Yeo Hyung Kim, MD1, Sung Jin Jung, MD1, Eun Joo Yang, MD, PhD1 and Nam Jong Paik, MD, PhD1,2
From the 1Department of Rehabilitation Medicine, Seoul National University Bundang Hospital, Seongnam and 2Department of Rehabilitation Medicine, Seoul National University College of Medicine, Seoul, Republic of Korea
OBJECTIVE: To identify baseline risk factors associated with hemiplegic shoulder pain during the first 6 months after a stroke and to investigate changes in these risk factors over time.
DESIGN: Longitudinal observational study.
Patients: A total of 94 patients with first-ever unilateral stroke lesion within 1 month after stroke.
METHODS: Clinical, radiological and sonographic evaluations were performed at baseline. Hemiplegic shoulder pain was assessed at 1, 3 and 6 months post-stroke. Associations between baseline factors and hemiplegic shoulder pain during the first 6 months and hemiplegic shoulder pain at 1, 3 and 6 months poststroke were analysed.
RESULTS: Poor arm motor function, indicated by a poor National Institutes of Health Stroke Scale item 5 score (odds ratio (OR) = 3.0; 95% confidence interval (CI) = 1.1–7.7) and the presence of supraspinatus tendon pathology (OR = 4.2; 95% CI = 1.4–12.9), were associated with hemiplegic shoulder pain. While patients with adhesive capsulitis, glenohumeral subluxation, or long head of biceps tendon effusion showed a higher prevalence of hemiplegic shoulder pain at 1 month after stroke, those with supraspinatus tendon pathology showed a higher prevalence at 3 and 6 months.
CONCLUSION: Patients at high risk of hemiplegic shoulder pain with severe arm paralysis and supraspinatus tendon pathology require more careful attention during the rehabilitation period.
Key words: stroke; shoulder pain; ultrasonography.
J Rehabil Med 2013; 45: 00–00
Correspondence address: Nam-Jong Paik, Department of Rehabilitation Medicine, Seoul National University College of Medicine, Seoul National University Bundang Hospital, 166 Gumi-ro, Bundang-gu, Seongnam-si, Gyeonggi-do, 463-707, South Korea. E-mail: njpaik@snu.ac.kr
Accepted Jul 3, 2013; Epub ahead of print Oct 15, 2013
INTRODUCTION
Hemiplegic shoulder pain (HSP), a general term for shoulder pain on the hemiplegic side after stroke, is a common complication that can cause poor functional recovery, prolongation of hospitalization, and reduced quality of life in stroke patients (1, 2). A recent review article on HSP revealed that the prevalence of HSP is approximately 22–23% in the general population of stroke survivors and approximately 54–55% among stroke patients in rehabilitation hospital settings (3). The pathogenesis of HSP is mostly unknown and is considered to be multifactorial.
Many previous studies have investigated potential factors associated with HSP, such as loss of motor function (4–6), sensory abnormalities (5, 7), adhesive capsulitis (5, 8–10), rotator cuff disorders (8, 9, 11–13), shoulder spasticity (5, 14), shoulder subluxation (4, 9), impaired activities of daily living (4), age (15), left hemiplegia (16) and diabetes mellitus (5, 17). Nevertheless, the supposed associations between HSP and many of these factors remain controversial across studies. Although some prospective studies have identified a few consistent risk factors for HSP, most evaluated crosssectional correlations only, without considering temporal course and confounding issues (6, 8, 9, 11–13). The inconsistent associations of possible predictors across studies may also result from variable HSP definitions, variable inclusion criteria for patients, inconsistent methodologies used for assessing risk factors, and limited sample sizes.
The present study, which was of longitudinal-observational design, was conducted to determine baseline risk factors for the occurrence of subsequent HSP during the rehabilitation period. The correlations of potential factors with HSP during the first 6 months after stroke were analysed to identify individual risk factors. A multivariate logistic regression model for HSP was constructed to determine independent risk factors after adjustment for possible confounders. In addition, correlations between potential factors and HSP at 1, 3 and 6 months post-stroke were investigated to identify changes to the risk factors according to time after a stroke.
METHODS
In total, 428 consecutive stroke patients admitted to the rehabilitation unit of Seoul National University Bundang Hospital were screened for participation between July 2009 and May 2011. The study protocol was approved by the Institutional Review Board of Seoul National University Bundang Hospital. Acute stroke patients with stroke onset within 1 month, whose diagnosis was confirmed by magnetic resonance imaging were included. Exclusion criteria were a history of shoulder pain or shoulder surgery before stroke onset, recurring or bilateral stroke, severe cognitive impairment, and an unstable medical condition.
Baseline (T0) demographic, clinical, radiological, and sonographic evaluations were performed on the rehabilitation unit within 1 month from stroke onset. The patients were also interviewed regarding their HSP at 1 (T0), 3 (T1) and 6 months (T2) after the stroke. The interviews at T1 and T2 were performed by a single researcher blinded to the patient characteristics in the outpatient clinic of the rehabilitation department. During the hospitalization period, all of the participants underwent a standard in-patient rehabilitation programme including range-of-motion exercises, strengthening exercises, gait training, balance training, and hand function training, according to their neurological deficit and tolerance. Patients who needed further rehabilitation after discharge from our tertiary hospital-based rehabilitation unit were transferred to a specialized rehabilitation hospital in the community. For the relief of HSP, physical therapy modalities, such as hot pack and ultrasound, were used first, and pain medication and/or intra-articular corticosteroid injection were given for persistent or intolerable pain.
Evaluation of baseline factors
Baseline variables collected at T0 included demographic, clinical, radiological and sonographic factors. Age, gender, lesion side, type of stroke, pre-stroke comorbidities, National Institutes of Health Stroke Scale (NIHSS) score and modified Barthel Index were recorded. The hospitalization period was recorded after the discharge of participants. The level of motor function was assessed by multiple methods, including Brunnstrom motor recovery stage (B-stage) of the arm and hand (18), Fugl-Meyer (FM) arm score (18), NIHSS item 5 (motor arm) score (19) and motor evoked potential. The NIHSS item 5 score for each arm was evaluated on a 4-point scale, in which 0 indicated normal motor function, and 4 indicated complete paralysis of the arm. Motor-evoked potential signals were recorded in the abductor pollicis brevis using a standard protocol (20), and displayed on a conventional electromyographic system (Medelec Ltd., Surrey, UK). Sensation to light touch was evaluated at the volar surface of the fingertip and the lateral epicondyle of the humerus, and compared with the non-hemiplegic side. Passive shoulder range of motion was measured with a goniometer for forward flexion, abduction, and external rotation. Subjects with a reduction in passive range of motion in at least 2 directions of the hemiplegic shoulder of > 30º, compared with the contralateral side, were considered to have adhesive capsulitis (21). The presence of shoulder spasticity was defined as a Modified Ashworth Scale score of 1 or greater in the shoulder flexor muscles (5, 6).
Bilateral shoulder X-rays of anterior-to-posterior and lateral projections were obtained to determine shoulder subluxation and other findings, such as acromioclavicular arthropathy, subacromial spur, and calcification around the shoulder joint. Shoulder subluxation was measured according to the method of Brooke et al. (22). Briefly, the presence of shoulder subluxation was determined by comparing the bilateral vertical distances between the inferior acromial point and the central point of the humeral head, measured on the shoulder X-ray.
A single physician, with 11 years of experience in musculoskeletal sonography, blinded to the study design and patient characteristics, performed shoulder sonography using a 5–13-MHz linear-array transducer (Accuvix V20; Samsung Medison, Seoul, Korea). Typical sonographic scanning techniques were used, as described previously (23, 24). The long head of the biceps tendon, supraspinatus tendon, subscapularis tendon and infraspinatus tendon were examined in both the longitudinal and transverse planes. An anechoic area around the long head of the biceps tendon was interpreted as effusion in the sheath of the biceps tendon. Tendinosis of the rotator cuff was determined by hypoechoic and swelling changes with a difference in tendon thickness, compared with the contralateral side. Tear of the rotator cuff was defined as a hypoechoic or an anechoic cleft within the tendon in both the longitudinal and transverse planes. The subacromial-subdeltoid bursa, acromioclavicular joint degeneration, and glenohumeral joint degeneration were also examined. Anechoic fluid accumulation in the subacromial-subdeltoid bursa was interpreted as bursa effusion.
Evaluation of shoulder pain
HSP was considered when a patient reported shoulder pain confined to the shoulder of the hemiplegic side in the resting state or during passive range-of-motion exercise (6). The severity of HSP was measured using a 10-point numeric rating scale (NRS), in which a score of 10 indicated the worst pain possible and a score of 0 indicated no pain. Patients were asked to describe their worst self-perceived shoulder pain during the past 48 h with the NRS. NRS score 0 was defined as no pain, 1–3 as mild pain, and 4–10 as moderate to severe pain (4, 25). Because a previous prospective study (4) documented that most stroke patients with HSP reported moderate-to-severe pain (NRS 4–10), patients complaining of moderate-to-severe shoulder pain on the hemiplegic side were defined as having HSP. To determine baseline predictors for the development of HSP during the first 6 months after stroke, patients who reported HSP at any point during the follow-up period were allocated to the HSP group (n = 51). The control group (n = 43) consisted of the remaining participants who did not experience HSP during the follow-up period.
Statistical analysis
We estimated that a minimum sample size of 93 was needed for the 5 independent variables in the multivariate logistic regression model using the method described by Peduzzi et al. (26). The proportion of HSP was assumed to be 54%, according to previous large rehabilitation hospital-based studies (3). For participants who dropped out during the follow-up period, the last observation carried forward method was used. The significance level for all hypothesis testing was set at p < 0.05. SPSS software (ver. 18.0) was used for statistical calculations.
Statistical significance for the demographic, clinical, radiological and sonographic differences between the HSP and control groups were assessed using an independent t-test for continuous variables and Pearson’s χ2 test or Fisher’s exact test for categorical variables, as appropriate. Continuous and ordinal clinical variables were dichotomized before analysis. Age was categorized as < 70 and ≥ 70 years, according to the median age of the participants. Poor motor function was defined in each evaluation measure, stage I, II or III for B-stage (6), a score of 20 or less for the FM arm score (27), and a score of 3 or 4 for NIHSS item 5 score. Severely impaired activities of daily living was defined as a modified Barthel index score < 50 (28).
To detect multicollinearity, Spearman’s rho correlation between each variable was tested before the multivariate analysis. Age, gender and significant variables from the univariate analysis were included in the final multivariate logistic regression model. The Hosmer-Lemeshow statistic was used to determine goodness of fit. To identify factors associated with HSP at each stage after stroke (T0, T1 and T2), the patients with HSP and the rest of the patients without HSP were compared with Pearson’s χ2 test or Fisher’s exact test, as appropriate.
RESULTS
In total, 94 patients who signed informed consent and completed the baseline evaluation were included in the current study. The patient flowchart is shown in Fig. 1. HSP was newly developed at all 3 time-points (T0, T1 and T2) in patients who did not experience shoulder pain before the onset of stroke (Table I). The cumulative incidence of HSP during 6 months after stroke onset was 54.3%, constituting the HSP group. The baseline demographic characteristics of the HSP and control groups were similar (Table II). Reflex sympathetic dystrophy occurred in 8 patients, and hypothyroidism occurred in one patient during the follow-up periods.
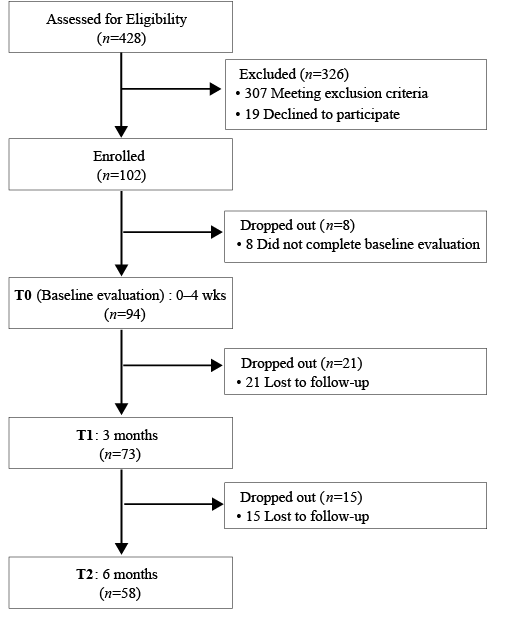
Fig. 1. Patient inclusion and follow-up.
|
Table I. Incidence of hemiplegic shoulder pain during the follow-up period |
|||
|
Days after stroke Mean (SD) |
HSP incidence n (%) |
HSP cumulative incidence n (%) |
|
|
T0 |
19.03 (8.14) |
30 (31.9) |
30 (31.9) |
|
T1 |
88.27 (28.92) |
11 (22.4) |
41 (43.6) |
|
T2 |
191.59 (37.04) |
10 (31.3) |
51 (54.3) |
|
HSP: hemiplegic shoulder pain; SD: standard deviation; T0: 1 month after stroke; T1: 3 months after stroke; T2: 6 months after stroke. |
|||
|
Table II. Demographics of the hemiplegic shoulder pain and control groups |
|||
|
HSP group (n = 51) |
Control group (n = 43) |
p-value |
|
|
Age, years, mean (SD) |
65.63 (10.95) |
65.49 (14.79) |
0.959 |
|
Males, n (%) |
24 (47.06) |
25 (58.14) |
0.284 |
|
Stroke lesion, n (%) |
|||
|
Right hemispheric |
21 (41.18) |
22 (51.16) |
0.333 |
|
Ischaemic |
41 (80.39) |
33 (76.74) |
0.667 |
|
Supratentorial |
43 (84.31) |
35 (81.40) |
0.708 |
|
Comorbidities, n (%) |
|||
|
Hypertension |
28 (54.90) |
25 (58.14) |
0.753 |
|
Diabetes mellitus |
14 (27.45) |
12 (27.91) |
0.961 |
|
Cardiovascular disease |
12 (23.53) |
9 (20.93) |
0.763 |
|
Malignancy |
3 (5.88) |
5 (11.63) |
0.463 |
|
Hospitalization, days, mean (SD) |
33.51 (13.94) |
32.16 (20.04) |
0.703 |
|
HSP group: hemiplegic shoulder pain group; those who reported shoulder pain during the first 6 months after a stroke; SD: standard deviation. |
|||
There were no significant differences in the baseline demographic, clinical, radiological and sonographic factors between follow-through and drop-out subjects, except age and modified Barthel Index score. The drop-out subjects involved older individuals (p = 0.007) with lower modified Barthel Index score (p = 0.005) compared with follow-through subjects.
In the HSP group, HSP occurred on the dominant side shoulder in 29 out of 51 subjects (56.9%). There were no significant differences in baseline demographic, clinical, radiological and sonographic factors between the subjects with HSP on the dominant side and those with HSP on the non-dominant side.
Risk factors for hemiplegic shoulder pain during the first 6 months after a stroke
Table III shows the associations between clinical, radiological and sonographic variables and HSP during the 6-month follow-up period in univariate analyses. Among the 5 variables assessed for loss of arm motor function, a poor FM arm score (OR = 2.6; 95% CI = 1.1–6.2; p = 0.024) and poor NIHSS item 5 score (OR = 2.9; 95% CI = 1.2–6.9; p = 0.014) were associated significantly with HSP during the first 6 months after a stroke. No association was noted between HSP and severely impaired ADL, decreased light touch of arm, adhesive capsulitis, shoulder spasticity, shoulder subluxation, or other radiological findings. Significant associations with HSP were also demonstrated in long head of biceps tendon effusion (OR = 2.7; 95% CI = 1.1–6.4; p = 0.023) and supraspinatus tendon tendinosis/tear (OR = 3.1; 95% CI = 1.3–7.5; p = 0.010).
|
Table III. Factors associated with hemiplegic shoulder pain during the first 6 months after a stroke |
||||
|
HSP group (n = 51) n |
Control group (n = 43) n |
OR (95% CI) |
p-value |
|
|
Clinical factors |
|
|
|
|
|
Loss of motor function |
||||
|
Poor B-stage, arm |
30 |
18 |
1.984 (0.871–4.520) |
0.101 |
|
Poor B-stage, hand |
34 |
21 |
2.095 (0.909–4.827) |
0.080 |
|
Poor FM arm score |
29 |
14 |
2.636 (1.129–6.154) |
0.024 |
|
Poor NIHSS item 5 score |
27 |
12 |
2.906 (1.225–6.895) |
0.014 |
|
No response of MEP |
30 |
21 |
1.905 (0.749–4.844) |
0.174 |
|
Severely impaired ADL |
30 |
26 |
0.934 (0.408–2.137) |
0.872 |
|
Decreased light touch of arm |
26 |
20 |
1.196 (0.531–2.696) |
0.666 |
|
Adhesive capsulitis |
28 |
19 |
1.538 (0.680–3.479) |
0.301 |
|
Shoulder spasticity |
11 |
4 |
2.681 (0.787–9.140) |
0.106 |
|
Radiological factors |
|
|
|
|
|
Glenohumeral subluxation |
18 |
10 |
1.740 (0.689–4.394) |
0.239 |
|
Acromiclavicular arthropathy |
5 |
5 |
0.791 (0.212–2.956) |
0.748 |
|
Subacromial spur |
7 |
7 |
0.780 (0.248–2.453) |
0.671 |
|
Calcification |
4 |
2 |
1.682 (0.291–9.705) |
0.687 |
|
Sonographic factors |
|
|
|
|
|
Long head of biceps tendon effusion |
26 |
12 |
2.687 (1.133–6.371) |
0.023 |
|
Supraspinatus tendon tendinosis/tear |
39 |
22 |
3.102 (1.285–7.487) |
0.010 |
|
Subscapularis tendon tendinosis/tear |
14 |
6 |
2.333 (0.809–6.731) |
0.111 |
|
Infraspinatus tendon tendinosis/tear |
11 |
8 |
1.203 (0.435–3.328) |
0.721 |
|
Subacromial-subdeltoid bursa effusion |
27 |
24 |
0.891 (0.394–2.013) |
0.781 |
|
Acromioclavicular degeneration |
16 |
14 |
0.947 (0.397–2.260) |
0.902 |
|
Glenohumeral degeneration |
7 |
5 |
1.209 (0.354–4.124) |
0.761 |
|
HSP group: hemiplegic shoulder pain group, those who complained of shoulder pain during the first 6 months after a stroke; B-stage: Brunnstrom motor recovery stage; FM: Fugl-Meyer; NIHSS: National Institutes of Health Stroke Scale; MEP: motor evoked potential; ADL: activities of daily living; OR: odds ratio; CI: confidence interval. |
||||
The logistic regression model for HSP during the first 6 months after stroke, derived from age, gender, and significant variables from the univariate analysis, is shown in Table IV. Because the correlation between the NIHSS item 5 score and FM arm score was significant (Spearman ρ = –0.870; p < 0.001), only the NIHSS item 5 score was included in the multivariate model. The fit of this model to the data was good, according to the Hosmer-Lemeshow test (p = 0.804). The model constructed revealed that age < 70 years (OR = 3.6; 95% CI = 1.3–10.6; p = 0.018), poor arm motor function, as indicated by a poor NIHSS item 5 score (OR = 3.0; 95% CI = 1.1–7.7; p = 0.026), and the presence of supraspinatus tendon tendinosis/tear (OR = 4.2; 95% CI = 1.4–12.9; p = 0.012) were associated with HSP during the first 6 months after a stroke.
|
Table IV. Multivariate logistic regression model of hemiplegic shoulder pain during the first 6 months after a stroke |
||
|
OR (95% CI) |
p-value |
|
|
Young age (< 70 years) |
3.647 (1.250–10.637) |
0.018 |
|
Male |
0.996 (0.370–2.683) |
0.994 |
|
Poor NIHSS item 5 score (≥ 3) |
2.957 (1.141–7.665) |
0.026 |
|
Presence of long head of biceps tendon effusion |
2.349 (0.897–6.150) |
0.082 |
|
Presence of supraspinatus tendon tendinosis/tear |
4.212 (1.372–12.931) |
0.012 |
|
NIHSS: National Institutes of Health Stroke Scale; OR: odds ratio; CI: confidence interval. |
||
Risk factors for hemiplegic shoulder pain at 1, 3 and 6 months after stroke
As shown in Table V, the baseline risk factors associated with HSP at each evaluation time-point (T0, T1 and T2) differed. Patients with poor NIHSS showed a higher prevalence of HSP at T0 (OR = 2.5; 95% CI = 1.0–6.1; p = 0.041), at T1 (OR = 3.1; 95% CI = 1.3–7.4; p = 0.010), and at T2 (OR = 3.7; 95% CI = 1.5–8.7; p = 0.003). Patients with poor B-stage of the arm or hand or a poor FM arm score showed a higher prevalence of HSP at T1 and T2 (poor B-stage of arm, OR = 2.9; 95% CI = 1.2–7.1 at T1, OR = 2.9; 95% CI = 1.2–6.7 at T2, poor B-stage of hand, OR = 2.8; 95% CI = 1.1–7.0 at T1, OR = 3.5; 95% CI = 1.5–8.5 at T2, poor FM arm score, OR = 2.7; 95% CI = 1.1–6.5 at T1, OR = 3.6; 95% CI = 1.5–8.4 at T2, respectively). Patients with no response of MEP or glenohumeral subluxation showed a higher prevalence of HSP at T0 and T1, respectively (no response of MEP, OR = 4.2; 95% CI = 1.3–13.9 at T0, OR = 4.1; 95% CI = 1.3–12.4 at T1; glenohumeral subluxation, OR = 3.5; 95% CI = 1.4–9.3 at T0, OR = 2.6; 95% CI = 1.0–6.6 at T1). Patients with adhesive capsulitis (OR = 2.7; 95% CI = 1.1–6.8) or long head of biceps tendon effusion (OR = 2.7; 95% CI = 1.1–6.5) showed a higher prevalence of HSP at T0 compared with those without adhesive capsulitis or long head of biceps tendon effusion. Patients with supraspinatus tendinosis/tear showed a higher prevalence of HSP at T1 and T2 compared with those without a supraspinatus tendinosis/tear (OR=3.0; 95% CI = 1.1–7.8 at T1 and OR = 2.7; 95% CI = 1.1–6.6 at T2).
|
Table V. Factors associated with hemiplegic shoulder pain at T0, T1 and T2 |
|||||||||
|
T0 |
T1 |
T2 |
|||||||
|
OR (95% CI) |
p-value |
OR (95% CI) |
p-value |
OR (95% CI) |
p-value |
||||
|
Clinical factors |
|
|
|
|
|
|
|
|
|
|
Loss of motor function |
|||||||||
|
Poor B-stage, arm |
1.700 (0.705–4.099) |
0.235 |
2.927 (1.211–7.078) |
0.015 |
2.893 (1.246–6.717) |
0.012 |
|||
|
Poor B-stage, hand |
2.059 (0.819–5.179) |
0.122 |
2.778 (1.113–6.933) |
0.026 |
3.542 (1.470–8.534) |
0.004 |
|||
|
Poor FM arm score |
1.861 (0.772–4.483) |
0.164 |
2.717 (1.138–6.485) |
0.023 |
3.586 (1.521–8.454) |
0.003 |
|||
|
Poor NIHSS item 5 score |
2.497 (1.028–6.064) |
0.041 |
3.083 (1.287–7.381) |
0.010 |
3.671 (1.548–8.703) |
0.003 |
|||
|
No response of MEP |
4.200 (1.270–13.895) |
0.014 |
4.089 (1.344–12.438) |
0.010 |
2.196 (0.837–5.760) |
0.107 |
|||
|
Severely impaired ADL |
1.026 (0.424–2.486) |
0.954 |
1.402 (0.588–3.344) |
0.445 |
1.280 (0.558–2.937) |
0.560 |
|||
|
Decreased light touch of arm |
1.295 (0.543–3.089) |
0.559 |
1.548 (0.664–3.610) |
0.311 |
1.179 (0.523–2.655) |
0.692 |
|||
|
Adhesive capsulitis |
2.741 (1.107–6.787) |
0.027 |
1.746 (0.745–4.091) |
0.198 |
1.294 (0.574–2.918) |
0.535 |
|||
|
Shoulder spasticity |
2.130 (0.692–6.559) |
0.229 |
0.862 (0.268–2.769) |
0.803 |
2.788 (0.871–8.919) |
0.076 |
|||
|
Radiological factors |
|
|
|
|
|
|
|
|
|
|
Glenohumeral subluxation |
3.538 (1.351–9.271) |
0.008 |
2.628 (1.040–6.639) |
0.038 |
1.034 (0.421–2.543) |
0.941 |
|||
|
Acromiclavicular arthropathy |
0.946 (0.225–3.978) |
1.000 |
0.671 (0.161–2.800) |
0.736 |
1.026 (0.275–3.833) |
1.000 |
|||
|
Subacromial spur |
0.870 (0.247–3.067) |
1.000 |
1.278 (0.400–4.077) |
0.678 |
1.028 (0.327–3.226) |
0.963 |
|||
|
Calcification |
1.120 (0.192–6.521) |
1.000 |
0.306 (0.034–2.744) |
0.401 |
2.154 (0.373–12.425) |
0.434 |
|||
|
Sonographic factors |
|
|
|
|
|
|
|
|
|
|
Long head of biceps tendon effusion |
2.678 (1.099–6.526) |
0.028 |
2.250 (0.951–5.323) |
0.063 |
1.594 (0.695–3.656) |
0.270 |
|||
|
Supraspinatus tendon tendinosis/tear |
1.763 (0.680–4.569) |
0.241 |
2.950 (1.112–7.824) |
0.026 |
2.711 (1.105–6.648) |
0.027 |
|||
|
Subscapularis tendon tendinosis/tear |
1.194 (0.421–3.386) |
0.739 |
2.083 (0.764–5.678) |
0.147 |
2.724 (0.973–7.625) |
0.051 |
|||
|
Infraspinatus tendon tendinosis/tear |
0.981 (0.332–2.894) |
0.972 |
1.371 (0.491–3.829) |
0.547 |
1.414 (0.515–3.880) |
0.500 |
|||
|
Subacromial-subdeltoid bursa effusion |
0.947 (0.397–2.260) |
0.902 |
1.336 (0.571–3.127) |
0.503 |
0.795 (0.352–1.796) |
0.581 |
|||
|
Acromioclavicular degeneration |
1.100 (0.436–2.774) |
0.840 |
1.032 (0.419–2.541) |
0.945 |
1.056 (0.442–2.520) |
0.902 |
|||
|
Glenohumeral degeneration |
0.386 (0.079–1.883) |
0.326 |
0.548 (0.138–2.181) |
0.526 |
1.216 (0.362–4.088) |
0.751 |
|||
|
T0: 1 month after stroke; T1: 3 months after stroke; T2: 6 months after stroke; B-stage: Brunnstrom motor recovery stage; FM: Fugl-Meyer; NIHSS: National Institutes of Health Stroke Scale; MEP: motor evoked potential; ADL: activities of daily living; OR: odds ratio; CI: confidence interval. |
|||||||||
DISCUSSION
The aim of the present study was to identify baseline risk factors associated with HSP during the first 6 months after a stroke and to reveal longitudinal changes in baseline risk factors according to time after a stroke. To our knowledge, few longitudinal studies of HSP, which consider both clinical and sonographic risk factors together, have been reported. The primary objective of this study was achieved by demonstrating that poor arm motor function and supraspinatus tendon pathology were independent predictors of the development of HSP during the first 6 months after stroke. In addition, the associated baseline predictors for subsequent HSP differed according to the temporal course after a stroke. Thus, future studies are required to describe precisely the time after stroke and the onset of HSP.
A positive correlation between HSP and loss of motor function has been reported; stroke patients with severe paralysis report HSP more frequently during the rehabilitation period (4, 6, 15, 17). Because the motor assessment tools used in these studies were diverse, such as B-stage (6, 15), NIHSS item 5 (4), Uppsala University Hospital Motor Assessment Scale (4), and the Motricity Index (5), we evaluated arm motor function using 5 methods to assess the most suitable tool. The correlations between these motor evaluations were moderate to strong (Spearman ρ = 0.555–0.860), as expected.
A significant association with HSP during the first 6 months after a stroke was found with the NIHSS item 5 and FM arm scores. The poor NIHSS item 5 score was the only tool associated with HSP at all follow-up time-points (T0, T1 and T2). While MEP response was associated with HSP in the acute-to-subacute stage (T0 and T1), poor B-stage and poor FM arm score were risk factors for HSP in the subacute and chronic stages (T1 and T2). Although whether the loss of arm motor function is a direct cause of HSP remains unknown, in the present study we demonstrated that severe motor impairment was an independent risk factor for HSP. In addition, future researchers for HSP should choose the motor evaluation tool with caution in the study design, because each tool showed different association with HSP according to the temporal course after a stroke. NIHSS item 5 score might be a universal tool during the first 6 months after stroke.
The glenohumeral joint, the most movable joint in the human body, is stabilized by the musculature called dynamic stabilizers, including the rotator cuff muscles, the long head of the biceps tendon, and other shoulder girdle muscles. Thus, the severe paralysis of arm by a stroke also accompanies severe weakness in these dynamic stabilizers of shoulder, which may diminish the stability of the glenohumeral joint, altering the normal protective movement patterns of the glenohumeral and scapulothoracic joints. In addition, severe paralysis can lead to prolonged immobilization of the shoulder and dependence on transfer activities, resulting in more possibilities for repeated traction injuries during the rehabilitation process and daily care (29). These conditions may facilitate abnormal movement patterns and periarticular soft-tissue injuries in the shoulder (30), causing subsequent HSP.
Sonographic evaluation by an experienced operator is a convenient and reproducible diagnostic test for rotator cuff problems (31). The current study highlighted that supraspinatus tendon pathology (tendinosis/tear) was an independent predictor of HSP during the first 6 months after a stroke, after adjustment for age, gender, and poor motor function. The long head of biceps tendon effusion was a risk factor for HSP during the first 6 months after a stroke, but not an independent predictor of HSP after adjustment for age, gender and poor motor function. These results are consistent with previous sonographic studies of hemiplegic shoulders; i.e. the primary abnormalities in hemiplegic shoulders were long head of biceps tendon effusion and supraspinatus tendon pathology (6, 15, 32). While long head of biceps tendon effusion was significantly associated with HSP at the acute stage (T0), supraspinatus tendon tendinosis/tear was associated with HSP at the subacute and chronic stages (T1, T2) in the temporal course of the stroke.
Our results are in partial agreement with those of Pong et al. (6), who performed sonographic examinations in both acute- and chronic-stage stroke patients, suggesting that abnormal sonographic findings were correlated only with HSP at the chronic stage of stroke. Their different study design to ours, excluding frozen shoulder subjects and including mild HSP patients in the analysis, might have caused the different results in terms of the correlation between HSP and sonographic abnormalities at the acute stage. Because Pong et al. (6) did not analyse the correlation between sonographic abnormalities at the acute stage and HSP in chronic stage after stroke, no conclusion as to risk factors could be drawn.
Multiple factors are thought to contribute to rotator cuff tears, including anatomical variables, acromial spurs, ageing, tensile overload and trauma (33). Among these, stroke patients are more susceptible to repeated micro/macro-trauma, due to immobility and dependent daily living activities. A sonographic study reported that patients with poor arm motor function were more prone to soft-tissue injury of the shoulder during rehabilitation, and demonstrated increased sonographic abnormalities in more severely paralysed patients (6). Another study reported that the prevalence of HSP increased in the first weeks after discharge from hospital (29). Thus, avoidance of unnecessary stretching or traction of the hemiplegic upper extremity is important to prevent HSP, especially in severely paralysed patients. Because sonographic evaluation was not performed before stroke onset, however, the time at which the rotator cuff problem occurred was unclear in the current study. Therefore, a cohort study with regular follow-up and sonographic evaluations of the bilateral shoulders is necessary to reveal the temporal course of hemiplegic shoulder pathology.
Adhesive capsulitis has been found to be common in stroke patients (8–10, 25). In the current study, 50% of participants showed a shoulder range of motion limitation in multiple directions at the acute stage of stroke (T0). Consistent with a previous cross-sectional study in acute stroke patients (8), a significant correlation between adhesive capsulitis and HSP was observed only in the acute stage. However, adhesive capsulitis did not correlate with either HSP during the first 6 months after stroke or HSP in the subacute to chronic stage after stroke (T1, T2). Thus, adhesive capsulitis may contribute only to immediate shoulder pain and not to persistent shoulder pain or that which develops in the future. Because a cross-sectional correlation was demonstrated, exercises to maintain shoulder range of motion, especially during the acute stage of stroke, are advocated during rehabilitation.
The relationship between glenohumeral subluxation and HSP remains controversial (4, 8, 15, 16, 25, 34, 35). One cohort multicentre study concluded that shoulder subluxation and time after stroke onset were risk factors for HSP, evaluated during a rehabilitation programme in which the mean onset-to-admission interval was 84.3–174.6 days (34). We also found that glenohumeral subluxation was significantly associated with HSP at 1 and 3 months after a stroke, but not with HSP during the first 6 months after a stroke. This inconsistent duration from stroke onset to HSP onset might be responsible for the several reports of no association between subluxation and HSP (8, 9).
A few studies have suggested that sensory impairment was associated with HSP (4, 7, 34, 36). While some (7, 34) found an association between decreased proprioception and HSP, 1 study (4) revealed that sensory disturbance for light touch was associated with HSP. A population-based case-cohort study assessed sensory impairment by interview as the presence of a loss of feeling that lasted more than 24 h (36). On the other hand, in the present study, we demonstrated no relationship between decreased light touch of the arm and HSP. These studies of sensory impairment have important limitations, however, mostly stemming from the vague definition of sensory impairment and their inconsistent measurement methods.
Controversy regarding the association between spasticity and HSP continues (6, 8, 15). A possible relationship between the spasticity of shoulder girdle muscles and HSP was proposed from reports of improvement in HSP after motor point block or botulinum toxin A injections into shoulder girdle muscles, especially the subscapularis (37–39). In contrast, a recent systematic review of interventions for HSP showed that HSP improved independently of spasticity (40). In the current study, shoulder spasticity was not related to HSP, but a borderline significant association between spasticity and HSP at the chronic stage was identified (T2). Treatment to reduce shoulder spasticity and pain might thus be more effective in HSP patients at the chronic stage.
Controversy exists regarding the demographic risk factors associated with HSP development. In the present study, the baseline demographics, including age, gender, stroke lesion and comorbidities, were not different between the HSP and control groups. After adjusting for arm motor function and sonographic shoulder pathology, younger age was an independent risk factor for HSP during the first 6 months after a stroke. It appears that a younger individual with an identical arm motor function and shoulder pathology as an older patient may be more active and thus more prone to soft tissue injuries of the shoulder.
The present study has certain limitations. Only 5 predictors could be included in the final multivariate model due to the small sample size. Moreover, dichotomization of continuous and ordinal variables decreased the power of these predictors in the analysis and interpretation. Furthermore, the fact that the last observation carried forward method was used for 22% (T1) and 38% (T2) of subjects lost to follow up might have a significant impact on the T1 and T2 findings, respectively. Appropriate treatments were given whenever each patient needed pain reduction during follow-up period. However, we did not classify the study participants according to the treatments for the simplification of the analysis. Because we excluded a large group of patients who were unable to describe their pain with NRS due to severe cognitive impairment, HSP in these patients could not be predicted. Future research should devise a method of evaluating shoulder pain in patients with cognitive impairment.
In conclusion, more than half of the 94 stroke patients experienced moderate-to-severe shoulder pain during the first 6 months after a stroke. Impaired arm motor function and presence of supraspinatus tendon pathology at the acute stage of stroke were independent risk factors for HSP during the 6 months after stroke onset. The high-risk patients for HSP, with severe arm paralysis and/or supraspinatus tendon pathology, require more attention to the handling of their hemiplegic upper extremity during all stages of rehabilitation period after a stroke. In the acute stage after a stroke, rehabilitation programme should include exercises to maintain shoulder range of motion to prevent adhesive capsulitis. The therapies to reduce shoulder subluxation such as using arm trough or applying neuromuscular electrical stimulation are necessary during acute to subacute stages after a stroke (18). In the chronic stage after a stroke, consideration may be given to reducing the tone in the peri-shoulder muscles. And during all stages after a stroke, applying rehabilitative training to regain lost motor function is also important. Because the associated risk factors for HSP differed according to time after the stroke, future studies should address temporal aspects, such as stroke duration and the onset of HSP.
AcknowledgEments
This study was supported by an independent research grant to N. J. Paik from Daewoong Pharmaceutical Co. Ltd, through Seoul National University R&DB Foundation (grant number 800-20100031).
References
