Christopher Kevin Wong, PT, PhD, OCS1, Stanford T. Chihuri, MPH2 and Guohua Li, MD2
From the 1Department of Rehabilitation and Regenerative Medicine and 2Center for Injury Epidemiology and
Prevention, Columbia University Medical Center, New York, NY, USA
OBJECTIVE: To assess fall-related injury risk and risk factors in people with lower limb amputation.
DESIGN: Prospective longitudinal cohort with follow-up every 6 months for up to 41 months.
SUBJECTS: Community-dwelling adults with lower limb amputations of any etiology and level recruited from support groups and prosthetic clinics.
METHODS: Demographic and clinical characteristics were obtained by self-reported questionnaire and telephone or in-person follow-up. Fall-related injury incidence requiring medical care per person-month and adjusted hazard ratio of fall-related injury were calculated using multivariable proportional hazards regression modeling.
RESULTS: A total of 41 subjects, with 782 follow-up person-months in total, had 11 fall-related injury incidents (14.1/1,000 person-months). During follow-up, 56.1% of subjects reported falling and 26.8% reported fall-related injury. Multivariable proportional hazard modeling showed that women were nearly 6 times more likely as men to experience fall-related injury and people of non-white race were 13 times more likely than people of white race to experience fall-related injury. The final predictive model also included vascular amputation and age.
CONCLUSION: Risk of fall-related injury requiring medical care in people with lower limb amputation appears to be higher than in older adult inpatients. Intervention programs to prevent fall-related injury in people with lower limb amputation should target women and racial minorities.
Key words: balance and falls; injury; amputation; prostheses; prognosis; health status disparity.
J Rehabil Med 2016: 48: 80–85
Correspondence address: Christopher Kevin Wong, Department of Rehabilitation and Regenerative Medicine, Columbia University Medical Center, Neurological Institute 8-822, 710 West 168th Street, New York, NY 10032, USA. E-mail: ckw7@cumc.columbia.edu
Accepted Oct 14, 2015; Epub ahead of print Dec 22, 2015
INTRODUCTION
Fall-related injury accounts for 20% of the nearly $20 billion annual cost of accidental injury in the USA (1). Although incidence increases with advancing age (2), fall-related injury affects all age groups (3) and occurs in both indoor and outdoor settings among community-dwelling individuals (4). People with lower limb amputations, a population expected to double to 3.6 million by 2050 (5), have heightened risks of falling compared to able-bodied individuals. While a study found that approximately 26% of a community-dwelling people, ranging in age from 20–92 years, had fallen (3), the annual incidence of falls in community-dwelling people with lower limb amputations is approximately double (6, 7).
Despite prosthesis use, limb loss places the person with lower limb amputation at a disadvantage. Retrospective studies of falls in people with amputations report associations with impaired balance ability (7), lower balance confidence, and decreased social participation (6). A limitation of any retrospective or cross-sectional study assessing balance confidence and ability, while recording a history of falls, is that a past fall can confound self-reported confidence, social activity, and physical ability at the time of self-reporting or testing. People who have fallen in the past may report less confidence, while those with more confidence and ability may participate in more activities regardless of past falls. Indeed, community-dwelling prosthetic users who fall most have been found to be younger, more confident individuals with better balance (7).
Individuals with lower limb amputations with better functional balance ability may feel more confident to access their communities and engage in activities that might expose them to falls, especially when past falls were not associated with injury. In fact, many people who fall do not get injured. Falls and recurrent falls do not correlate closely with incidence of injury (7, 8). Cross-sectional or retrospective studies investigating falls in people with lower limb amputations have yielded a variety of odds ratios for various factors to explain a history of falls (6, 7). However, self-reports of past falls, considered together with data obtained at a single time-point, inescapably confound the contributing variables with the fall occurrence. Models derived from cross-sectional and retrospective designs, statistically predict variations in a variable, such as history of falls, without a longitudinal time component to give insight into future occurrences.
No prospective longitudinal multivariate analysis assessing risk for falls and fall-related injury in community-dwelling people with lower limb amputations was identified. The purpose of this study was to explore the factors that predispose community-dwelling people with lower limb amputations to experience fall-related injury severe enough to require medical care in a prospective study with a follow-up of up to 4 years, using multivariate analysis with Cox proportional hazards regression. The aims were: (i) to determine the incidence of fall-related injury over time in sample of community dwelling individuals with lower limb amputation; and (ii) to identify a predictive model for fall-related injury in people with lower limb amputation.
METHODS
This prospective longitudinal cohort study was conducted according to the protocol approved by the Institutional Review Board of the participating university medical center.
Subjects
The convenience sample for this study was recruited from local prosthetic clinics and support groups in the metropolitan area of the participating medical center. The study included community-dwelling adults with bilateral or unilateral lower limb amputations of any etiology or surgical level. Subjects with medical issues that affected balance, including uncontrolled cardiovascular disorders, neurological disorders, such as stroke or vestibular disorders, blindness, or cognitive disability, that prevented understanding of the study were excluded. The 5–10 subjects per variable guideline determined sample size (9).
Measures
After providing informed consent, subjects attended an initial out-patient assessment session at the participating university medical center to complete a demographic and medical information questionnaire, self-report prosthetic use for mobility and balance confidence scales, and complete a performance-based balance assessment. Follow-up data were obtained by telephone or in-person communication at support group meetings or prosthetic clinic visits every 6 months (±2 months) from October 2009 through April 2014 for periods of up to 4 years.
The primary outcome measures, obtained at follow-up, were self-reported falls and fall-related injury. Falls were defined as an unintentional loss of balance resulting in the individual coming to rest on the ground (6) and were counted from the last communication points. Fall frequency was categorized as no fall, a single fall (no more than 1), or repeated falls (more than 1) during the study. Fall-related injury severity was defined as requiring no medical care, a visit to the emergency room or physician, or hospitalization or surgery.
Medical information obtained at initial assessment included: age, sex, race, weight, height, medical comorbidities, amputation etiology and level, years-since-amputation, prosthesis use, and number of falls in the past 12 months. Research personnel were present at the initial assessment to assist or answer questions for all subjects during self-reported data collection.
Prosthetic use for mobility was assessed with the Houghton scale. The self-reported Houghton scale quantifies daily prosthesis wear, use of the prosthesis and walking aids, and perceived stability walking with the prosthesis on various terrains (10). Scores on the 4-question Houghton scale are added together, with the total score ranging from 0 to 12. Higher scores indicate better function, with scores of 9 or greater suggested to represent satisfactory outdoor prosthetic use (10). Scores on the Houghton correlate moderately with physical walking ability measures, such as the Timed-Up-and-Go and 2-Minute-Walk-Test (11, 12), with moderate internal consistency (11), excellent test-retest reliability (12), and responsiveness to change after rehabilitation (11).
The subjective perception of balance confidence was assessed with the self-reported Activities-specific Balance Confidence (ABC) scale. Percent confidence when performing 16 common activities of daily life was averaged to describe the individual’s subjective confidence in maintaining balance when they perform the activities (13) that range in difficulty (14). Use of the ABC has been investigated in people with lower limb amputations, and validity (11) and reliability (12) has been established.
After completing the self-reported ABC and Houghton scales, balance ability was assessed by testers trained to administer the Berg Balance Scale (BBS) to people with limb loss. The 14 static and dynamic balance tasks of the BBS were scored from 0 to 4 with the total score reported (15). Scores range from 0 to 56 and distinct balance ability strata for people with lower limb amputations have been described, with those scoring 54–56 having the best balance and those 0–32 having the worst (16). The validity and reliability of the BBS to assess balance in people with lower limb loss has been documented (16–18).
Statistical analyses
Kaplan–Meier survival function estimates and non-parametric log rank tests were used to test proportional hazards assumptions and explore individual effects of several variables on fall-related injury incidence. Fall-related injury was defined as an injury sustained during a fall to the ground during the study period requiring medical care by a doctor or in an emergency room, or requiring hospitalization or surgery.
Demographic information (age, sex, race) and variables deemed clinically important for people with lower limb amputations (amputation etiology, amputation level, years since amputation, balance confidence/ABC score, prosthetic use/Houghton score, and fall history) were compiled for descriptive analysis. For Kaplan–Meier analyses, age, ABC scores, Houghton scores, and years since amputation were continuous variables; sex, etiology, race, and level of amputation were dichotomous. Cox proportional hazard models were sequentially created to include variables demonstrating univariate statistical significance. Likelihood ratio tests compared nested models. Hazard ratios (HR) with 95% confidence intervals (CI) were calculated. Subjects who did not provide follow-up data or who died were excluded from the analyses. Analyses were performed in SAS 9.4 (SAS Institute, Cary, NC, USA).
RESULTS
An initial total of 54 subjects were recruited. One subject died and 12 were lost to follow-up, thus 41 were included in the analyses. By study end, 56.1% (23/41) reported at least a single fall, 26.8% (11/41) had experienced a fall-related injury requiring medical care. The incidence of fall-related injury was 14.1 per 1,000 person-months (11/782 person-months; 95% CI 6.0–32.5/1,000 person-months).
Table I shows the sample characteristic distributions by injury status. Mean age was 56.9 years, ranging from 34 to 82 years. Mean time since amputation was 6.7, ranging from 0 to 46 years. Most subjects were men, and had transtibial amputations, and vascular etiologies. Over 50% of subjects had reported a history of at least one past fall within the previous 12 months in both the injured and uninjured groups.
|
Table I. Sample characteristics at baseline according to injury status by the end of the study period |
||||
|
Characteristic |
Total n = 41 |
Injury n = 11 |
No injury n = 30 |
Kaplan–Meier log rank p-value |
|
Age, years, mean (SD) |
56.9 (11.8) |
54.7 (13) |
57.7 (11.5) |
0.19 |
|
Sex, n (%) |
||||
|
Male |
24 (58.5) |
3 (27.3) |
21 (70) |
0.05* |
|
Female |
17 (41.5) |
8 (72.7) |
9 (30) |
|
|
Race, n (%) |
||||
|
White |
14 (34.2) |
2 (4.9) |
12 (29.3) |
0.034* |
|
Non-White |
27 (65.9) |
9 (22.0) |
18 (43.9) |
|
|
Etiology, n (%) |
||||
|
Vascular |
29 (70.7) |
10 (24.4) |
19 (46.3) |
0.11 |
|
Non-vascular |
12 (29.3) |
1 (2.4) |
11 (26.8) |
|
|
Level, n (%) |
||||
|
TFA/bilateral TFA |
14 (36.8) |
3 (7.9) |
11 (29.0) |
0.21 |
|
TTA/bilateral TTA |
24 (63.2) |
8 (21.1) |
16 (42.1) |
|
|
Years since amputation, mean (SD) |
6.7 (10.9) |
5.9 (13.7) |
7.0 (10.0) |
0.74 |
|
ABC, mean (SD) |
63.9 (30.2) |
57.6 (32.7) |
66.3 (29.4) |
0.001* |
|
Berg Balance Scale, mean (SD) |
40.9 (15.8) |
38.1 (12.21) |
42.0 (17.0) |
0.01* |
|
Houghton score, n (%) |
||||
|
≥ 9 |
18 (43.9) |
3 (7.3) |
15 (36.6) |
0.33 |
|
< 9 |
23 (56.1) |
8 (19.5) |
15 (36.6) |
|
|
Falls in 12 months: n (%) |
||||
|
None |
18 (43.9) |
5 (12.2) |
13 (31.7) |
0.74 |
|
1 |
11 (26.8) |
4 (9.8) |
7 (17.1) |
|
|
≥ 2 |
12 (29.3) |
2 (4.9) |
10 (24.4) |
|
|
*Significant at p < 0.05 level. ABC: Activities-specific Balance Confidence scale; TFA: transfemoral amputation; TTA: transtibial amputation; SD: standard deviation. |
||||
Of the 11 subjects who had a fall-related injury, 10 had amputations of vascular etiology. Subjects injured during the study scored less, on average, on the ABC and BBS than those not injured. In subjects classified as unsatisfactory prosthetic users, based on a Houghton score of < 9, 72.7% (8/11) had experienced a fall, compared to 50% (15/30) of satisfactory prosthetic users. No statistical difference in injury incidence was found between prosthetic use classifications.
Less than half of the subjects (43.9%) did not experience a fall, while 29.3% had recurrent falls, as shown in Table II. Total follow-up time was 41 months. In total, 73.2% of the subjects received no care, either because they did not experience a fall or because they fell and had minor injuries not requiring medical care (Fig. 1). Greater fall frequency correlated with greater injury severity (r = 0.407, p = 0.008), which suggests that subjects with recurrent falls were likely to have more severe injuries that required medical attention.
|
Table II. Frequency distributions of frequency of falls and injury and severity medical attention required |
||
|
n (%) |
Cumulative % |
|
|
Injury severity |
||
|
No injury |
30 (73.2) |
73.2 |
|
Required visit to MD or ER |
6 (14.6) |
87.8 |
|
Required hospitalization |
2 (4.9) |
92.7 |
|
Required surgery |
3 (7.3) |
100 |
|
Fall frequency |
||
|
No fall |
18 (43.9) |
43.9 |
|
One fall only |
11 (26.8) |
70.7 |
|
Recurrent falls |
12 (29.3) |
100 |
|
MD: medical doctor; ER: emergency room. |
||
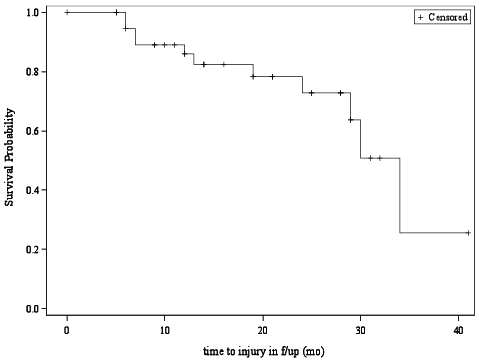
Fig. 1. Kaplan–Meier plot showing survival estimates for the cohort. f/up: follow-up; mo: months.
Fall-related injury throughout the study duration was predicted by a model including sex, race, age, and etiology of amputation (Table III). The injury rate among females was 5.88 times that among males throughout the study period (95% CI 1.30–26.51) when adjusting for race, age and amputation etiology. The injury rate among non-white people was 13.07 times that among white individuals (95% CI 1.0–165.7) when adjusting for race, age and amputation etiology. Amputation etiology did not remain a significant independent predictor (p = 0.07) when adjusting for sex, race, and age, but had a HR = 10.2 (95% CI 0.81–129.09). The injury rate decreased by 13.8% (95% CI –40% to +27.6%) for every 5-year increase in age, adjusting for sex, race, and amputation etiology. The most precise multivariate model to predict the hazard function for fall-related injury is shown in Table III.
|
Table III. Bivariate and multivariable hazard ratios (HR) for predicting fall-related injuries |
||||||
|
Variable |
Bivariate HR |
95% HR CI |
p-value |
Multivariate HR |
95% HR |
p-value |
|
Age at baseline |
0.97 |
0.91–1.02 |
0.21 |
0.97 |
0.90–1.05 |
0.44 |
|
Sex |
||||||
|
Male |
Ref |
|||||
|
Female |
3.52 |
0.93–13.34 |
0.065 |
5.88 |
1.30–26.51 |
0.02* |
|
Race |
||||||
|
White |
Ref |
|||||
|
Non-white |
7.67 |
0.89–65.76 |
0.063 |
13.07 |
1.03–165.76 |
0.047* |
|
Etiology |
||||||
|
Non-vascular |
Ref |
|||||
|
Vascular |
4.78 |
0.59–38.70 |
0.14 |
10.21 |
0.81–129.09 |
0.07 |
|
Amputation level |
||||||
|
TTA/bilateral TTA |
Ref |
|||||
|
TFA/bilateral TFA |
0.34 |
0.08–1.48 |
0.15 |
– |
||
|
Houghton score |
||||||
|
< 9 |
Ref |
|||||
|
≥ 9 |
0.52 |
0.13–2.02 |
0.34 |
– |
||
|
Years since amputation |
0.99 |
0.92–1.05 |
0.65 |
– |
||
|
ABC |
0.99 |
0.98–1.02 |
0.61 |
– |
||
|
Berg Balance Scale |
0.99 |
0.95–1.03 |
0.54 |
– |
||
|
*p < 0.05 level. ABC: Activities-specific Balance Confidence scale; TFA: transfemoral amputation; TTA: transtibial amputation; CI: confidence interval; HR: Hazard ratios. |
||||||
DISCUSSION
This prospective longitudinal study examined the incidence and hazard risk of fall-related injuries requiring medical care over time in community-dwelling people with lower limb amputations. The fall-related injury incidence of 14.1/1,000 person-months in this study (46.2/100,000 days) represents a significant problem when compared to other at-risk populations. For instance, the incidence of major fall-related injuries in hospitalized elderly people ranged from 10/100,000 days for those 65–74 years old to 30/100,000 days for those 75 years of age and older (19). Hospitalized people with lower limb amputations have been reported to be at even higher risk, with 180 fall-related injuries per 100,000 person days (20).
Our results show that prospective fall-related injuries in community-dwelling people with lower limb amputations were predicted by a model that included sex, race, age and amputation etiology. Balance confidence and balance ability, both included in models that identified people with lower limb amputation who had a history of past falls, were not included in the predictive model for fall-related injury (7). Within the final model, fall-related injury was most likely to occur in women and individuals of non-white race. Within the study, the likelihood of experiencing fall-related injury was 5.88 times greater for women than men and 13.07 times greater for people of non-white than white race. Although people with vascular amputations had a HR > 10, the confidence interval was wide and amputation etiology did not remain a significant independent predictor when included in the model. The large HR was a strong indication that amputation etiology would have been significant had the sample size been larger. No other prospective longitudinal study of fall-related injury in people with amputations could be identified for comparison.
While people with vascular lower limb amputations in a hospital rehabilitation setting have demonstrated the greatest crude odds ratio (2.4) to indicate a fall, injury occurrence and severity was not considered in the retrospective analysis (21), making risk assessment for future fall-related injury uncertain. In people with unilateral trans-tibial amputations discharged home from rehabilitation after recent amputations, lower functional scores correlated with repeat falls at 6-months in a study that did not record fall-related injury (22). Past cross-sectional research has shown that people with non-vascular amputations had a greater likelihood to have reported repeated falls, not associated with injury, and had higher prosthetic functional use scores and significantly more years of prosthetic experience (7). While higher functioning community-dwelling individuals with lower limb amputations may fall repeatedly without injury (7), the results of the current study found that over an extended period of years increasing fall frequency correlated with greater fall-related injury severity. Women of non-white race, especially with a vascular amputation etiology, were at the greatest risk of serious fall-related injury although fall frequency did not remain in the model.
Vascular amputation etiology could be a factor because it may indicate lower overall health status. Over 70% of study subjects had vascular amputations and well over 30% of people with lower limb amputations (5) have diabetes or diabetes-related disease, making comparison useful. Like people with amputations in the study, people with diabetes have increased risk for fall-related injury (23). Diabetes and other general health comorbidities, such as hypertension, are known to be associated with minority race (24) and peripheral artery disease (25). In this study, even after adjusting for vascular etiology, non-white race was a significant independent predictor in the final model, with HR = 13.07 for injury resulting from a fall. Overall, a greater number of comorbidities was associated with both repeated falls (26) and fall-related injury after controlling for other factors in a retrospective study (27), although the association was weak (odds ratio = 1.4). A direct link between fall-related injury and non-white race was not identified in the literature related to the USA, although an association has been noted in native peoples in Ecuador (28).
In addition to non-white race, female sex was the other significant factor (HR = 5.9) in the overall model predicting fall injury over time. Older women have demonstrated a greater risk for fall-related injury (29) although women experience more injuries across all age groups (3). While falls occur in all ages, specific fall-related injuries vary with younger people injuring more distal extremities, middle-aged people injuring mostly knees, and older people injuring knees, but also experiencing head injuries (3). Women may be particularly vulnerable to fractures of the lumbar spine, pelvis and hip (30). Educational level can be a confounding variable, as women over 55 years of age with lower education levels were at greater risk, along with similar men over 60 years of age (31). Injurious falls among women were most common in the bathroom (32), with slips and trips related to rugs and carpets generally implicated (33).
The last variable included in the final model was age. Other research has shown that older age is associated with increasing rates of hospitalizations for severe injury due to falls (2). The results of this study found that age over 55 years was a significant univariate predictor, but did not remain significant as an independent variable in the multivariate model. For people with lower limb amputations, age may be a mediator of more than one variable. For instance, older age was associated with greater incidence of vascular disease and may occur with poor health, which, in people with lower limb amputation, may lead to decreased activity and thus reduced risk due to the decreased opportunity to fall. However, people who lose a limb due to trauma may otherwise be healthy and live long enough for advancing age itself to be a risk factor to fall regardless of amputation etiology. Older women who have greater fall-related injury risk, may be predisposed to greater risk of falls regardless of race or amputation etiology. The final model represents age as a continuous variable to allow for greater clinical utility and to ensure better comparability that may be lost when age is dichotomized in determining fall-related injury risk.
Fall-related injury can have unfortunate consequences for an individual’s quality of life. A major factor can be social deprivation, which has been documented after fall-related fractures (34). The social consequences of fall-related injury, such as social isolation related to lost mobility and ability to access the community environment, result in decreased quality of life beyond 9 months associated with age (35). In turn medical issues related to injury after falls have a cost, higher in women and mostly related to fractures, to the individual and society (36). Although this study did not systematically document circumstances leading to fall-related injuries, one subject fell getting out of bed and fractured her hip on the same side as the amputated limb and required surgery.
This predictive model for determining fall-related injury risk may impact patient prognoses, access to care, injury prevention, and associated medical cost. In hospital settings where most falls involved poor balance, a safety education program to reduce falls for adult in-patients following major lower limb amputation has been initiated (37). While no follow-up data were collected, fall prevention programs have been widely recommended (27, 37, 38). Fall prevention programs can result in fewer injurious falls (39) and reduce costs related to in-hospital fall injuries (40). In community-dwelling adults over 50 years of age, higher levels of physical activity decrease the risk of fall and injury (41). Interventions to increase physical activity in people (41) and patient safety education regarding common environmental factors implicated in slips, trips, and falls related to environment, such as bathroom rugs (32, 33), may also reduce fall-related injuries. The predictive model of fall-related injury over time in people with lower limb amputations may help clinicians in out-patient settings identify at-risk patients and determine the need for safety education, balance training, or fall prevention interventions.
This study was the first to determine injury risk related to falls in people with lower limb amputation; however, the study results should be considered in light of the limitations. The small sample size limited the number of variables considered for the final model. No attempt was made to specify the precipitating circumstances of the fall, the specific injury experienced, or the outcome of any recovery (42). Furthermore, a convenience sample was used and the clinic or support group from which the subjects were recruited was not recorded nor were current medications documented. In addition, the time of injury was approximate due to the self-reported data collection process without control for recall error. Minor injuries, such as scrapes and bruises, which did not require a visit to a physician or hospital and thus were unlikely to incur substantial healthcare costs, were not recorded, but may have had an impact on prosthetic function. The results observed in this data set suggest that larger studies are warranted in future to address these limitations and assess the effects of prevention strategies, such as wellness or physical therapy programs, prosthetic components, or safety education. Further study into the economic status of people with lower limb amputation and costs of fall-related injury may aid cost benefit analysis of such programs.
In conclusion, fall-related injury severe enough to require medical care is a significant problem for people with lower limb amputation, with incidence rates higher than in other at-risk populations. A model based on age, sex, race, and amputation etiology predicted fall-related injury over time. Further large studies are needed to thoroughly examine all factors associated with fall-related injuries in people with lower limb amputations. This research may determine future risk and enhance decision-making related to fall prevention patient education or physical intervention programs.
ACKNOWLEDGEMENTS
This research was supported in part by grant 1 R49 CE002096 from the National Center for Injury Prevention and Control, Centers for Disease Control and Prevention to the Center for Injury Epidemiology and Prevention at Columbia University.
REFERENCES
