OBJECTIVE: The International Classification of Functioning, Disability and Health (ICF) serves as a unifying model for rehabilitation medicine. Variables of the health status measurements, the Crohn’s Disease Activity Index and the Harvey-Bradshaw Index, have not been linked with the ICF categories and compared with other predictors of rehabilitation outcomes.
METHODS: Crohn’s Disease Activity Index variables were linked with ICF categories using linking rules. A chart review included the patients of our in-patient rehabilitation centre during one year (n = 355) with International Classification of Disease Codes for Crohn’s disease (ICD K50). We identified variables linked with clinical improvement (decrease in the Harvey-Bradshaw Index of ≥ 2 U) and rehabilitation success (conversion from unfit-to-work to fit-to-work) by multivariate logistic regression.
RESULTS: The ICF component, activities and participation, was not represented in the Crohn’s Disease Activity Index and the Harvey-Bradshaw Index. A Harvey-Bradshaw Index ≥ 5 U was associated with clinical improvement during rehabilitation (odds ratio 5.65 (95% CI 3.41–9.35)). Normal C-reactive protein (odds ratio 2.8 (95% CI 1.1–7.0)) and higher body mass index (odds ratio (per 1 kg/m2 increase) 1.1 (95% CI 1.0–1.2)), but not Harvey-Bradshaw Index, were associated with vocational rehabilitation success in 124 patients who were initially unfit-to-work.
CONCLUSION: Variables representing activities and participation as well as immune functions may improve Crohn’s disease health status measurements on the basis of better prediction of vocational rehabilitation success.
Key words: Crohn’s disease; Harvey-Bradshaw Index; Crohn’s Disease Activity Index; vocational rehabilitation; return to work; International Classification of Functioning, Disability and Health; gastroenterology; disability.
J Rehabil Med 2010; 42: 74–80
Correspondence address: Priv.-Doz. Dr. Christoph Reichel, Reha Zentrum Bad Brückenau, Klinik Hartwald, Schlüchterner Str. 4, DE-97769 Bad Brückenau, Germany. E-mail: christoph.reichel @web.de
Submitted March 12, 2009; accepted September 24, 2009
Introduction
The International Classification of Functioning, Disability and Health (ICF) is regarded as the unifying model for physical and rehabilitation medicine (PRM) (1, 2). The health status measures, the Crohn’s Disease Activity Index (CDAI) (3) and the Harvey Bradshaw Index (HBI) (4), have not been linked with ICF categories and rehabilitation outcomes. In addition, ICF factors associated with work disability and rehabilitation success have not been characterized in Crohn’s disease (CD). CD is characterized by an insidious onset in early adulthood and a relapsing and remitting course of discontinuous inflammations that may involve all regions of the gastrointestinal tract. Despite impairments in functional health the majority of patients with CD remain within the workforce and engage in gainful employment (5–14). Nevertheless, a considerable number of patients with CD are not able to maintain their tenure track, because of limitations in their physical and mental well-being and reduced energy levels. Accordingly, it has been shown that 17% of patients, as well as 11% of their partners, believe that CD compromises their professional career (15). Furthermore, employees with CD are absent from work more often than their healthy colleagues. In line with this, 50% of patients with CD were absent from work in a given year according to Mayberry et al. (16) and Pinchbeck et al. (17). Due to these impeding functional impairments, approximately 9% of all German employees with inflammatory bowel disease are engaged in in-patient medical rehabilitation each year (18). In other words, more than 3000 employees with inflammatory bowel disease followed rehabilitation procedures in Germany in 2004. A number of, mainly retrospective, studies have evaluated the employment and disability status of patients rehabilitated with inflammatory bowel disease (15, 16, 19–21). However, no attempts have been made to identify determinants of clinical improvements, work disability and vocational success in rehabilitation. Moreover, it is not known which ICF factors may be associated with work-ability and work-related outcomes in this patient group. Herein, we link the CD-specific health status measurements CDAI and HBI with ICF categories. Furthermore, we identify technical and clinical measurements associated with vocational rehabilitation success.
METHODS
Study design
This analysis was performed as part of a larger ongoing exploratory study into the characterization of medical rehabilitation in CD. In short, a single-centre cohort study was performed in a 228-bed in-patient rehabilitation centre where patients with gastrointestinal diseases from all regions of Germany are rehabilitated. Almost all rehabilitants were white-collar employees insured by the German Pension Insurance, Federal Office. A chart-review was performed of patients from the year 2006. We included all patients assigned to the International Classification of Disease (ICD) code K50 (Crohn’s disease) fulfilling the following predefined inclusion criteria: documented endoscopic, histological and laboratory signs of CD and complete data-sets. The study was approved by the ethics committee of the Bavarian board of physicians.
Parameters assessed
The following data were recorded: fitness/ability to work at the beginning and the end of in-patient rehabilitation, gender, age, duration of rehabilitation, smoking status, body mass index (BMI), ileocecal resection, fistulizing disease, stoma, duration of disease, prescription of systemic available corticosteroids, and C-reactive protein (CRP) on admission. Furthermore, we extracted the CDAI (3) from the files in the first week as well as the HBI (4) in the first and last weeks (Table I). Parameters such as CRP and BMI were assessed within 24 h after admission. In addition, we checked whether the patients fulfilled the diagnostic criteria for mild to moderate disease put forward by the American Gastroenterology Association (AGA) (22). Mild to moderate disease was defined as: ambulatory patients able to tolerate oral alimentation without manifestations of dehydration, toxicity (high fevers, rigors and prostration), abdominal tenderness, painful mass, obstruction, or > 10% weight loss. All rehabilitants took part in a standardized rehabilitation programme according to the German guidelines for rehabilitation in gastroenterology (23). The programme comprised weekly presentations on treatment options, aetiology and prognosis of CD, as well as an adapted programme of physical exercises offered 3 times a week. Additionally, psychological support and dietary counselling were part of the programme. A physician assessed the patients working status within 12 h after admission. The working status was assessed by screening available information from the pension insurance and health insurance accompanying the patient files. If no information was available from these sources the working status was recorded according to the patient’s statements. At the end of the rehabilitation programme a physician assessed the fitness-to-work/work-ability of the patient according to the current guidelines of the German association for rehabilitation of digestive and metabolic diseases (GRVS) (24).
| Table I. Linking variables and coefficients of Crohn’s Disease Activity Index (CDAI) and Harvey Bradshaw Index (HBI) with International Classification of Functioning, Disability and Health (ICF) categories |
| Variable | CDAI variable definitions* | ICF categories | CDAI coefficient, 1976† | HBI coefficient, 1980 |
| 1 | Number of liquid or very soft stools per day | Faecal consistency (b5251), Frequency of defecation (b5252) | 14 | 1 |
| 1-A | Adjustment if using diarrhoea-control medication | Drugs (e1101) | 30 | – |
| 2 | Abdominal pain rating (0–3) | Pain in stomach or abdomen (b28012) | 35 | 1 |
| 3 | General well-being rating (0–4) | Not definable-general health (nd-gh) | 49 | 1 |
| 4 | Number of 6 types, other occasional CD findings‡ | CD associated health conditions (hc)‡, Body temperature (b5500), Maintenance of body temperature (b5501) | 20 | 1 |
| 5 | Abdominal mass (CDAI = 0, 2, 5; HBI =1–4) | Structure of small intestine (s5400), Structure of large intestine (s5401), Additional information not contained in these categories is documented | 10 | 1 |
| 6 | Haematocrit, % decrease from expected | Production of blood (b4300), Oxygen-carrying functions of blood (b4301) | 6 | – |
| 7 | Body weight, % decrease from expected | Assimilation functions (b520) General metabolic functions (b540) Weight maintenance functions (b530) | 1 | – |
| Range of index values, these data: |
| | Low | | –27 | 0 |
| | High | | 662 | 19 |
| *HBI definitions are the same or similar. †Variables 1 through 3 for CDAI were changed here from 7-day total to average per day, and these coefficients were adjusted accordingly. HBI uses single-day values for these 3 variables. ‡List of occasional CD findings with ICF categories in brackets: arthritis (hc); skin lesions (hc); fever (body temperature (b5500); maintenance of body temperature (b5501)); anal fissures (hc); anal fistulas (hc); anal abscess (hc); other fistulas (hc); iritis or uveitis (hc). CD: Crohn’s Disease; hc: health condition. |
The result of the assessment was defined with the consent of the patient and the multi-professional rehabilitation team under the surveillance of the attending gastroenterologist trained in social medicine. Because we reviewed the charts for the year 2006 and the study started in 2007, the assessing rehabilitation team was not aware of the study’s objectives.
Linking Crohn’s disease health status measurements, clinical measures and interventions with the ICF
In short, we identified all meaningful concepts within each variable of the CD-specific health measures CDAI and HBI. Then we defined the aims with which technical or clinical measures were performed by applying the specific rules for health status, technical and clinical measures as previously described (25). In a second step we linked each meaningful concept and objective with the most precise ICF category, by applying the updated linking rules as put forward by Cieza and co-worker (25). The linking procedure was performed by physicians specialized in gastroenterological rehabilitation.
Statistics
For statistical analysis the SPSSTM software package (Chicago, USA) was used. Variables such as CDAI and HBI are given mean with standard deviation (SD). If not otherwise stated, numerical variables are given as mean with 95% confidence intervals (95% CI). Parameters associated with the outcomes studied were identified by a forward binary logistic regression analysis. Candidate variables with a p-value < 0.1 on univariate analysis were entered into the regression analysis. A p-value < 0.05 was considered significant. The results were expressed as odds ratios (OR) with 95% CI. The non-parametric Wilcoxon signed-rank test and the Mann-Whitney U test were used for inter-individual comparisons, as for most variables it is not known whether they are normally distributed. Frequencies were compared by the χ2 test, and p-values were Bonferroni corrected for multiple comparisons. BMI and CRP values in different patient groups were compared by analysis of variance (ANOVA) also using post-hoc Bonferroni correction. The performance of BMI and CRP as predictors of fitness-to-work at the end of rehabilitation was assessed by receiver operator curve (ROC) analysis. The non-parametric Spearman rho correlation coefficient (rS) was calculated to describe bivariate correlations between BMI and CRP. The Pearson correlation coefficient (rP) was calculated to describe correlations between BMI and CDAI.
Results
Patients
Overall, we screened 3113 files of rehabilitants scheduled for rehabilitation in our centre in 2006. Of 355 patients with ICD K50, 331 fulfilled the predefined inclusion criteria (Table II). Patients with disability pensions were not identified in our cohort. The mean age was 40 (SD 11) years. The study population comprised 85 men and 246 women, with a mean CDAI of 147 U (95% CI 36–285) and HBI 4.9 U (95% CI 1–11 U). The rehabilitation procedure had a mean duration of 23 (95% CI 20–34) days.
| Table II. Comparison of rehabilitants fit and unfit-to-work on admission (n = 331) |
| Working status (d845) | Fit-to-work n = 207 | Unfit-to-work n = 124 | p-value |
| Female gender, n (%) | 147 (71) | 99 (80) | 0.528† |
| Age, years, mean (95% CI) | 41 (39.6–42.5) | 38.6 (36.6–40.6) | 0.66° |
| BMI, kg/m2, mean (95% CI) | 24.6 (24.0–25.3) | 24.0 (22.9–25.1) | 0.45° |
| Smokers, n (%) | 65 (31) | 54 (44) | 0.363† |
| Duration of CD, years, mean (95% CI) | 11.1 (9.9–12.4) | 8.9 (7.2–10.6) | 0.044° |
| Ileocecal resection, n (%) | 66 (32) | 52 (42) | 0.825† |
| Fistulizing course of disease, n (%) | 58 (28) | 45 (36) | 1.0† |
| Crohn’s Disease Activity Index, mean (95% CI) | 130 (120–139) | 176 (163–189) | < 0.0011° |
| HBI ≥ 5/HBI < 5 Units, n | 89/118 | 75/49 | 0.022† |
| C-reactive protein, mg/dl, mean (95% CI) | 0.92 (0.73–1.10) | 1.23 (0.94–1.53) | 0.473° |
| Systemic steroid therapy, n (%) | 54 (26) | 60 (48) | < 0.0011† |
| †χ2 test; °Mann-Whitney U test. p-values are corrected for multiple comparisons (Bonferroni correction). CD: Crohn’s disease; CI: confidence interval; BMI: body mass index; HBI: Harvey-Bradshaw Index. |
Linking Crohn’s disease health status measures, clinical measures and interventions with the ICF
Table I shows the results of the linking process when applied to the CDAI and HBI variables. Overall, the 7 CDAI variable definitions were linked with 10 categories of body functions, 2 of body structures, one of environmental factors, and 8 health-related conditions. The CDAI variable “general well-being” could not be defined according to the fifth updated linking rule and was coded as “not definable-general health”. The clinical measure CRP was linked with the body function non-specific immune response (b43501), whereas BMI was linked with assimilation functions (b520), general metabolic functions (b540) and weight maintenance functions (b530). The clinical intervention steroid treatment was linked with drugs (e1101).
Parameters associated with clinical improvement in rehabilitation
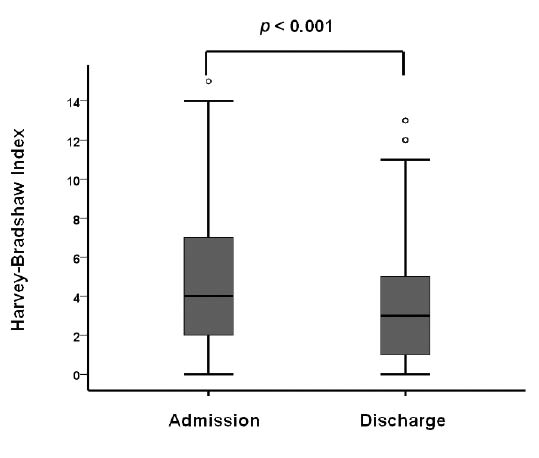
Overall, the HBI decreased significantly, from 4.9 U to 3.7 U, by 1.2 U (95% CI 0.7 U–1.7 U) (p < 0.001) during rehabilitation (Fig. 1). We therefore asked which parameters may be associated with a clinically relevant decline in disease activity in CD patients rehabilitated in our centre. In accordance with others we defined clinically relevant improvement as a HBI decline ≥ 2 U during rehabilitation, which equals an almost 70 U CDAI reduction in disease activity (26). Overall, we observed a clinically relevant improvement in 70 of 207 (34%) patients fit-to-work and 48 of 124 (39%) patients unfit-to-work on admission. Interestingly, the parameters female gender (OR 0.042) and duration of CD (OR 0.952) were inversely related to clinically successful rehabilitation in the univariate analysis (Table III). However, in contrast to a HBI ≥ 5 U (OR 5.65 (95% CI 3.41–9.35)) these parameters were not independently associated with clinical improvement in the multivariate analysis (Table III). Overall, a HBI ≥ 5 U (OR 5.65 (95% CI 3.41–9.35)) was the only parameter associated with clinical improvement during rehabilitation in the final model (Table III).
Fig. 1. The Harvey-Bradshaw Index on admission and discharge. The box-plots represent medians and quartiles. o: outliers.
| Table III. Univariate and multivariate analysis of parameters associated with clinical improvement in 331 patients with Crohn’s disease (CD) |
| Parameter | Univariate analysis | Multivariate analysis |
| OR (95% CI) | p-value | OR (95% CI) | p-value |
| Female gender | 0.54 (0.3–0.98) | 0.042 | – | ns |
| Age (per 1 year increase) | 1.02 (0.99–1.04) | 0.233 | | |
| BMI (per 1 kg/m2 increase) | 1.03 (0.99–1.08) | 0.149 | | |
| Smokers | 0.89 (0.521–1.53) | 0.676 | | |
| Duration of CD (years) | 0.952 (0.92–0.98) | 0.003 | – | ns |
| Ileocecal resection | 1.12 (0.622–2.00) | 0.713 | | |
| Fistulizing course of disease | 1.54 (0.87–2.72) | 0.139 | | |
| HBI ≥ 5 Units | 7.21 (4.08–12.75) | < 0.0001 | 5.65 (3.41–9.35) | < 0.0001 |
| C-reactive protein ≤ 0.8mg/dl | 1.05 (0.65–1.7) | 0.9 | | |
| Systemic steroid therapy | 1.00 (0.57–1.76) | 1.00 | | |
| Unfit-to-work on admission | 0.91 (0.52–1.58) | 0.736 | | |
| CI: confidence interval; BMI: body mass index; HBI: Harvey-Bradshaw Index, OR: odds ratio; ns: not significant. |
Parameters associated with work disability on admission
To identify parameters associated with work disability or unfitness to work on admission, we compared 207 individuals who were fit-to-work and 124 individuals who were unfit-to-work (Table II). As can be seen from Table II, the duration of CD was significantly shorter in patients who were unfit-to-work. As expected patients who were unfit-to-work had a significantly higher disease activity irrespective of the score used for assessment of disease severity (Table II). Moreover, the percentage of patients receiving systemic steroids was twice as high (48%) in patients who were unfit-to-work as amongst those who were fit-to-work (26%). This difference was highly significant even after correction for multiple testing (Table II).
For further characterization of parameters associated with unfitness to work we analysed all 10 variables shown in Table II in a univariate analysis followed by a multivariate analysis to identify independent predictors. As expected from the literature (26) HBI and CDAI were highly correlated (rP = 0.811 p < 0.0001), thus we chose HBI for further analysis. Moreover, disease activity HBI and CRP were entered as categorical variables stratified according to the cut-offs ≥ 5 U HBI and ≤ 0.8 mg/dl (normal value in our laboratory) respectively. Only 8 variables entered the multivariate analysis, as BMI and CRP did not fulfil the inclusion criteria for multivariate testing (Table IV). Of these, 4 parameters were found to be independently associated with unfitness to work on admission i.e. duration of CD (OR 0.96), history of ileocecal resection (OR 2.3), HBI ≥ 5 U (OR 2.4) and systemic steroid therapy (OR 3.1) (Table IV).
| Table IV. Univariate and multivariate analysis of parameters associated with work disability on admission in 331 patients with Crohn’s disease (CD) |
| Variable | Univariate analysis | Multivariate analysis |
| OR (95% CI) | p-value | OR (95% CI) | p-value |
| Female gender | 1.66 (0.95–2.75) | 0.077 | – | ns |
| Age (per 1 year increase) | 0.98 (0.96–1.0) | 0.05 | – | ns |
| BMI (per 1 kg/m2 increase) | 0.98 (0.94–1.02) | 0.382 | | |
| Smokers | 1.69 (1.06–2.67) | 0.026 | – | ns |
| Duration of CD (years) | 0.97 (0.95–0.98) | 0.036 | 0.96 (0.94–0.99) | 0.007 |
| Ileocecal resection | 1.54 (0.97–2.45) | 0.065 | 2.3 (1.4–4.0) | 0.002 |
| Fistulizing course of disease | 1.58 (0.95–2.60) | 0.076 | – | ns |
| HBI ≥ 5 Units | 2.10 (1.30 –3.38) | 0.002 | 2.4 (1.5–3.89) | 0.001 |
| C-reactive protein ≤ 0.8mg/dl | 0.8 (0.48–1.2) | 0.234 | | |
| Systemic steroid therapy | 2.95 (1.81–4.82) | < 0.0001 | 3.1 (1.9–5.1) | 0.0001 |
| CI: confidence interval; BMI: body mass index; HBI: Harvey-Bradshaw Index; OR: odds ratio; ns: not significant. |
Parameters associated with vocational success in rehabilitation
Of 124 patients who were unfit-to-work 33 converted to fit-to-work during the rehabilitation procedure, whereas 12 patients who were initially fit-to-work deteriorated to unfit-to-work. Work-ability remained unchanged in 286 patients. Overall, rehabilitation was associated with a significant conversion from unfit-to-work to fit-to-work if tested intra-individually (p = 0.002). Interestingly, only 14 out of 331 (4.2%) patients had applied for a disability pension before rehabilitation. To identify parameters associated with conversion from unfit-to-work to fit-to-work during rehabilitation, we performed a forward binary logistic regression analysis in 124 patients who were unfit-to-work on admission. From the parameters analysed BMI and CRP fulfilled the criteria for inclusion into the multivariate analysis. Both remained in the multivariate model (Table V). This means that both are independently associated with vocational success of rehabilitation (Table V). Next we assessed the performance of BMI and CRP as predictors of vocational success in rehabilitation by ROC analysis. As expected the areas under the curve (AUCs) were significantly different from 0.5 in both cases (BMI 0.638 (95% CI 0.535–0.741) (p = 0.019) and CRP 0.61 (95% CI 0.509–0.712) (p = 0.019)).
| Table V. Univariate and multivariate analysis of parameters associated with change from unable to able-to-work during rehabilitation in 124 patients with Crohn’s disease (CD) |
| Variable | Univariate analysis | Multivariate analysis |
| OR (95% CI) | p-value | OR (95% CI) | p-value |
| Female gender | 1.2 (0.4–3.4) | 0.757 | | |
| Age (per 1 year increase) | 1.0 (0.93–1.02) | 0.262 | | |
| BMI (per 1 kg/m2 increase) | 1.1 (1.0–1.2) | 0.003 | 1.1 (1.0–1.2) | 0.016 |
| Smokers | 1.6 (0.7–4.1) | 0.292 | | |
| Duration of CD (years) | 1.0 (0.96–1.07) | 0.908 | | |
| Ileocecal resection | 1.2 (0.4–3.2) | 0.723 | | |
| Fistulizing course of disease | 0.5 (0.2–1.5) | 0.232 | | |
| Harvey-Bradshaw Index on admission ≥ 5 Units | 0.4 (0.2–1.2) | 0.103 | | |
| C-reactive protein ≤ 0.8 mg/dl | 2.2 (1–5.2) | 0.078 | 2.8 (1.1–7.0) | 0.033 |
| Systemic steroid therapy on admission | 0.4 (0.2–1.1) | 0.132 | | |
| BMI: body mass index; OR: odds ratio. |
Body mass index, C-reactive protein and vocational outcomes
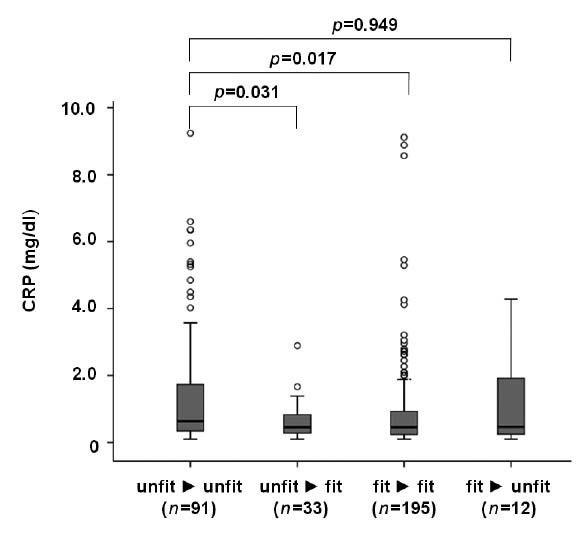
To corroborate these findings we studied the association of BMI and CRP with vocational outcomes of medical rehabilitation in more detail. For this we stratified the whole study population (n = 331) into 4 categories: patients who were persistently unfit-to-work on admission and discharge (n = 91), patients who were improving from initially unfit-to-work to fit-to-work on discharge (n = 33), patients who were persistently fit-to-work on admission and discharge (n = 195) and patients with deteriorating work-ability from initially fit-to-work to unfit-to-work on discharge (n = 12) (Fig. 2). Corroborating the findings from the multivariate analysis, the 99 persistently unfit-to-work patients had CRP levels twice as high 1.5 mg/dl (95% CI 1.06–1.84 mg/dl) as 33 initially unfit-to-work patients who improved to fit-to-work with mean CRP levels of 0.64 mg/dl (95% CI 0.43–0.84 mg/dl) (p = 0.031). The same was true of 195 patients who were persistently fit-to-work with average CRP levels of 0.9 mg/dl (95% CI 0.71–1.08 mg/dl), which were significantly lower than CRP levels in the above-mentioned 91 patients who were persistently unfit-to-work with 1.5 mg/dl (95% CI 1.06–1.84 mg/dl) (p = 0.017)) (Fig. 2). In addition, the average CRP levels did not differ significantly between the persistently unfit-to-work patients and those deteriorating from fit-to-work to unfit-to-work (Fig. 2). On the other hand, in 91 patients who were persistently unfit-to-work we found a lower mean BMI of 23 kg/m2 (95% CI 22–25 kg/m2) compared with 33 patients improving from unfit-to-work to fit-to-work with an average BMI of 26 kg/m2 (95% CI 24–28 kg/m2) and 195 patients who were persistently fit-to-work with a BMI of 25 kg/m2 (95% CI 24–26 kg/m2). However, in the case of BMI these differences were not significant. Interestingly, CRP and BMI correlated inversely with each other in the overall study population (n = 331) (rS = 0.131) (p = 0.017).
Fig. 2. C-reactive protein (CRP) levels, stratified according to vocational rehabilitation outcomes: patients persistently unfit-to-work on admission and discharge (n = 91), patients improving from initially unfit-to-work to fit-to-work on discharge (n = 33), patients persistently fit-to-work on admission and discharge (n = 195) and patients with deteriorating work ability from initially fit-to-work to unfit-to-work on discharge (n = 12). The box-plots represent medians and quartiles. o: outliers.
Discussion
Traditionally CDAI or HBI are used as CD-specific health status measures in gastroenterology. A good, albeit not perfect, relationship has been described between both indices (26). Until now it has been unclear how variables and coefficients of CDAI and HBI relate to ICF categories. As can be seen from Table I, most CDAI variables could be linked with the ICF components body functions and structures by applying the updated linking rules (25, 27). One important exception is the CDAI variable “general well-being”, which cannot be linked with a single ICF domain alone (1). Some limitations of ICF linking by linking rules have to be emphasized. The updated linking rules are based on 4 different applications: technical and clinical measures, health status measures and interventions (25). Thus, information from experts in Delphi exercises and patient’s statements may pose new aspects that are not covered by our approach (25). Despite this, our linking results demonstrate that a CDAI- and HBI-based measurement of disease activity and health status relies heavily on assessing body functions, body structures and CD-associated health conditions (Table I). This restriction may explain the fact that HBI, although associated with clinical rehabilitation success, was not associated with vocational rehabilitation outcomes in our study.
Overall, we observed a significant decrease in CD severity, by 1.2 U (95% CI 0.7–1.7 U) (p < 0.001), from 4.9 to 3.7 U, during rehabilitation (Fig. 1). As there was no control group in our study we were not able to establish a causal relationship between these clinical improvements and the rehabilitation process. However, the multivariate analysis revealed elevated disease severity (HBI ≥ 5 U) as the only independent predictor of clinical rehabilitation success (OR 5.65 (95% CI 3.41–9.35)) (Table III). This may be explained by the fact that a decrease of more than 2 U HBI may be easier to achieve in patients with elevated HBI levels. Such a direct correlation between rehabilitation effect and severity of initial impairment has been described in neurorehabilitation (28). However, our findings do indicate that even patients with higher HBI levels may profit from rehabilitation. Interestingly, the clinical success of rehabilitation was independent of work ability at the start of rehabilitation (OR 0.91 (95% CI 0.52–1.58) (p = 0.736) (Table III).
The association demonstrated in Table IV between shorter disease duration as well as ileocecal resection and work disability has been established in earlier studies (29). Additionally, it is known that quality of life, healthcare resource use and personal factors, such as work-related experience and behavioural patterns, are associated with disease severity in CD (30, 31). Moreover, it has been shown that treatment with systemic steroids is associated with a clinically significant reduction in health-related quality of life in CD (32). However, to our knowledge, this is the first time that the ICF-environmental factor therapy with systemic steroids has been independently associated with work ability. It is important to note that the association between steroid use and work disability was independent of disease severity (Table IV). Thus, steroid treatment itself may confer a barrier for an individual’s functioning in major life areas, such as maintaining employment in CD patients.
As can be seen in Table V, CRP and BMI were the only variables independently associated with vocational success. This is the first time that bio-markers have been associated with such a complex outcome as return-to-work (33–38). In previous research the importance of the individual’s expectations, the number of days of sick leave taken and a high level of life satisfaction and sense of coherence have been identified as predictors (35). As we did not assess psychological parameters and personal factors in our cohort we could not study CRP and BMI in comparison with such parameters.
Although we studied a large number of patients with CD all patients were white-collar employees. In addition, centre-specific attitudes in assessing fitness-to-work may have influenced our results. However, the accordance between pre-rehabilitation sick leave and working status recorded in the rehabilitation charts is known to be high. In addition, working status at discharge was always fixed in co-operation with the informed patient, as described in the GRVS guidelines (24). Consequently, the patient’s discontent was less than 1% in our centre according to external quality assessment data provided by the pension insurance. This does not differ from other centres and does not support the assumption of an assessment bias. However, results of multivariate regression analysis are known to be quite inert to selection and centre biases as well as bias inherent to the retrospective study design. Furthermore, our definition of vocational success as conversion from unfit-to-work to fit-to-work may not represent return-to-work. Although data in CD are lacking it has been shown in cardiac rehabilitation that 92% of patients discharged as fit-to-work successfully returned to work when assessed 6 and 12 months after rehabilitation in Germany (33). This indicates that conversion from unfit-to-work to fit-to-work may be used as a surrogate marker for return-to-work (34).
In addition, it may be argued that CRP and BMI have been identified as determinants of vocational rehabilitation success in a rather small subgroup of only 124 patients who were admitted as unfit-to-work (Table V). However, the results of this multivariate analysis were corroborated by the results of the comparison of CRP and BMI in all 331 patients with different vocational outcomes (Fig. 2).
In conclusion, the variables of the CD-specific health status measures CDAI and HBI could be successfully linked with ICF categories by applying the updated linking rules. The fact that a relevant ICF component such as “activities participation” is not represented in these outcome measurements may foster research to refine these scores for rehabilitation purposes by integrating this component. As an elevated HBI is independently associated with clinical improvement, patients should not be excluded from rehabilitation procedures due to elevated HBI levels alone. Finally, bio-markers, such as CRP and BMI, representing several ICF categories may be linked with complex outcomes such as return-to-work in patients with CD. This may facilitate the identification of worthwhile targets for the rehabilitation process and the improvement of CD-specific health status measures.
References