Tim Pauley, MSc1, Michael Devlin, MD, FRCPC2,3 and Pamela Madan-Sharma, BSc.PT3
From the 1Nathan Clinical Research Institute, West Park Healthcare Centre, 2Division of Physiatry, Department of Medicine, University of Toronto, Toronto, and 3Amputee and Neurological Rehabilitation Services, West Park Healthcare Centre, Toronto, Canada
OBJECTIVE: To evaluate hip abductor strength-training for patients with unilateral transfemoral amputation.
DESIGN: Single-blind, cross-over (AB/BA) trial with randomization.
SUBJECTS: Seventeen patients with transfemoral amputation.
METHODS: Subjects completed 8-week programs of twice weekly hip abductor strength training or arm ergometry. Subjects were randomly assigned to receive either the experimental or active control intervention first. A physiotherapist blinded to group assignment conducted baseline and post-intervention assessments. The Timed Up & Go (TUG) test was selected as the primary outcome measure; secondary measures included the 2 Minute Walk (2MW), hip abductor strength, Activities Specific Balance Confidence Scale (ABC) and prosthetic use. A two-way cross-over ANOVA was used for baseline and post-intervention treatment comparisons.
RESULTS: There were no baseline differences between treatments for TUG, 2MW, ABC, Houghton scale, sitting or side-lying abductor strength (p > 0.05 for all), though supine strength was greater for the experimental treatment (p < 0.05). After 8-weeks of hip abductor strength training, there were significant treatment effects for TUG, ABC (p < 0.01 for both), 2MW (p < 0.05), sitting and side-lying abductor strength (p = 0.05 for both), but not for supine strength, prosthetic use, nor thigh girth measures (p > 0.05 for all).
CONCLUSIONS: This study suggests that patients with unilateral transfemoral amputation can improve functional performance and balance confidence following intense hip abductor strength training.
Key words: amputation; amputees; hip abductor; resistance training; functional performance; balance confidence.
J Rehabil Med 2014; 46: XX–XX
Correspondence address: Tim Pauley, West Park Healthcare Centre, 82 Buttonwood Ave. Toronto, ON, M6M 2J5 Canada. E-mail: Tim.pauley@westpark.org
Accepted Oct 10, 2013; Epub ahead of print Dec 19, 2013
INTRODUCTION
Lower limb amputation results in neurophysiological and biomechanical changes (1). For example, proprioceptive feedback through the amputated limb is obliterated distal to the site of amputation, though factors such as muscular strength of the intact musculature of the residual limb are modifiable with appropriate therapeutic exercise.
Lower limb amputation rehabilitation requires an extensive period of adjustment to the use of a prosthesis and is often accompanied by fear of falling (2) and reduced quality of life (3). Any or all of these factors may contribute to reduced activities of daily living (ADL) (4). ADL reduction in turn likely contributes to detraining and atrophy which further restricts the ability to perform ADLs independently. Lower limb loss has been associated with muscle atrophy ranging from 40–60% in the sectioned muscle groups as well as up to 30% for intact hip stabilizers proximal to the amputation (5), the latter suggesting that strength loss is not a direct result of the amputation surgery, but likely also affected by other contributing factors such as reduced activity. Patients with lower limb amputation also demonstrate structural changes to the proximal muscle groups, including lower thigh bone-free lean body mass and higher percent thigh fat (6), both of which have been linked to poorer ambulation among able-bodied older adults (7), while atrophy of the hip-stabilizing muscles has been shown to contribute to greater gait asymmetry among patients with transfemoral amputation (TFA) (8). As a result, the capacity for isometric torque production by the abductors on the prosthetic side is as much as 30% less than the intact side (9), leading to an asymmetric stance, with 55% to 70% of body weight distributed over the intact leg, and poor medio-lateral centre of pressure control (10). This loss of strength is also thought to be the main cause of Trendelenburg gait (11), commonly observed among patients with lower limb amputation. As leg weakness has been causally linked to falls among older adults (12), maintenance of lower limb strength is critical for patients with amputation.
Though lower limb musculature strength has been identified as a factor related to functional performance (13), a literature search identified only a single trial investigating a 10-week, twice weekly training program for patients with TFA (14) as well as a single case study of strength training for a patient with a left unilateral upper and lower limb amputation (15). While these studies were able to demonstrate improvements in hip strength and oxygen consumption, and leg press strength, respectively, neither evaluated the impact of training interventions on functional outcomes typically utilized by clinicians to evaluate therapeutic progress. This study investigated an abductor strength training program designed to improve functional performance, as measured on the Timed Up & Go (TUG) primary outcome measure, as well as the secondary measures of abductor strength, 2-Minute Walk (2MW) and prosthetic use. Balance confidence was included to test for changes in perception of postural control. The following null hypothesis was tested: relative to the control treatment, subjects will demonstrate no improvement in primary or secondary outcome measures at the completion of the experimental intervention.
METHODS
Subjects
Six patients with right and 11 with left unilateral TFA (age 67.8 years (standard deviation (SD) 5.2) were recruited. Subjects’ demographics and select clinical characteristics are included in Table I. Experimental subjects had undergone unilateral, TFA secondary to diabetes or peripheral vascular disease, were 65 years or older, 6-months post-fitting with a prosthesis, ambulatory prosthetic users, taking no medications that may impair balance, able to complete all testing procedures, and not involved in a concurrent exercise program. This study was approved by the Research Ethics Boards at West Park Healthcare Centre and St. John’s Rehabilitation Hospital.
|
Table I. Demographic and clinical data of study participants (n = 17) |
|
|
Characteristic |
Subjects |
|
Gender, male, n (%) |
13 (76) |
|
Age, mean (SD) |
67.8 (5.2) |
|
Side of amputation, right, n (%) |
6 (35) |
|
Time since amputation, years, mean (SD) |
7.3 (8.2) |
|
Residual limb length, cm, mean (SD) |
31.6 (4.7) |
|
Residual limb length, proportion ht, mean (SD) |
0.19 (0.02) |
|
SD: standard deviation. |
|
Procedures
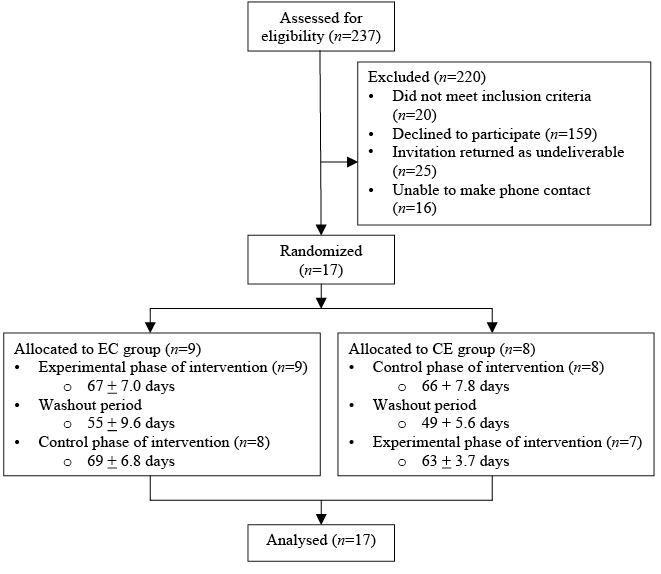
This study utilized a single-blind (evaluator), cross-over trial (AB/BA) with randomization. Subjects were randomised using the random numbers generator function in Microsoft Excel [i.e., = RAND()] by the study Principal Investigator who was not involved in data collection or subject orientation/supervision. Group assignment was conducted by the study Research Assistant (RA). Subjects fitting the study inclusion criteria were identified by clinical staff and sent a letter with a description of the study and invitation to contact the study coordinator if interested in participating. Patients expressing an interest were invited to West Park Healthcare Centre where informed consent was obtained by the study coordinator. TFAs were randomly assigned to receive either the experimental (EC group; n = 9) or control interventions first (CE group; n = 8). A Consolidated Standards of Reporting Trials (CONSORT) flow diagram describes recruitment and compliance (Fig. 1).
Baseline and post-intervention assessments included the Timed Up and Go (TUG) (16), Two-Minute Walk (2MW) (17), and hip abduction strength. For the TUG, upon the “Go” command, subjects rose from a chair, walked forward for 3 m, turned, and returned to the seated position. The 2MW was conducted in one direction only (i.e., no turning) in an approximately 200-m corridor. The distance was measured from the start position until 2 min had expired. Hip abductor strength measures were taken in accordance with the manufacturer’s instructions for use of the microFET2 digital handheld muscle dynamometer. Subjects were tested while sitting, side-lying and in a supine position on a hospital plinth. Strength measures were repeated three times with the mean utilized in the analysis. Thigh girth was measured 15% of height distal to the iliac crest. Secondary measures included the Activities Specific Balance Confidence Scale (ABC) (18) and the Houghton scale of prosthetic use (19). Baseline and post-intervention assessments were conducted by a physiotherapist (PT) blinded to group assignment. Prior to assessment the study RA cautioned each subject not to reveal group assignment to the PT, if known. Upon completion of the baseline assessment subjects were oriented to, and instructed on the use of the training equipment for the treatment to which they had initially been assigned. Post intervention assessments were conducted on the next regularly scheduled visit following the final training session.
Apparatus
This study utilized a commercially available Cybex Hip Abduction machine (Cybex International, Inc., Medway, Ma, USA). The pads, against which force is typically applied by the lower femur to operate the machine, were elongated such that a laterally directed force could be applied with proximal half of the femur without dislodging the prosthesis (see Figs 2a and 2b for anterior and posterior oblique views of the modified hip abductor). A Keiser M3 stationary cycle-ergometer (Keiser Corporation, Fresno, CA, USA) was used for warm-up purposes. This cycle ergometer was selected for its direct drive mechanism (i.e., with no “coast” capability, pedals continued to rotate when pressure was no longer applied by the rider) and toe-clips, thus allowing patients to cycle with the prosthesis donned without fear of imbalance or dislodging the prosthesis. A table mounted arm ergometer (Accessible Fitness Systems, Model AFS 301, Safety Harbor, FL, USA ) was used during the control treatment. The microFET2 (Hoggan Health Industries, Salt Lake City, UT, USA) dynamometer was used to obtain abductor strength data.

Fig. 2. Modified hip abductor machine (Cybex International, Inc.), indicating elongated hip abductor pads. Figs 2a and 2b show the anterior and posterior oblique views, respectively, of the modified hip abductor.
Hip abductor training (experimental treatment)
Though no specific recommendations for strength training of lower limb amputees are available, the American College of Sports Medicine (ACSM) provides recommendations for older adults and the frail elderly (20). For these groups, the ACSM indicates high intensity strength training as a safe and effective means of improving functional and general health status and recommends resistance training at 80% 1 repetition max (1RM), 2–3 days/week, with 2–3 sets of each exercise. For purposes of establishing a safe exercise program for patients with amputation, the ACSM guidelines for sets and frequency were adopted, while a 10RM target was used in place of the 80% 1RM target. Subjects started their initial hip abductor strength training session with no resistance followed by incremental increases in 5-pound intervals. At each resistance setting, the patient was asked to carry out 10 repetitions. This continued until 10 repetitions could not be completed in one continuous set. The highest resistance at which the patient could successfully complete 10 repetitions was considered the 10 RM.
Subjects attended twice weekly supervised training sessions for 8 weeks. Each session included a 5-min warm-up on a stationary cycle ergometer at 60 cycles/min against an electronic metronome. Resistance was titrated to achieve a target heart rate of 60% (using the Karvonen formula (21)) + 5 beats/min of age-predicted maximal heart rate. Subjects then performed 3 sets of 10 RM bilaterally on the hip abductor with their prosthesis donned. Resistance was progressively increased by 5-pound increments each time the individual was able to complete all 30 repetitions per training session. Each session lasted 15 to 20 min including the 5-min warm-up. The hip strengthening segment did not exceed 15 min for any subjects.
Arm ergometry (control treatment)
Control subjects underwent supervised arm ergometry training twice weekly for 8 weeks. Subjects exercised for 30 min/session at a 60 cycles/min against an electronic metronome. Resistance was titrated to achieve a target heart rate of 60% (using the formula by Karvonen et al. (21)) + 5 beats/min of age-predicted maximal heart rate. Ergometer resistance was adjusted periodically to ensure a consistent target training zone throughout the duration of training. Arm ergometry training was selected as an intervention that was expected to have no effect on the primary and secondary measures selected for this study. The arm ergometer was not calibrated throughout the trial.
All subjects received compensation for expenses related travel/parking costs associated with attendance at all sessions as well as a modest honorarium scaled in accordance with program compliance.
Analysis
Data were rank-transformed prior to inferential statistical analysis, to avoid violating the underlying assumptions of the ANOVA (22). Two 2-way cross-over ANOVAs were used for baseline and post-intervention treatment comparisons, thus controlling for sequence and period effects, where period 1 included the experimental and control treatments for the EC and CE groups, respectively, while period 2 included the control and experimental treatments for the EC and CE groups, respectively. Means and SD reported herein reflect the untransformed data; significance values reflect the results of the analysis on the transformed data. An intention-to-treat analysis using last observation carried forward was used to account for two subjects (one each from the CE and EC groups) who completed period 1, but opted not to transition to the alternative treatment condition. Minimal detectable difference based on 90% confidence interval scores (MDD90) were calculated from published data (16) for the primary outcome measure TUG to determine the proportion of subjects who demonstrated improvement in TUG scores which exceeded MDD during experimental and control treatments. A priori sample size calculation (23) determined that a minimum sample size of 17 subjects was required to achieve the appropriate power to detect statistical significant differences at p < 0.05 on the identified outcome measures. SAS for Windows, version 9.1 was used to conduct the analyses.
RESULTS
Compliance with the experimental protocol was 100% for 15 subjects who completed period 1 and period 2. Two subjects completed all 16 session of period 1 only. Eleven subjects missed a mean of 2.4 sessions (11 during experimental treatment, 15 during control treatment) due to inclement weather (n = 7), transportation issues (n = 7), or sickness (n = 12), though all missed sessions were made-up at a later date. There were no suspensions greater than two consecutive training days missed during either treatment for any subjects. The mean duration of treatments was 64.8 days (SD 5.6) for the experiment treatment and 66.5 days (SD 7.4) for the control treatment. There were no adverse effects associated with participation in the trial.
Two subjects (one from the CE group, one from EC) opted not to transition to the period 2 treatment upon completion of the period 1 treatment due to personal reasons. The CE subject was within one SD of the CE group mean on all baseline measures except the ABC (83.1 vs. 51.8 (SD 15.8)); at post-intervention this subject was within one SD of the CE group means on all measures. The EC subject was within one SD of the EC group mean on all baseline measures except side-lying strength (15.6 vs. 12.2 kg (SD 2.3)); at post-intervention this subject’s side-lying strength measure remained greater than one SD relative to the EC group mean (14.8 vs. 12.2 kg (SD 2.7)), though all other measures were within one SD of the group mean. In consultation with the physiotherapist who conducted all baseline and post-intervention it was determined that there was no reason to exclude these data from the analysis. Among the 15 subjects that completed both intervention treatments, two had a TUG time that exceeded two SDs of their respective sequence group mean, and one each had a 2MW walk distance, sitting strength or side-lying strength measure that exceeded two SDs of the respective group means. At post intervention one subject each had a TUG time, side-lying or supine strength measure that exceeded two SDs of the respective group means. No outliers were consistently associated with any particular subjects. Once again, in consultation with the physiotherapist, it was determined that there was no reason to exclude these data from the analysis as all tests were carried out in accordance with testing instructions.
A target wash-out period of 8 weeks between study periods (actual mean 7.4 weeks (SD 1.16)) was utilized to eliminate carry-over effects from period 1 to period 2. The lack of significant period effects associated with baseline (p > 0.14 for all) or post-intervention measures (p > 0.24 for all) suggests that the wash-out period was sufficient to preclude contamination of period 2 baseline measures by gains achieved during period 1. This is particularly relevant for the EC group where the gains accrued during the experimental treatment during period 1 may have improved control baseline measures at the beginning of period 2.
The baseline and post-intervention measures for experimental and control treatments are provided in Table II. The results of the cross-over ANOVA indicated few between-treatment differences at baseline. The only exception was supine hip abductor strength at the start of the experimental treatment (10.1 kg (SD 3.1) vs 9.1 kg (SD 2.0), p < 0.05).
|
Table II. Results for baseline and post-intervention primary and secondary outcome measures for experimental and control treatment phases |
|||||||
|
Baseline |
Post-intervention |
||||||
|
Control Mean (SD) |
Experimental Mean (SD) |
Effect size (d) |
Control Mean (SD) |
Experimental Mean (SD) |
Effect size (d) |
||
|
TUG, s |
30.0 (14.3) |
31.3 (13.4) |
0.100 |
29.6 (14.6) |
24.6 (11.4)** |
0.358 |
|
|
2MW, m |
57.1 (17.9) |
54.0 (15.9) |
0.182 |
56.8 (17.3) |
60.9 (18.2)* |
0.235 |
|
|
ABC |
52.8 (20.9) |
53.2 (21.0) |
0.018 |
52.8 (21.3) |
59.2 (17.9)** |
0.324 |
|
|
Houghton |
5.7 (2.7) |
5.7 (2.8) |
0.000 |
5.9 (2.8) |
5.8 (2.8) |
0.021 |
|
|
Strength, kg |
|||||||
|
Sitting |
10.3 (2.3) |
10.4 (2.8) |
0.077 |
10.3 (2.7) |
11.4 (2.9)* |
0.382 |
|
|
Side-lying |
10.9 (3.8) |
11.5 (4.0) |
0.144 |
10.9 (3.2) |
12.2 (2.5) |
0.436 |
|
|
Supine |
9.1 (2.0) |
10.1 (3.1)** |
0.394 |
9.8 (2.3) |
10.0 (2.4) |
0.114 |
|
|
Girth, cm |
48.3 (6.5) |
47.9 (5.9) |
0.071 |
48.5 (6.2) |
48.1 (6.2) |
0.066 |
|
|
*p < 0.05; **p < 0.01. TUG: Timed Up & Go; 2MW: Two-Minute Walk; ABC: Activities Specific Balance Confidence Scale; Houghton: Houghton Scale of Prosthetic Use. |
|||||||
Analysis of post-treatment data indicated a number of significant improvements associated with hip abductor training relative to arm ergometry. Hip abductor training resulted in 17% faster TUG time (24.6 s (SD 11.4) vs. 29.6 s (SD 14.6), p < 0.01), 7% greater 2MW distance (60.9 m (SD 18.2) vs. 56.8 m (SD 17.3), p < 0.05), 12% greater balance (59.2 (SD 17.9) vs. 52.8 (SD 21.3), p < 0.01), and 11% greater sitting strength (11.4 kg (SD 2.9) vs. 10.3 kg (SD 2.7), p < 0.05). There were no differences detected for side-lying strength (12.4 kg (SD 2.4) vs. 10.6 kg (SD 3.2), p = 0.06), supine strength (p = 0.71), prosthetic use (p = 0.45), nor thigh girth (p = 0.42). The cross-over ANOVA also indicated no significant sequence or period effects for any of the outcome measures, indicating that the outcome measures were affected by neither group assignment (EC vs. CE) nor the ordering of treatment within each group.
Utilizing published data (16), it was determined that an improvement of 5.7 s on the TUG met the MDD90 threshold. While only two subjects achieved an improvement of at least 5.7 s during the arm ergometry treatment, more than half (9/16) were able to demonstrated improvements greater than 5.7 s during the hip abductor treatment.
DISCUSSION
The outcome of this study resulted in the partial rejection of the null hypotheses that there would be no treatment effect on either the primary or secondary outcome measures. The results demonstrate that a twice weekly program of hip abductor strength training is effective in improving TUG and 2MW performance, balance confidence and abductor strength. In addition, this 8-week program was well tolerated by all subjects as indicted by the excellent compliance of nearly all study subjects.
Interventions targeted at improving functional performance are important for TFAs as they tend to ambulate less frequently than transtibial amputees (TTA) (24); demonstrate limited endurance (25, 26); report a higher incidence of community falls than TTAs (27, 28) and, as a result of greater bone density loss compared to both able-bodied adults and patients with TTAs (29), are likely at a higher risk of hip fracture. The results of the current study suggest that hip abductor strength training may, through improvement in functional performance, mitigate these factors.
Functional outcome measures
Outcomes commonly utilized in the rehabilitation of patients with amputation were used in this study. Published values for the TUG for TFAs vary widely and are often difficult to discriminate as data are often aggregated for TFAs and TTAs (18, 30). A study evaluating the reliability and validity of the TUG for patients with lower limb amputation, which found TUG score of 28.3 s (SD 12.2) for TFAs (16), is comparable to the range of TUG scores found in the current study, which ranged from 31.9 s (SD 13.6) at baseline to 24.3 s (SD 11.6). In a study comparing two different mechanical knees and the patients’ original knee, the reported TUG time with the original knee was 10.4 s (SD 3.7) for a group of TFAs (31). While quite different from the results of the current study, the differences may be ascribed to the characteristics of that group which tended to be younger (67.8 years (SD 5.2) vs. 58.8 years (SD 11.9)) and had experienced their amputation much earlier (7.3 years (SD 8.2) vs. 31.8 years (SD 17.3)); in addition, inclusion criteria included 6–8 h daily prosthetic use and ability to walk for a distance of 1 km. Nonetheless, as the TUG has been established as a measure of functional walking speed related to physical mobility (16), a 17% improvement in TUG time clearly suggests the effectiveness of hip abductor strength training. Only 2/16 subjects were able to achieve improvements in TUG score exceeding the 5.7s MDD90 score as a result of arm ergometry, while 9/16 subjects exceeded 5.7s as a result of hip abductor strength training.
2MW times are also often not reported in a manner allowing discrimination between TFAs and TTAs (32, 33). In the current study mean 2MW times at the beginning of both intervention treatments, as well as the mean 2MW time at the completion of the control treatment, were comparable to a previously published report of TFAs when using a locked-knee prosthesis (34). Given that the 2MW test has been shown to be related to ambulation performance in the community (32), an improvement of 7% in 2MW performance is notable.
The significant improvement in perception of balance confidence is a welcome result of this program, given the study group tended to report much lower balance confidence relative to non-vascular patients with amputation (35) and indeed has been identified as a variable that should be closely considered by clinicians as it relates to functional performance (36). Though balance confidence at discharge from prosthetic rehabilitation has been shown to be predictive of social activity, it tends not to change over time, in spite of improvement in walking ability (37). In the current study, the significant improvement in balance confidence may have resulted from the fact that subjects were able to observe progressive improvement in strength gains over time. This suggests that the observed improvement in strength translated to a perceived improvement in balance, whereas in previous studies an improvement in function (i.e., walking ability) was not readily evident to the subject, thus balance confidence remained unchanged.
Strength measures
Hip abductor strength improved while seated or side-lying, but not while lying supine. Given that baseline supine strength was significantly different, it is unclear why this difference failed to remain at post-intervention, particularly as post-intervention sitting and side-lying strength differed significantly. This apparent incongruence may reflect inherent differences in testing manoeuvres. Seated and side-lying abduction may allow more force generation to be directed toward the hand-held dynamometer, while supine abduction may result in force being directed both as an abduction force toward the dynamometer and an extension force toward the bed, thus dissipating abduction force. Alternatively, this observation may be partially explained by the fact that strength training was conducted in the seated position. Further examination of the reliability and validity of hand-held dynamometer for assessing hip abduction force generation among patients with TFA may be warranted.
The observed increased in hip abductor strength is largely consistent with Nolan (14) who found that a 10-week home-based training program consisting of twice weekly balance, co-ordination and hip flexion/extension exercises resulted in significant increases in hip flexor/extensor strength in the residual and intact limbs, while hip strength measures remained largely unchanged among the control group. However, where Nolan was largely focused on improvements in muscular strength and restoration of running ability, the current study focused primarily on functional outcomes commonly used in the rehabilitation setting and suggestive of improved community ambulation. In addition, where Nolan utilized relatively young patients with amputation due to trauma, tumour or congenital problems, the patients included in the current study were a mean of 26.7 years older with a history of diabetes and/or peripheral vascular disease.
In spite of the exercise-related improvements in abductor strength, the values obtained at the completion of the experimental treatment in the current study remain well below reference values for able-bodied male (26.7 kg, non-dominant; 26.4 kg, dominant) and female adults aged 60–69 years (16.8 kg, non-dominant; 17.6 kg, dominant), as measured in the supine position (38). In addition, the relatively short duration of the intervention treatment and the absence of significant differences in girth measures suggest that the observed improvement in hip abductor strength likely resulted from neurological adaptation to the strength training as opposed to muscle hypertrophy (39). Given the gap that remains between strength measures seen in the current study and age-matched reference values as well as the absence for significant muscle hypertrophy, it is possible that continued exercise training would allow additional strength gains to be achieved. Though not previously demonstrated experimentally among patients with TFA, strength training of patients with TTA has been shown to result in substantial structural adaptation of the thigh muscles in terms of girth, fibre typing, as well as improvements in walking distance (40). An intervention of sufficient duration to stimulate muscle hypertrophy may allow for even greater improvements in both muscular structure and physical function.
Study limitations
Given that study subjects were reimbursed for travel to attend exercise and testing sessions, and received a modest prorated honorarium to promote compliance, we are unable to say definitively whether the same results would be achieved in a less formal training regimen. Alternatively, we are unable to rule-out whether those who opted to participate represented a particularly high functioning, relatively young group with fewer comorbidities, the latter of which may impact the ability to engage in an exercise program for an extended period of time. As a consequence, those who opted to participate may represent a highly motivated subgroup of patients, thus limiting generalizability. Further, we are unable to determine the sustainability of strength and function gains beyond the completion of the formal experimental intervention. Finally, the interpretation of the results of this study would have been strengthened by further use of the MDD90 scores for selected outcomes, though calculation of MDD is limited by the fact that TFA data is not routinely reported separately from TTA data.
Conclusion
The results of this study provide evidence of the efficacy of twice weekly hip abductor strength training for improving TUG and balance confidence among older patients with TFA. A relatively simple intervention such as the one described in this study offers a number of advantages, as this intervention requires equipment that is commonly available in community health and fitness centres, requires little expertise to use properly, and can be inexpensively and easily modified by simply elongating the knee/thigh pads proximally toward the hip. In addition, compliance with the exercise protocol may suggest favourable long-term compliance. Further examination is required to determine whether the gains observed in the current study can be replicated with less specialized equipment (e.g., Thera-Bands® Exercise Bands), thus offering an effective training program for utilization independently in ones’ own home, and whether such gains translate to other outcomes (e.g., social participation).
ACKNOWLEDGEMENTS
This project was funded by a research grant provided by the Canadian Diabetes Association. The authors wish to acknowledge the contributions of Ruby Paner in conducting the exercise training sessions.
REFERENCES
