Elior Moreh, MD1, Zeev Meiner, MD1, Martin Neeb, BPT1, Nurith Hiller, MD2 and Isabella Schwartz, MD1
From the 1Department of Physical Medicine and Rehabilitation and 2Department of Radiology, Hadassah University Hospital, Jerusalem, Israel
Elior Moreh, MD1, Zeev Meiner, MD1, Martin Neeb, BPT1, Nurith Hiller, MD2 and Isabella Schwartz, MD1
From the 1Department of Physical Medicine and Rehabilitation and 2Department of Radiology, Hadassah University Hospital, Jerusalem, Israel
OBJECTIVE: To describe the rehabilitation outcome of a case of spinal decompression sickness presenting as partial Brown-Sequard syndrome treated with robotic-assisted body-weight support treadmill training.
Study design: Case report.
BACKGROUND: Type II decompression sickness patients commonly suffer from myelopathy with gait disturbances necessitating rehabilitation. Robotic-assisted body-weight support treadmill training has been shown to improve the rehabilitation outcome of incomplete spinal cord injury. Its usefulness has not been described in decompression sickness myelopathy.
METHODS: Robotic-assisted body-weight support treadmill training was administrated using the LokomatTM. Primary outcomes were American Spinal Cord Association scale, Spinal Cord Independence Measurement, Berg Balance Test, and Walking Index for Spinal Cord Injury.
RESULTS: The patient was admitted 3 weeks after the diving injury, with severe paraparesis and a T11 sensory neurological level, resembling partial Brown-Sequard syndrome. After 3 months of rehabilitation including 18 Lokomat sessions, American Spinal Cord Association score improved from C to D, Spinal Cord Independence Measurement improved from 50 to 90 out of 100. Berg Balance Test improved from 35 to 43 out of 56 and Walking Index for Spinal Cord Injury improved from 1 to 15 out of 20. Upon discharge he could walk with one crutch for more than 1 km.
CONCLUSION: Robotic-assisted body-weight support treadmill training for spinal decompression sickness rehabilitation might be beneficial.
Key words: decompression sickness, spinal cord injury, Brown-Sequard syndrome, physical therapy modalities.
J Rehabil Med 2009; 41: 88–89
Correspondence address: Elior Moreh, Department of Physical Medicine and Rehabilitation, Hadassah Mount Scopus University Hospital, POB IL-24035, Jerusalem IL-91420, Israel. E-mail: elior@hadassah.org.il
Submitted April 8, 2008; accepted June 27, 2008
INTRODUCTION
Decompression sickness (DCS) is caused by an alteration in environmental pressure that results in the release of previously dissolved inert gas bubbles into tissue or blood (1). Scuba divers with type II DCS most commonly suffer from myelopathy with gait disturbances and need rehabilitation treatment. Locomotor therapy by robotic-assisted body-weight support treadmill training (BWSTT) is evolving as a promising method in the rehabilitation of partial spinal cord injured patients (2). Its usefulness has not been described previously in DCS myelopathy.
CASE REPORT
A 42-year-old experienced diver felt sharp thoracic back pain when climbing into the boat from the water. Shortly afterwards, he developed progressive weakness and numbness of his lower limbs. On admission to the emergency room he presented with flaccid paraplegia, hypoesthesia below T11 and flaccid bladder. Treatment with hyperbaric oxygen and intravenous methylprednisolone were started, with a total of 15 recompression treatments. Magnetic resonance imaging (MRI) revealed non-enhancing hyperintense T2 foci in the posterior mid and posterior right aspect of the cord at levels T5–6, T7–8, consistent with ischaemic insult (Fig. 1). Upon admission to rehabilitation, 3 weeks after the injury, he had severe spastic paraparesis, grade C according to the American Spinal Cord Association (ASIA) Scale. Neurological examination revealed spasticity grade 2/4 on the modified Ashworth scale, 1/5 weakness in the right leg and 3–4/5 weakness in the left leg, a diminished fine touch sensation below the level of T11, more prominent on the left, and impaired proprioception more prominent on the right. Motor and pin-prick sensory ASIA scores were 70/100 (right 26/50, left 44/50) and 84/112 (right 46/56, left 38/56), respectively. He had a urinary catheter and a flaccid rectal sphincter. The clinical picture corresponded to partial Brown-Sequard syndrome at the level of T11 on the right and his Spinal Cord Independence Measurement (SCIM) score was 50 out of 100.
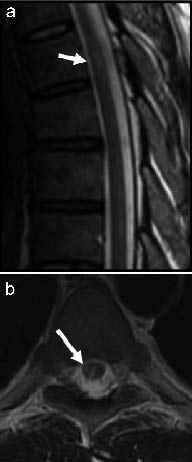
Fig. 1. Magnetic resonance imaging in (a) sagittal and (b) axial T2 weighted images demonstrating a hyperintense intramedullary lesion at the level of D5–D6.
Concomitantly with conventional physiotherapy, he was treated with robotic-assisted BWSTT (LokomatTM, Hocoma, Swiss) twice a week for 18 treatments with no complications. Following the treatment, significant improvement was revealed in locomotor parameters, including reduction of body weight support from 60% at the beginning to 0% at the end and marked improvement in walking velocity and duration.
On discharge, after 3 months of treatment, muscle strength in the lower limbs improved to 3–4/5 on the right and 4–5/5 on the left. His neurological condition according to ASIA scale improved from C to D. ASIA motor score improved to 89/100 (right 42/50, left 47/50). He reached complete independence in transfers and basic activities of daily life and his SCIM improved to 90 out of 100. He still needed to perform clean intermittent catheterizations 4 times a day and his bowel movements were pharmaceutically regulated. He could walk independently with crutches for long distances, and climb stairs near a ramp. His balance improved from 35 out of 56 according to the Berg Balance Test on admission to 43 upon discharge. His Walking Index for Spinal Cord Injury (WISCI) score improved from 1 out of 20 on admission to 15 upon discharge, meaning an improvement from walking a few steps between parallel bars with the aid of 2 persons, to walking with one crutch, a brace and no physical assistance for at least 10 m. Functionally he was able to walk for long distances with one crutch.
DISCUSSION
The patient’s symptoms of backache after surfacing from his dive, with progression to lower extremity numbness and paralysis, are consistent with myelopathy secondary to type II DCS (1). Brown-Sequard syndrome is an unusual manifestation of DCS described in only one case report with correspondent lesion on MRI (3). The overall prognosis of spinal cord injury secondary to DCS is good. In one series of 68 patients with spinal cord DCS, full recovery was reached in 79% (1). However, most patients had milder symptoms and showed resolution of symptoms within one month after recompression therapy. In another series of 60 DCS patients, 22% had residual symptoms one month after the injury, and 11.8% remained symptomatic after 6 months (4). Moreover, 5 out of 8 patients with severe DCS still showed prominent limb weakness and sensory loss 6 months after the injury, reflecting a worse prognosis of patients with severe DCS on presentation.
Locomotor treatment using robotic-assisted BWSTT was proved to be effective in partial spinal cord injury, with faster and greater mobility improvement demonstrated with a combined treadmill training and conventional physiotherapy vs conventional physiotherapy alone (5). The rationale of its use is evidence of use-dependent neuroplasticity in the spinal cord, at the level of spinal locomotor centres. Our patient had severe paraparesis on admission 3 weeks after the injury, reflecting a worse prognosis than the general prognosis of DCS myelopathy. Nevertheless, his condition improved markedly after 3 months of rehabilitation treatment including robotic-assisted BWSTT. Robotic-assisted BWSTT for spinal DCS rehabilitation might thus be beneficial.
REFERENCES
1. Aharon-Peretz J, Adir Y, Gordon C, Kol S, Gal N, Melamed Y. Spinal cord decompression sickness in sport diving. Arch Neurol 1993; 50: 753–756.
2. Wirz M, Zemon DH, Rupp R, Scheel A, Colombo G, Dietz V, et al. Effectiveness of automated locomotor training in patients with chronic incomplete spinal cord injury: a multicenter trial. Arch Phys Med Rehabil 2005; 86: 672–680.
3. Kimbro T, Tom T, Neuman T. A case of spinal cord decompression sickness presenting as partial Brown-Sequard syndrome. Neurology 1997; 48: 1454–1456.
4. Dick PK, Massey EW. Neurologic presentation of decompression sickness and air embolism in sport divers. Neurology 1985; 35: 667–671.
5. Dietz V, Wirz M, Colombo G. Locomotor pattern in paraplegic patients: training effects and recovery of spinal function. Spinal Cord 1998; 36: 380–390.
