primary-care rehabilitation could be of importance when constructing individualized rehabilitation programmes.
In conclusion, living with long-term, variable NSP involves a struggle not to let the pain become too much of a physical obstacle to daily life. Individuals learn to respond to the pain in different ways using different strategies. Giving oneself adequate time and prioritizing one’s own health in relation to pain seem to be important contextual factors for controlling pain and should be taken into account in the rehabilitation process.
ACKNOWLEDGEMENTS
We wish to thank KvartersAkuten Matteus, Department of Rehabilitation Medicine Stockholm, Danderyd University Hospital. Karolinska Institutet, Department of Clinical Sciences, Danderyd Hospital, Division of Rehabilitation Medicine and Department of Neurobiology, Care Sciences and Society, Division of Physiotherapy, Stockholm, for making this paper possible. We would also like to thank Gabriele Biguet at the Division of Physiotherapy for valuable comments on the manuscript and Lisbeth Broman, Division of Rehabilitation Medicine, for designing the figure. Finally, we thank all the women and men who participated in this research.
REFERENCES



